Folliculitis
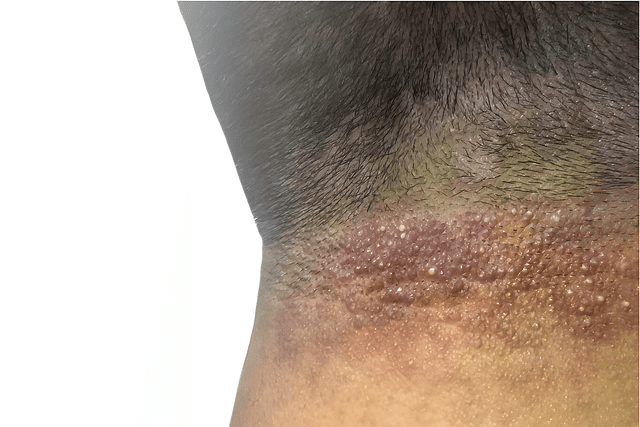
Folliculitis develops when hair follicles become inflamed or infected by bacteria, fungi, viruses, or physical irritation. It typically appears as small, red, inflamed bumps resembling acne and can occur on various parts of the body, including the face, scalp, arms, back, legs, and even the buttocks. The condition can cause discomfort, itching, or tenderness, and in some cases, the bumps may fill with pus, leading to more noticeable irritation. Mild cases usually resolve with home care, while more severe cases may require treatment by a dermatologist.
Last updated on : 14 Apr, 2026
Read time : 12 mins
Overview of Disease
Folliculitis is an inflammatory condition that targets hair follicles. It can manifest as an acute, short-term issue or a chronic, long-term problem. The severity of folliculitis ranges from mild to severe, with milder cases often resolving spontaneously without treatment. However, more severe cases may require medical intervention to prevent complications such as scarring and irreversible hair loss. In this article, we will delve deeper into the causes, types, symptoms, and treatment options for this condition.
What is Folliculitis?
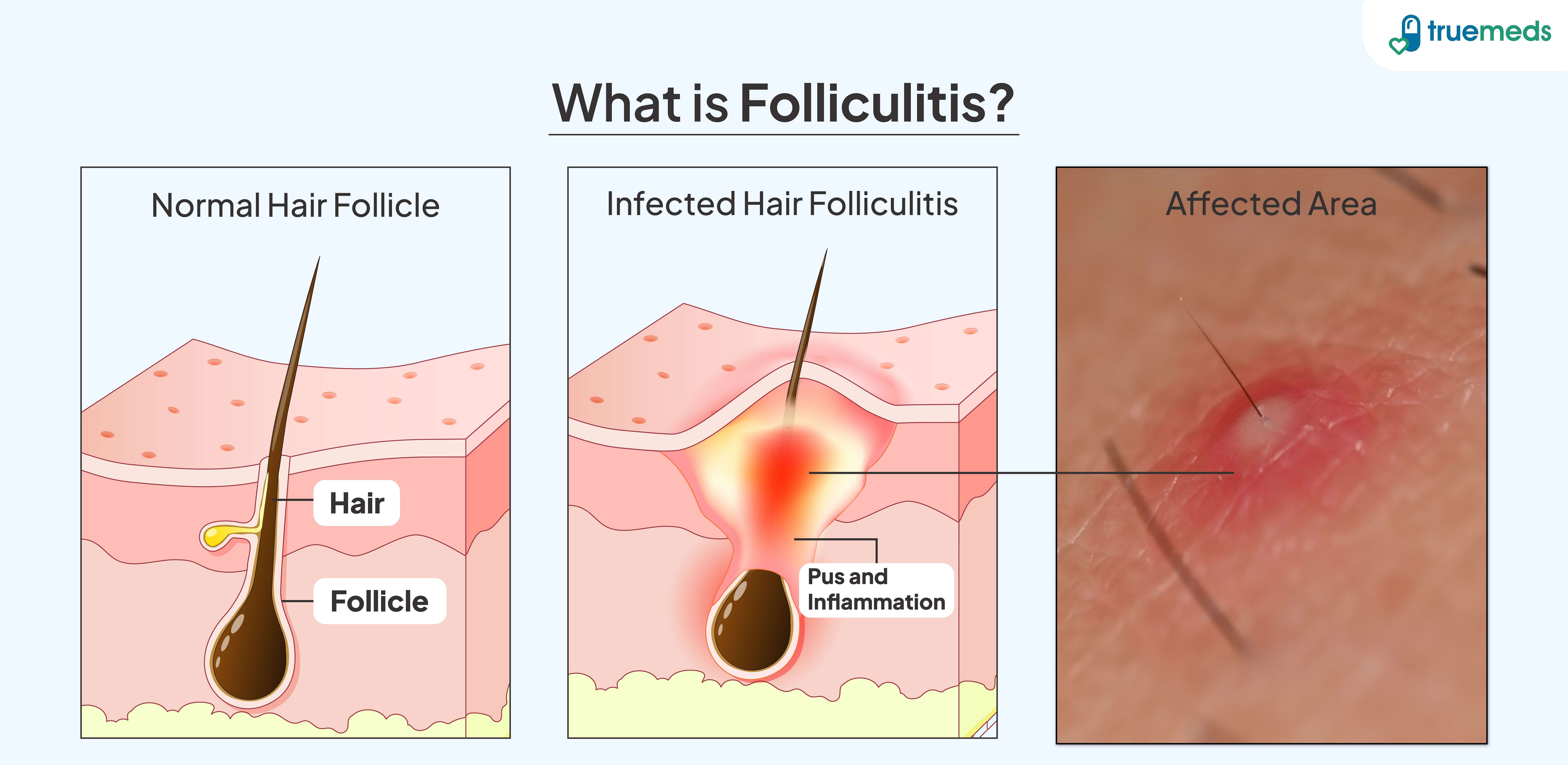
Folliculitis is a common skin condition where hair follicles become inflamed, often due to a bacterial infection. It usually appears as small red bumps or pus-filled pimples around the hair follicles, resembling acne. The condition can be itchy, painful, or cause a burning sensation, and in some cases, it may spread and form crusty sores.
Most cases of folliculitis resolve on their own within 7 to 10 days with basic self-care, such as keeping the affected area clean and avoiding irritants. However, severe or recurrent cases may require prescription medications, including antibiotics or antifungal treatments. If left untreated, severe folliculitis can lead to scarring and permanent hair loss.
Key Factors about Folliculitis
| Category | Details |
| Also Referred as | Barber's itch, hot tub rash, razor bumps, shaving rash, pseudofolliculitis barbae, tinea barbae |
| Commonly Occurs In | Neck, thighs, buttocks, armpits, face, arms, back, legs |
| Affected Organ | Hair follicles |
| Type | Superficial folliculitis, deep folliculitis, bacterial folliculitis, hot tub folliculitis (pseudomonas folliculitis), pityrosporum folliculitis, folliculitis decalvans, malassezia folliculitis, eosinophilic folliculitis, viral folliculitis |
| Common Signs | Red bumps, itchy bumps, pus-filled sores, crusty sores, inflamed skin, tender bumps |
| Consulting Specialist | Dermatologist, primary care physician |
| Treatment Procedures | Topical antibiotics, oral antibiotics, antifungal medicines, warm compresses, surgical incision and drainage (for deeper infections) |
| Managed By | Antibiotic creams (mupirocin), oral antibiotics (clindamycin, cephalexin, dicloxacillin, doxycycline, trimethoprim-sulfamethoxazole, or ciprofloxacin), oral antifungal (fluconazole, itraconazole), oral antiviral medications (acyclovir) |
| Mimicking Condition | Guttate psoriasis, acne, hidradenitis suppurativa |
Types of Folliculitis
The two main types of folliculitis include:
- Superficial folliculitis: This classification type involves the hair follicle and is typically caused by bacteria (Staphylococcus aureus), such as hot tub folliculitis and yeast infections (Pityrosporum folliculitis).
- Deep folliculitis: This classification type involves the entire hair follicle and presents more severe symptoms, including sycosis barbae (Barber's itch), gram-negative folliculitis, eosinophilic folliculitis, and instances where hair follicles become deeply infected and present painful and swollen boils (furuncles) or carbuncles (clusters of boils, which may rupture and drain).
Within these two categories, there are several subtypes:
- Bacterial folliculitis: Caused by bacteria, most commonly Staphylococcus aureus, and presents as pustules, often without symptoms of fever.
- Hot tub folliculitis (pseudomonas folliculitis): Caused by Pseudomonas aeruginosa and typically occurs after swimming in a pool or sitting in a hot tub where pH or chlorine levels are not balanced (Winters & Mitchell, 2023).
- Pityrosporum folliculitis: Caused by a yeast infection, typically affecting the upper body, and results in itchy, pus-filled pimples.
- Folliculitis decalvans: A rare type of scalp folliculitis leading to hair loss due to long-term bacterial inflammation (Singh et al., 2025).
- Malassezia folliculitis: Caused by the yeast Malassezia, which is naturally found on the skin, and can lead to an itchy acne-like condition, especially in oily skin.
- Razor bumps (pseudofolliculitis barbae): Occur when shaved hair grows back into the skin, causing inflammation and bumps, commonly affecting the beard area.
- Sycosis barbae: A type of deep folliculitis affecting the beard area, causing painful, pus-filled bumps.
- Gram-negative folliculitis: A rare type of folliculitis caused by gram-negative bacteria, often occurring after long-term antibiotic treatment for acne.
- Boils and carbuncles: Severe forms of folliculitis where hair follicles become deeply infected, resulting in painful, pus-filled bumps that may require medical intervention.
Recognising the various types of folliculitis is crucial for accurate diagnosis and targeted treatment, which may involve a combination of self-care measures, topical or oral medications, and lifestyle changes to prevent recurrence.
Symptoms of Folliculitis
Folliculitis symptoms depend on the severity of the infection. Here are common signs:
- Red bumps or pimples: Small, red, inflamed bumps form around hair follicles, often looking like acne and feeling tender.
- Itching or burning: The affected area may feel itchy or burn.
- Pus-filled blisters: In severe cases, bumps may turn into blisters that break open and ooze fluid.
- Crusting or scabbing: As blisters heal, they may form scabs or crust over.
- Pain or discomfort: The area can be sore, especially if infected or irritated.
- Swelling and inflammation: The surrounding skin may become swollen and inflamed.
Causes of Folliculitis
Folliculitis occurs when hair follicles become infected or inflamed. The most common cause is bacterial infection, particularly by Staphylococcus aureus. In addition to viral, fungal, and parasitic infections can also lead to folliculitis. Certain medications or physical injury from shaving or friction can also lead to folliculitis. The main causes include:
- Bacterial infection: The most common cause of folliculitis is a bacterial infection, particularly by Staphylococcus aureus. This bacterium can enter the hair follicle through cuts or irritation.
- Fungal infection: Fungi, such as those that cause tinea (ringworm), can also cause folliculitis. This type is more common in warm, moist environments.
- Viral infection: Certain viruses, including the herpes simplex virus, can cause folliculitis. This may be seen in conditions like herpes outbreaks.
- Ingrown hairs: When hair grows back into the skin instead of out, it can lead to inflammation and folliculitis, especially in areas prone to shaving or friction.
- Irritation from shaving or waxing: Frequent shaving or waxing can irritate hair follicles, making them more susceptible to inflammation and infection.
- Blocked follicles: Excess oil, sweat, or dirt can clog hair follicles, leading to inflammation. This is often exacerbated by tight clothing or excessive friction.
- Certain medications: Antibiotics and corticosteroids can alter the skin’s natural flora, increasing the risk of folliculitis.
- Underlying skin conditions: Conditions such as acne, eczema, or dermatitis can contribute to folliculitis by compromising the skin barrier.
- Immune system factors: Individuals with weakened immune systems may be more susceptible to infections, including those that cause folliculitis.
Risk Factors
Certain factors can increase the likelihood of developing folliculitis,including:
- Regularly wearing tight, moisture-trapping clothing
- Using unclean or poorly maintained hot tubs and pools
- Shaving, especially with improper techniques or unclean tools
- Having a weakened immune system due to conditions like diabetes, HIV/AIDS, or undergoing chemotherapy
- Using certain medications, such as corticosteroid creams or long-term antibiotic therapy for acne
- Having dermatitis or excessive sweating (hyperhidrosis)
Who's at Risk?
Some individuals are at a higher risk of developing folliculitis, including:
- Individuals with compromised immune systems, such as those with diabetes, HIV/AIDS, or cancer
- People who frequently use hot tubs or pools, or engage in activities that cause excessive sweating
- Those who wear tight, constrictive clothing or use heavy, occlusive skin products
- Individuals who shave regularly, especially if they use improper techniques or unclean tools
Recognising these at-risk groups can aid early detection and treatment of folliculitis, as well as the implementation of preventive strategies.
Complications
While folliculitis is often a mild and self-limiting condition, it can lead to several complications if left untreated or if recurrent episodes occur. Here are some potential complications:
- Skin infections: Persistent or severe folliculitis can lead to deeper skin infections, such as cellulitis, which may require more aggressive treatment.
- Scarring: Repeated inflammation of hair follicles can lead to scarring, especially if the area is frequently scratched or irritated.
- Abscess formation: In some cases, folliculitis can progress to an abscess — a painful collection of pus that may require drainage and antibiotics.
- Post-inflammatory hyperpigmentation: The skin may develop darkened areas or spots after folliculitis resolves, particularly in individuals with darker skin tones.
- Chronic folliculitis: Some individuals may experience recurrent bouts of folliculitis, leading to chronic inflammation and ongoing discomfort.
- Hair loss: Severe or chronic folliculitis can damage hair follicles, potentially resulting in temporary or permanent hair loss in the affected areas.
If you experience symptoms of folliculitis or notice any complications, it is important to consult a doctor for an appropriate diagnosis and treatment.
Prevention of Folliculitis
Taking proactive measures can help reduce the risk of developing folliculitis. Here are some effective prevention strategies:
- Maintain good hygiene: Regularly washing the skin with mild soap can help remove dirt, oil, and bacteria that may clog hair follicles. It is essential to cleanse areas prone to sweating.
- Avoid tight clothing: Wearing loose-fitting clothing can minimise friction and irritation on the skin, reducing the chances of folliculitis developing in areas where hair follicles are more vulnerable.
- Practice safe shaving: Use clean, sharp razors and shave in the direction of hair growth to help prevent ingrown hairs and irritation. Consider using shaving cream or gel to protect the skin.
- Avoid hot tubs and pools: Recreational water sources can harbour bacteria and fungi. If using hot tubs or pools, ensure they are well-maintained and avoid using them if you have an open wound or an active infection.
- Moisturise regularly: Keeping the skin hydrated can help maintain its barrier function, making it less susceptible to infections and irritation.
- Limit hair removal methods: If prone to folliculitis, consider alternatives to shaving, such as depilatory creams or laser hair removal, which may cause less irritation.
- Address underlying skin conditions: Managing acne or eczema with a doctor can reduce the risk of folliculitis.
- Be cautious with personal items: Avoid sharing towels, razors, or clothing, as they can spread bacteria and increase the risk of infection.
By following these preventive measures, you can significantly reduce your risk of developing folliculitis and maintain healthier skin.
Diagnosis & Tests
Diagnosing folliculitis typically involves a combination of clinical evaluation and, in some cases, laboratory tests. These include:
- Medical history: The doctor will start by discussing your medical history, including any prior episodes of folliculitis, underlying skin conditions, and recent activities that may have contributed to the condition, such as shaving or using a hot tub.
- Physical examination: A thorough physical examination of the affected area is essential. The doctor will look for characteristic signs of folliculitis, such as red bumps, pustules, and any signs of irritation or infection.
- Skin culture: If the infection is severe, recurrent, or does not respond to initial treatment, the doctor may take a sample from the affected area for culture. This can help identify the specific bacteria or fungi causing the folliculitis.
- Biopsy: In rare cases, a skin biopsy may be performed to rule out other skin conditions or to determine the exact cause of persistent folliculitis.
- Blood tests: If there is concern about an underlying immune system condition or if systemic treatment is needed, blood tests may be performed.
Treatment & Management
Medications Based on the Cause of Folliculitis
1. Staphylococcal Folliculitis
- Treated with topical antibiotics such as mupirocin and clindamycin to combat bacterial infections.
- Oral antibiotics like doxycycline, cephalexin, dicloxacillin,or trimethoprim + sulfamethoxazole may be prescribed for more severe cases.
2. Gram-Negative Folliculitis
- Managed with oral antibiotics, including ampicillin, trimethoprim + sulfamethoxazole, or ciprofloxacin, to control bacterial overgrowth.
3. Pityrosporum Folliculitis
- Typically treated with oral antifungal agents such as fluconazole and itraconazole, which help eliminate fungal infections affecting hair follicles.
4. Viral Folliculitis
- Requires oral antiviral medications, including acyclovir, valacyclovir, or famciclovir, to suppress viral infections causing folliculitis.
5. Demodex Folliculitis
- Treated with topical permethrin, an anti-parasitic agent targeting mite infestations.
- Oral anti-parasitic agents such as ivermectin and metronidazole may be required for more persistent infections.
6. Eosinophilic Folliculitis
- Managed with antiretroviral therapy (ART), including zidovudine, stavudine, and lamivudine, especially in immunocompromised individuals.
- Topical corticosteroids like hydrocortisone help reduce inflammation.
- Antihistamines such as diphenhydramine may be used to control itching and discomfort.
- Additional treatments may include phototherapy (UVA/UVB exposure), itraconazole, or isotretinoin for resistant cases.
When to See a Doctor?
If your folliculitis symptoms worsen or persist for more than five days, it is essential to see a doctor, especially if you notice signs of severe infection, such as increased redness, swelling, or pus. If self-care measures like washing with antibacterial soap and applying over-the-counter treatments do not improve your condition, consult a doctor. Additionally, seek medical advice if you experience hair loss or scarring, as your doctor can identify the underlying cause and recommend an effective treatment plan.
Key Takeaways
- Folliculitis is often caused by bacterial infections, particularly Staphylococcus aureus, as well as fungal infections, ingrown hairs, and other factors like friction from tight clothing or shaving.
- Symptoms of folliculitis include red, itchy, and sometimes painful bumps or pus-filled blisters around hair follicles.
- Diagnosis of folliculitis is typically based on a physical examination and review of symptoms, but skin swabs or biopsies may be necessary for persistent or severe cases.
- Treatment options for folliculitis include topical and oral antibiotics, antifungal medications, and home remedies like warm compresses and saltwater soaks.
- Prevention measures, such as good hygiene, avoiding tight clothing, and proper shaving techniques, can help reduce the risk of developing folliculitis.
- If symptoms persist or worsen despite home treatment, it is important to consult a doctor for proper diagnosis and treatment to prevent complications.
FAQs
What triggers folliculitis?
What treatments are effective in killing folliculitis-causing bacteria?
Which skin conditions are often misdiagnosed as folliculitis?
How to remove folliculitis from skin?
What kills folliculitis naturally?
Which antibiotics are good for folliculitis?
Which cream treats folliculitis?
Is there a permanent cure for folliculitis?
What is the best antifungal for folliculitis?
Can folliculitis spread by scratching?
References
- Adil, M., & Amin, S. S. (2022). Folliculitis. In StatPearls. StatPearls Publishing. https://www.ncbi.nlm.nih.gov/books/NBK547754/
- American Academy of Dermatology Association. (2023). Folliculitis: Overview. https://www.aad.org/public/diseases/a-z/folliculitis
- MedlinePlus. (2020). Folliculitis. https://medlineplus.gov/ency/article/000823.htm
- Singh, G., Pathania, Y., Goswami, P., Tyagi, S., & Patel, T. (2025). Folliculitis decalvans: An uncommon case report with review of literature. International Journal of Applied and Basic Medical Research, 15(1),63–65.https://doi.org/10.4103/ijabmr.ijabmr_414_24
Latest health articles
Top Health Essentials
Disclaimer
Top-Selling Medicines:
...View more
Top-OTC medicines:
...View more
Company
About UsHealth ArticleHealth StoriesHealth LibraryDiseases & Health ConditionsAyurvedaUnderstanding Generic MedicinesAll MedicinesAll BrandsNeed HelpFAQSecuritySavings CalculatorSubscribe
Registered Office Address
Grievance Officer
Download Truemeds
Contact Us
Our customer representative team is available 7 days a week from 9 am - 9 pm.
v4.23.1
2026 - Truemeds | All rights reserved. Our content is for informational purposes only. See additional information.
Our Payment Partners
















































