Interstitial Nephritis
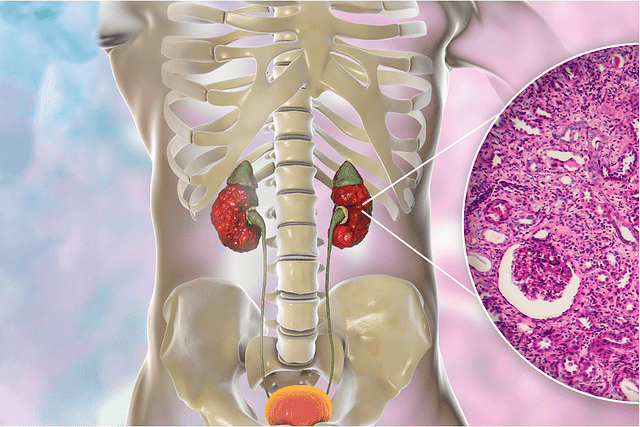
Interstitial nephritis is a kidney condition characterised by inflammation of the renal interstitium, the tissue and space around the renal tubules. This inflammation can impair the kidneys' ability to filter waste and excess fluids from the blood, leading to various symptoms and complications (Yu et al., 2025). Interstitial nephritis can be acute or chronic and requires prompt diagnosis and treatment to prevent permanent kidney damage.
Last updated on : 28 Apr, 2026
Read time : 10 mins
Overview of Disease
Interstitial nephritis, also known as tubulointerstitial nephritis, is a significant kidney condition that affects millions of people worldwide. While not as well-known as other kidney diseases, such as kidney stones or chronic kidney disease, interstitial nephritis can have serious consequences if left untreated. In this article, we will discuss the causes, symptoms, diagnosis, and treatment options for interstitial nephritis, providing you with the information needed to understand and manage this condition effectively.
What is Interstitial Nephritis?
Interstitial nephritis is a type of kidney inflammation that specifically targets the interstitium, which is the tissue surrounding the tiny tubules within the kidneys. These tubules are responsible for filtering waste products from the blood and regulating the body's fluid and electrolyte balance. When the interstitium becomes inflamed, it can disrupt the normal function of the kidney tubules, leading to various symptoms and complications.
Key Factors about Interstitial Nephritis
| Category | Details |
| Also Referred to as | Tubulointerstitial nephritis |
| Commonly Occurs In | Adults, children |
| Affected Organ | Kidneys (renal interstitium, tubules) |
| Type | Acute, chronic |
| Common Signs | Changes in urine output, fever, rash, nausea, vomiting, fatigue, appetite changes, breathing problems, flank pain, painful urination, and, in some cases, high blood pressure. |
| Consulting Specialist | Nephrologist (primary specialist) |
| Treatment Procedures | Stopping agents that induce interstitial nephritis, corticosteroids, dialysis, and kidney transplantation |
| Managed By | Corticosteroids |
| Mimicking Condition | Pyelonephritis, other kidney diseases, systemic inflammatory conditions (sarcoidosis) |
Types of Interstitial Nephritis
Interstitial nephritis can be classified into two types:
- Acute interstitial nephritis: This form develops suddenly and is often caused by an allergic reaction to a medication, such as antibiotics, nonsteroidal anti-inflammatory drugs, or proton pump inhibitors.
- Chronic interstitial nephritis: This form develops gradually over months or years and is usually associated with long-term exposure to certain toxins, infections, or underlying health conditions like autoimmune disorders.
The severity of interstitial nephritis can vary from mild to severe, depending on the extent of inflammation and damage to the kidney tubules.
Symptoms of Interstitial Nephritis
The symptoms of interstitial nephritis can vary and may develop suddenly or gradually. Some key symptoms to be aware of include:
- Reduced urine output: A decrease in urine output is a sign of acute kidney injury, which can occur in interstitial nephritis and requires prompt medical attention (Swathy et al., 2025).
- Increased urine output: In some cases, you may produce excessive urine, especially at night (nocturia), and experience frequent urination.
- Nausea and vomiting: These are common symptoms that often occur along with a decrease in appetite.
- Fever and rash: A fever and rash can indicate an allergic reaction, which may cause interstitial nephritis.
- Itchiness: You may experience itchiness, particularly in chronic cases, which may be associated with symptoms of kidney failure.
- Fatigue and confusion: Due to the buildup of waste products in your blood, you may feel tired and confused.
- High blood pressure: Kidney damage from interstitial nephritis can lead to high blood pressure.
- Breathing difficulties: In severe cases, fluid buildup can cause respiratory issues.
Causes of Interstitial Nephritis
Interstitial nephritis can be triggered by various factors that provoke an immune response or an allergic reaction. The primary causes include:
- Medications: Different medications can potentially induce interstitial nephritis. Common culprits include antibiotics like methicillin, non-steroidal anti-inflammatory drugs, proton pump inhibitors used for acid reflux, and certain cancer immunotherapies called immune checkpoint inhibitors.
- Infections: Bacterial infections such as E. coli, viral infections like HIV and herpes, sexually transmitted infections like syphilis, parasitic infestations, and fungal infections can all lead to interstitial nephritis by triggering inflammation in the kidneys.
- Autoimmune disorders: Conditions where the immune system mistakenly attacks the body's tissues, such as sarcoidosis, Sjögren's syndrome, and lupus, are associated with an increased risk of developing interstitial nephritis.
- Environmental factors: Exposure to certain toxins or receiving radiation therapy can damage the kidneys and cause inflammation, characteristic of interstitial nephritis.
- Chronic conditions: Chronic underlying conditions, such as diabetes or hypertension, can cause chronic interstitial nephritis over time.
Risk Factors
Various factors can increase an individual's risk of developing interstitial nephritis. These include:
- Exposure to certain medications: Medications such as antibiotics (penicillins, cephalosporins, sulfonamides), nonsteroidal anti-inflammatory drugs, proton pump inhibitors, and diuretics are common culprits in medication-induced acute interstitial nephritis. People taking these medications for prolonged periods or at high doses are at higher risk.
- Having an autoimmune disorder: Conditions such as Sjögren's syndrome, systemic lupus erythematosus, and IgG4-related disease can lead to chronic interstitial nephritis as part of their disease process.
- Experiencing infections: Bacterial, viral, or fungal infections can trigger interstitial nephritis, especially in immunocompromised individuals.
- Exposure to toxins: Exposure to certain toxins, such as heavy metals like lead and cadmium, can damage the kidneys and cause interstitial nephritis.
- Having a family history: Some genetic conditions, such as Alport syndrome and Fabry disease, can lead to progressive interstitial nephritis.
- Older age: The risk of developing interstitial nephritis increases with age, possibly due to age-related changes in kidney function and increased medication use.
Diagnosis & Tests
Diagnosing interstitial nephritis involves a combination of clinical evaluation, laboratory tests, and imaging studies. Here is a closer look at the diagnostic approach:
1. Clinical Evaluation
- Clinical evaluation: A detailed medical history is taken to identify potential causes of interstitial nephritis, including medication use and exposure to toxins. The doctor will also perform a physical examination to look for signs of kidney disease, such as swelling, rash, or changes in blood pressure.
2. Laboratory Tests
- Blood tests: Blood tests are used to detect signs of kidney failure, such as elevated waste products (urea and creatinine), metabolic acidosis, and electrolyte imbalances. These tests can help assess the severity of the condition.
- Urine tests: Urine tests are performed to analyse the urine for abnormalities, including protein, blood, and white blood cells. The presence of these substances in the urine can indicate kidney inflammation.
- Kidney biopsy: A kidney biopsy is the definitive diagnostic test for interstitial nephritis. During this procedure, a small sample of kidney tissue is removed and examined under a microscope to confirm the diagnosis and determine the extent of the inflammation.
3. Imaging Studies
- Imaging tests: Imaging tests may be recommended to visualise your kidneys and rule out other potential causes of your symptoms:
- Ultrasound: This non-invasive test uses sound waves to create images of your kidneys, helping to identify any structural abnormalities or obstructions.
- CT scan or MRI: These advanced imaging techniques provide more detailed pictures of your kidneys and can help detect inflammation or scarring.
Treatment & Management
The treatment approach for interstitial nephritis, whether acute or chronic, depends mainly on the underlying cause, the severity of the condition, and whether kidney function is compromised. Prompt diagnosis and appropriate intervention are crucial for preserving kidney function and preventing the progression to chronic kidney disease.
1. Discontinuation of the Offending Agent
In cases of medicine-induced acute interstitial nephritis (AIN), which is the most common cause, immediate withdrawal of the offending medication is the first and most crucial step. Stopping medications like NSAIDs, PPIs, antibiotics, anticonvulsants, or diuretics helps reverse medicine-induced acute interstitial nephritis by removing the trigger causing kidney inflammation.
Common causative agents include:
- NSAIDs (e.g., ibuprofen, naproxen)
- Proton pump inhibitors (PPIs) (e.g., omeprazole, pantoprazole)
- Antibiotics (e.g., penicillins, cephalosporins, rifampin, ciprofloxacin, sulfonamides)
- Anticonvulsants (e.g., phenytoin, carbamazepine)
- Diuretics (e.g., furosemide, thiazides)
2. Corticosteroids
Glucocorticoids (such as prednisone or methylprednisolone) are commonly used when kidney function does not improve after discontinuation of the causative agent, or in immune-mediated or idiopathic cases. Evidence supports their use, though optimal dosing and duration remain under investigation (Yu et al., 2025).
- Prednisone or Methylprednisolone: Steroids help reduce inflammation, especially in allergic or autoimmune forms of interstitial nephritis.
3. Additional Immunosuppressive Therapy
In steroid-resistant or severe cases, especially with autoimmune causes such as Sjögren’s syndrome, sarcoidosis, lupus nephritis, or TINU syndrome, immunosuppressants such as mycophenolate mofetil or cyclophosphamide may be used, though evidence is limited and individualised according to KDIGO (2025).
- Cyclophosphamide, Azathioprine, Mycophenolate mofetil, Rituximab, Methotrexate: Suppress the overactive immune system in resistant or immune-mediated interstitial nephritis, helping to preserve kidney function.
4. Supportive Care
Managing complications and preserving kidney function is crucial:
- Antihypertensive agents: To control elevated blood pressure
- ACE inhibitors (e.g., enalapril, lisinopril): Lower blood pressure and reduce protein loss in urine, protecting the kidneys.
- ARBs (e.g., losartan, valsartan): These also lower blood pressure and reduce protein loss in urine.
- Diuretics (e.g., furosemide, torsemide) to manage fluid overload
- Electrolyte correction: Hyperkalemia, acidosis, and phosphate disturbances may need tailored correction with:
- Sodium bicarbonate: Corrects metabolic acidosis caused by impaired renal acid excretion.
- Potassium binders (e.g., sodium polystyrene sulfonate or patiromer): Lower high potassium levels commonly seen in kidney dysfunction.
- Low-sodium and low-protein diet: Helps manage hypertension and reduce nitrogenous waste build-up.
5. Dialysis
Indicated in cases with:
- Severe acute kidney injury (AKI) unresponsive to medical therapy
- Fluid overload, refractory hyperkalemia, or uremia
- Dialysis is typically temporary in AIN but may become long-term if irreversible kidney damage occurs.
6. Kidney Transplantation
In patients progressing to end-stage renal disease (ESRD) due to chronic interstitial nephritis, a kidney transplant may be considered as a definitive treatment. Management of the underlying disease is still necessary post-transplant.
7. Long-Term Monitoring and Management
- Regular monitoring of renal function (serum creatinine, eGFR, urine protein)
- Avoidance of nephrotoxic agents
- Managing chronic conditions such as autoimmune disorders or infections
- In chronic interstitial nephritis, slow progression can be achieved with:
- ACE inhibitors/ARBs
- Strict blood pressure and glycemic control
When to See a Doctor?
If you suspect that you or someone else is experiencing symptoms of interstitial nephritis, it is crucial to seek medical attention promptly. Symptoms that warrant immediate medical evaluation include:
- Decreased or increased urine output
- Fever
- Rash
- Blood in the urine
- Nausea and vomiting
- Swelling and weight gain due to fluid retention
- Mental status changes, such as drowsiness or confusion
If you are taking medications and notice any of these symptoms, it is essential to inform your doctor immediately. Early recognition and discontinuation of the offending medication are critical for preventing long-term kidney damage. If you have already been diagnosed with interstitial nephritis and experience new or worsening symptoms, such as a decrease in urine output or increased confusion or alertness changes, it is important to seek medical advice without delay.
Key Takeaways
- Early recognition and intervention are critical for preventing permanent kidney damage, with prompt discontinuation of offending agents and timely corticosteroid therapy improving outcomes.
- Your doctor will conduct a thorough medical history and physical examination and may order laboratory tests such as blood chemistry, urinalysis, and possibly a kidney biopsy to confirm the diagnosis and guide treatment.
- If you suspect that you may have interstitial nephritis based on your symptoms or risk factors, do not hesitate to contact your doctor for a proper evaluation and appropriate management of your condition.
FAQs
What causes interstitial nephritis?
What are the three classic symptoms of interstitial nephritis?
How is interstitial nephritis treated?
Which medications are commonly associated with causing interstitial nephritis?
Is it possible to cure nephritis?
What are the common symptoms of nephritis?
References
- Swathy, R., Ramachandran, N., Srinivas, B. H., & Priyamvada, P. S. (2025). Clinicopathological spectrum and outcomes in patients with acute interstitial nephritis. Indian Journal of Nephrology. https://www.researchgate.net/publication/395281292_Clinicopathological_Spectrum_and_Outcomes_in_Patients_with_Acute_Interstitial_Nephritis
- KDIGO. (2025). KDIGO 2025 Clinical Practice Guideline for the Management of Glomerular Disease. https://doi.org/10.1016/j.kint.2025.04.003
- Muhammad, A., et al. (2024). The diagnosis of acute interstitial nephritis caused by infection. Clinical Kidney Journal, 17(4), sfae054. https://doi.org/10.1093/ckj/sfae054
- ERA. (2025). Immune profiling of checkpoint inhibitor–induced nephritis reveals distinct subtypes. European Renal Association 2025 Congress. https://www.emjreviews.com/nephrology/news/era-2025-immune-profiling-of-checkpoint-inhibitor-induced-nephritis-reveals-distinct-
- Yu, Y., et al. (2025). A systematic review of treatment for acute interstitial nephritis. Kidney International Reports, 10(5), 1003–1015. https://doi.org/10.1016/j.ekir.2025.03.012
Check Related Salts
Browse Other Conditions
Latest health articles
Top Health Essentials
Disclaimer
Top-Selling Medicines:
...View more
Top-OTC medicines:
...View more
Company
About UsHealth ArticleHealth StoriesHealth LibraryDiseases & Health ConditionsAyurvedaUnderstanding Generic MedicinesAll MedicinesAll BrandsNeed HelpFAQSecuritySavings CalculatorSubscribe
Registered Office Address
Grievance Officer
Download Truemeds
Contact Us
Our customer representative team is available 7 days a week from 9 am - 9 pm.
v4.23.0
2026 - Truemeds | All rights reserved. Our content is for informational purposes only. See additional information.
Our Payment Partners
















































