Diabetic Foot Ulcers
Diabetic foot ulcers are a serious complication of diabetes, causing open wounds on the feet due to factors like high blood sugar, poor circulation, nerve damage, and immune system issues. They can progress through various stages, from superficial ulcers to extensive gangrene, and require prompt treatment to prevent amputation.
Last updated on : 07 Apr, 2026
Read time : 11 mins
Overview of Disease
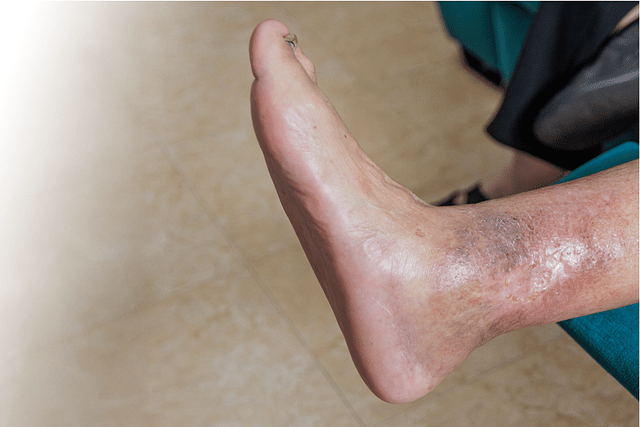
Diabetic foot ulcers are a prevalent and potentially severe complication affecting approximately one-third of individuals with diabetes (Kilic et al., 2025). These open wounds develop on the feet due to a combination of factors, including elevated blood sugar levels, poor circulation, nerve damage, and foot irritation or injury. Prompt recognition and treatment of diabetic foot ulcers are crucial to prevent progression and reduce the risk of amputation.
What are Diabetic Foot Ulcers?
Diabetic foot ulcers are open sores on the feet of people with diabetes that occur when the skin tissue breaks down, exposing the underlying layers. These ulcers can arise from a lack of sensation or blood flow in the affected area, often resulting from prolonged high blood sugar levels that damage blood vessels and nerves throughout the body.
The development of these ulcers involves multiple factors, such as neuropathy, peripheral artery disease (PAD), foot deformities, other diabetes-related complications, and obesity.
Key Factors about Diabetic Foot Ulcers
| Category | Details |
| Also Referred as | DFUs |
| Commonly Occurs In | People with diabetes, commonly affecting the bottom of the foot, especially the plantar surface |
| Affected Organ | Feet, specifically the skin, nerves, and blood vessels |
| Common Signs | Open sore or wound, lack of feeling, poor circulation, foot deformities, signs of infection (redness, swelling, warmth) |
| Consulting Specialist | Podiatrist, vascular surgeon, infectious disease specialist |
| Managed By | Wound care, pressure offloading, antibiotics, vascular care (bypass surgery or endovascular procedures), blood sugar control, proper foot care, regular monitoring |
Symptoms of Diabetic Foot Ulcers
The symptoms of diabetic foot ulcers can vary, but may include the following:
- Swelling, redness, and warmth around the wound
- A foul odour from the ulcer
- Drainage from the affected area
- Skin discolouration
- Visible bone or tendons in the wound bed
- Callused or thickened skin surrounding the ulcer
- Pain around the callused or irritated region
- Fever or chills, indicating a systemic infection
Stages of Diabetic Foot Ulcers
The progression of diabetic foot ulcers can be classified using various systems, but one commonly used method is the Wagner Ulcer Classification System (Shah et al., 2022):
- Stage 0 (No Open Lesions): At this stage, there may be evidence of a healed lesion, but no open wounds are present.
- Stage 1 (Superficial Ulcer): A superficial ulcer develops without penetrating the deeper layers of the skin.
- Stage 2 (Deeper Ulcer): The ulcer extends to the tendon, bone, or joint capsule.
- Stage 3 (Deeper Tissues Involved): The ulcer involves deeper tissues, possibly with an abscess, osteomyelitis, or tendinitis.
- Stage 4 (Gangrene): Gangrene develops in a portion of the forefoot or heel.
- Stage 5 (Extensive Gangrenous Involvement): The entire foot is affected by extensive gangrene.
Causes of Diabetic Foot Ulcers
Diabetic foot ulcers can arise due to a combination of factors. Some of the causes of diabetic foot ulcers are listed below:
- High Blood Sugar Levels: High blood glucose levels, which are characteristic of diabetes, can stiffen arteries and narrow blood vessels, restricting blood and oxygen delivery needed for healing.
- Neuropathy: Neuropathy (nerve damage), also caused by uncontrolled blood sugar levels, can lead to a loss of sensation, making it difficult for individuals to notice minor injuries or irritation on their feet.
- Poor Blood Circulation: Poor circulation due to PAD further impairs the body's ability to heal, as restricted blood flow to the feet deprives tissues of the oxygen and nutrients needed for repair.
- Pre-existing Wounds: Any existing wounds or irritation on the feet, such as minor cuts, blisters, or surgical wounds, can significantly increase the risk of developing diabetic foot ulcers.
Risk Factors
The following is a list of risk factors for diabetic foot ulcers:
- High blood sugar levels
- Nerve damage (neuropathy)
- Poor circulation
- Previous history of ulcers or amputation
- Irritated or wounded feet
- Foot deformities
- Older age
- Smoking
- Obesity
- Hypertension
- Poor foot hygiene
- Improper trimming of toenails
- Alcohol consumption
- Eye, kidney, or heart disease
Complications
If left untreated, diabetic foot ulcers can lead to severe complications, such as:
- Infection: Infection is a significant concern, as high blood sugar levels and poor circulation can make it difficult for the body to fight off bacteria.
- Amputation: In extreme cases, amputation may be necessary if the ulcer does not heal and becomes severely infected.
- Prolonged Healing Time: Diabetic foot ulcers often take longer to heal due to the underlying metabolic and circulatory issues.
- Recurrence: Even after an ulcer has healed, there is a risk of recurrence if proper preventive care is not maintained.
- Hospitalisation: In some cases, hospitalisation may be required to manage complications arising from diabetic foot ulcers.
Prevention of Diabetic Foot Ulcers
Preventing diabetic foot ulcers is crucial for avoiding serious complications. Key strategies include:
- Daily Foot Inspection: Check your feet every day for redness, pain, blisters, cuts, or other sores. Use a mirror or ask a caregiver for help if needed.
- Proper Foot Care: Wash feet daily in warm water and dry gently, especially between the toes. Gently rub callus-prone areas with a pumice stone. Apply moisturiser to the tops and soles of your feet to keep your skin soft.
- Wear Comfortable, Well-fitting Shoes: Wear shoes that support the heel, arch, and ball of the foot. Avoid tight, high-heeled, or narrow shoes. Consider specialist orthopaedic footwear if advised.
- Nail Care: Trim toenails straight across, avoiding the corners. File sharp edges. If you have reduced sensation, see a podiatrist regularly for nail care.
- Maintain a Healthy Lifestyle: You can manage diabetes well through a healthy diet, regular exercise, blood sugar monitoring, and correct medication use. Controlling blood sugar, blood pressure, and cholesterol helps prevent many diabetic complications.
Apart from the points mentioned above, avoid walking barefoot, using adhesive tape on your feet, managing corns/calluses yourself, or using hot water bottles or foot warmers. Also, avoid tight socks or stockings that reduce blood flow.
Diagnosis & Tests
Diagnosing diabetic foot ulcers combines clinical examination and specific tests:
- Clinical Examination: During routine check-ups, a doctor will carefully inspect the foot for signs of ulcers, redness, swelling, or other abnormalities.
- Screening for Protective Sensation Loss: Tools like the Semmes-Weinstein monofilament are used in primary care to identify patients at risk of foot ulceration.
- Neuropathy Assessment: Neuropathy is quantified using biothesiometry. Lower limb vascular status is assessed with Doppler ultrasound and the ankle-brachial pressure index.
- Imaging: X-rays, magnetic resonance imaging (MRI), or computed tomography (CT) scans may be used to evaluate bone involvement if osteomyelitis is suspected.
- Wound Culture: If the ulcer appears infected, a tissue sample or swab may be taken to identify the microorganisms present and guide antibiotic therapy.
- Blood Tests: Testing for blood sugar, markers of infection, and other parameters helps guide overall treatment of diabetic foot ulcers.
Treatment & Management
Managing diabetic foot ulcers requires a multidisciplinary approach that focuses on wound healing, infection control, and the prevention of complications.
Wound care
Wound care includes cleaning the ulcer, removing dead tissue (debridement), and applying dressings that promote a moist healing environment. Offloading pressure from the affected area using total contact casts, removable boots, or custom orthotic devices is essential to aid recovery.
Infection control
Infection control is critical; topical or systemic antibiotics, such as amoxicillin/ clavulanate, clindamycin, ciprofloxacin, or metronidazole, may be used depending on the severity and type of infection. In severe cases, intravenous antibiotics like piperacillin-tazobactam or meropenem may be necessary.
Here is how these medicines work:
- Amoxicillin + Clavulanate: Broad-spectrum antibiotic combination that treats polymicrobial infections by inhibiting bacterial cell wall synthesis and overcoming resistance via beta-lactamase inhibition.
- Clindamycin: Lincosamide antibiotic effective against anaerobes and gram-positive cocci; inhibits bacterial protein synthesis.
- Ciprofloxacin: Fluoroquinolone antibiotic that targets gram-negative organisms by inhibiting bacterial DNA gyrase, preventing DNA replication.
- Metronidazole: Effective against anaerobic bacteria and protozoa; disrupts bacterial DNA, leading to cell death.
- Piperacillin + Tazobactam: A broad-spectrum IV antibiotic combination that covers severe polymicrobial infections; inhibits bacterial cell wall synthesis and beta-lactamase enzymes.
- Meropenem: A carbapenem antibiotic used in resistant or severe infections; inhibits bacterial cell wall synthesis, effective against a wide range of organisms.
Vascular care
Vascular care is essential if poor blood flow is contributing to the development of the ulcer. This may involve revascularisation procedures, such as angioplasty or bypass surgery.
Tight blood glucose control is achieved with medications such as metformin, insulin, or DPP-4 inhibitors. These medicines work in the following way:
- Metformin: An oral antidiabetic medicine that lowers blood glucose by reducing hepatic glucose production and improving insulin sensitivity.
- Insulin: Hormone therapy that lowers blood glucose levels directly by facilitating cellular glucose uptake.
- DPP-4 Inhibitors (e.g., Sitagliptin): Help lower blood sugar by increasing incretin levels, which inhibit glucagon release and increase insulin secretion.
For infected or non-healing ulcers, advanced therapies such as topical growth factors, skin substitutes, or negative-pressure wound therapy may be used.
Patient education on daily foot inspection, hygiene, proper footwear, and prompt reporting of new symptoms is vital. Regular monitoring by a diabetic foot specialist ensures proper healing and helps prevent recurrence.
Living with Diabetic Foot Ulcers
Living with diabetic foot ulcers requires diligent care, regular monitoring, and a comprehensive management plan to prevent complications and improve quality of life. You can consider the following tips to live with and manage the condition:
- Daily foot care is essential, including checking your feet daily for cuts, redness, swelling, sores, blisters, corns, calluses, or other changes to the skin or nails. Use a mirror if you can not see the bottom of your feet, or ask a family member to help.
- Wash your feet every day in warm (not hot) water, dry them thoroughly, and apply moisturiser to the top and bottom of your feet, avoiding the area between your toes to prevent infection.
- Never go barefoot; always wear shoes, socks, or slippers, even indoors, to avoid injury. Ensure the lining of your shoes is smooth and free of objects that could cause harm.
- Wearing shoes that fit well and provide good support is also essential, and specialised footwear may be necessary to reduce pressure on the wound and aid healing.
- Keeping blood glucose levels within the target range is crucial for wound healing and preventing further complications. High blood sugar levels can lead to problems with circulation, nerves, and the immune system, all of which can hinder the healing process of diabetic foot ulcers.
- Regular medical check-ups are essential when living with diabetic foot ulcers. Get your feet checked at every visit with your doctor, and visit your foot doctor every year (more often if you have nerve damage) for a complete exam that includes checking your foot sensation and blood flow.
- Lifestyle modifications, such as following a healthy eating plan and engaging in regular physical activity, can improve overall health and help manage diabetes effectively. Activities such as walking, biking, or swimming are recommended, but consult your doctor to determine the best activities for your condition.
When to See a Doctor?
It is critical to seek medical attention promptly if you notice any of the following signs or symptoms of diabetic foot ulcers:
- Redness, swelling, or warmth around a wound
- Foul-smelling discharge or coloured pus from the wound
- Pain or firmness in the affected area
- Fever or chills, which may indicate an infection
- New or worsening wounds on the feet
- Changes in skin colour or temperature
- Calluses or corns that are not resolving with home treatment
- Ingrown toenails or fungal infections
Key Takeaways
- Diabetic foot ulcers are open sores that occur on the feet of people with diabetes when the skin tissue breaks down, exposing the underlying layers.
- They can progress through various stages, from superficial ulcers to extensive gangrene, and require prompt treatment to prevent amputation.
- The development of these ulcers involves multiple factors, including neuropathy, PAD, foot deformities, other diabetes-related complications, and obesity.
- You can prevent this condition to a great extent by practising regular foot care, wearing comfortable, well-fitting shoes, and maintaining a healthy lifestyle.
FAQs
What is the most effective approach to managing diabetic foot ulcers?
What are the different phases of progression in diabetic foot ulcers?
How severe is a stage 3 diabetic foot ulcer?
Which topical treatment is most suitable for diabetic foot ulcers?
How severe can diabetic foot ulcers become?
What types of antibiotics are recommended for managing diabetic foot ulcers?
What are the initial signs of foot ulcers in people with diabetes?
References
- Armstrong, D. G., Boulton, A. J. M., & Bus, S. A. (2017). Diabetic foot ulcers and their recurrence. New England Journal of Medicine, 376(24), 2367-2375. https://doi.org/10.1056/NEJMra1615439
- Boulton, A. J. (2008). The diabetic foot: Grand overview, epidemiology and pathogenesis. Diabetes/Metabolism Research and Reviews, 24(S1), S3-S6. https://doi.org/10.1002/dmrr.833
- Jeffcoate, W. J., Vileikyte, L., Boyko, E. J., Armstrong, D. G., & Boulton, A. J. M. (2018). Current challenges and opportunities in the prevention and management of diabetic foot ulcers. Diabetes Care, 41(4), 645-652. https://doi.org/10.2337/dc17-1836
- Schaper, N. C., Van Netten, J. J., Apelqvist, J., Bus, S. A., Hinchliffe, R. J., & Lipsky, B. A. (2019). Practical guidelines on the prevention and management of diabetic foot disease (IWGDF 2019 update). Diabetes/Metabolism Research and Reviews, 36(S1), e3266. https://doi.org/10.1002/dmrr.3266
- Voelker, R. (2023). What are diabetic foot ulcers? JAMA, 330(23), 2314. https://doi.org/10.1001/jama.2023.17291
- Kilic, M., Olgun, N., Dündar, M., Advan, S. C., Kücük, F. Z., Okcuoglu, S., Sahin, S., Bicer, E. K., Ülker, Y., Sahin, P., & Taskiran, Z. (2025). Prevalence, risk level and risk factors of diabetic foot ulcer among adult individuals with diabetes in the Southeastern Anatolia Region of Turkiye. Journal of Tissue Viability, 34(1), 100839. https://doi.org/10.1016/j.jtv.2024.12.003
- Shah, P., Inturi, R., Anne, D., Jadhav, D., Viswambharan, V., Khadilkar, R., Dnyanmote, A., & Shahi, S. (2022). Wagner’s classification as a tool for treating diabetic foot ulcers: Our observations at a suburban teaching hospital. Cureus. https://doi.org/10.7759/cureus.21501
Latest health articles
Top Health Essentials
Disclaimer
Top-Selling Medicines:
...View more
Top-OTC medicines:
...View more
Company
About UsHealth ArticleHealth StoriesHealth LibraryDiseases & Health ConditionsAyurvedaUnderstanding Generic MedicinesAll MedicinesAll BrandsNeed HelpFAQSecuritySavings CalculatorSubscribe
Registered Office Address
Grievance Officer
Download Truemeds
Contact Us
Our customer representative team is available 7 days a week from 9 am - 9 pm.
v4.22.3
2026 - Truemeds | All rights reserved. Our content is for informational purposes only. See additional information.
Our Payment Partners
















































