Chronic kidney disease
Chronic kidney disease (CKD) is a gradual loss of kidney function over time, leading to complications such as high blood pressure, anaemia, and bone disease. CKD is often a silent disease with no noticeable symptoms in its early stages, but as it progresses, symptoms may include foamy urine, changes in urinary frequency, fatigue, and swelling in extremities. The causes of CKD include diabetes, high blood pressure, and inherited conditions such as polycystic kidney disease.
Last updated on : 22 Apr, 2026
Read time : 19 mins
Overview of Disease
Chronic kidney disease (CKD) is a condition that affects millions of people worldwide. It is a progressive disease that occurs when the kidneys become damaged and lose their ability to filter waste and excess fluids from the blood effectively. CKD can lead to a wide range of health problems, including high blood pressure, anaemia, bone disease, and cardiovascular disease. If left untreated, CKD can progress to kidney failure, also known as end-stage renal disease (ESRD), which requires dialysis or a kidney transplant to sustain life. Understanding the causes, symptoms, and stages of CKD is crucial for early detection and effective management of the condition.
What is Chronic Kidney Disease?
Chronic kidney disease is a condition defined by abnormalities of kidney structure or function present for at least 3 months, with health implications (for example, persistent reduction in GFR and/or increased albuminuria), according to KDIGO (2024). The kidneys are vital organs that play a crucial role in filtering waste and excess fluids from the blood, regulating blood pressure, producing hormones, and maintaining the balance of electrolytes in the body. When the kidneys become damaged, they lose their ability to perform these functions effectively, leading to a build-up of waste and fluids in the body. CKD can be caused by a variety of factors, including diabetes, high blood pressure, glomerulonephritis, polycystic kidney disease, and prolonged use of certain medications. Early detection and management of CKD are essential to prevent the progression of the disease and reduce the risk of complications.
Key Factors about Chronic kidney disease
| Category | Details |
| Also Referred as | Chronic Renal Failure (CRF), End-Stage Renal Disease (ESRD) |
| Commonly Occurs In | Diabetics, Hypertensives, Elderly, People with Family History of Kidney Disease |
| Affected Organ | Kidneys |
| Type | Chronic, Progressive Disease |
| Common Signs | Fatigue, Swelling, Nausea, Vomiting, Loss of Appetite, Headaches, Muscle Cramps, Shortness of Breath, Pale Skin, Dull Skin, Itching, Sleep Problems |
| Consulting Specialist | Nephrologist |
| Treatment Procedures | Dialysis, Kidney Transplant, Medications for Managing Symptoms and Underlying Conditions |
| Managed By | ACE inhibitors like enalapril, lisinopril, and ramipril; ARBs such as losartan, valsartan, and telmisartan; Diuretics, including furosemide, torsemide, and metolazone; Statins, like atorvastatin, rosuvastatin, and simvastatin; Phosphate binders (such as sevelamer and calcium acetate) |
| Mimiciking Condition | Heart Failure, Liver Disease, Anaemia |
Symptoms of Chronic kidney disease
Chronic kidney disease often progresses slowly, and symptoms may be subtle or even absent in the early stages. However, as the disease advances, patients may experience:
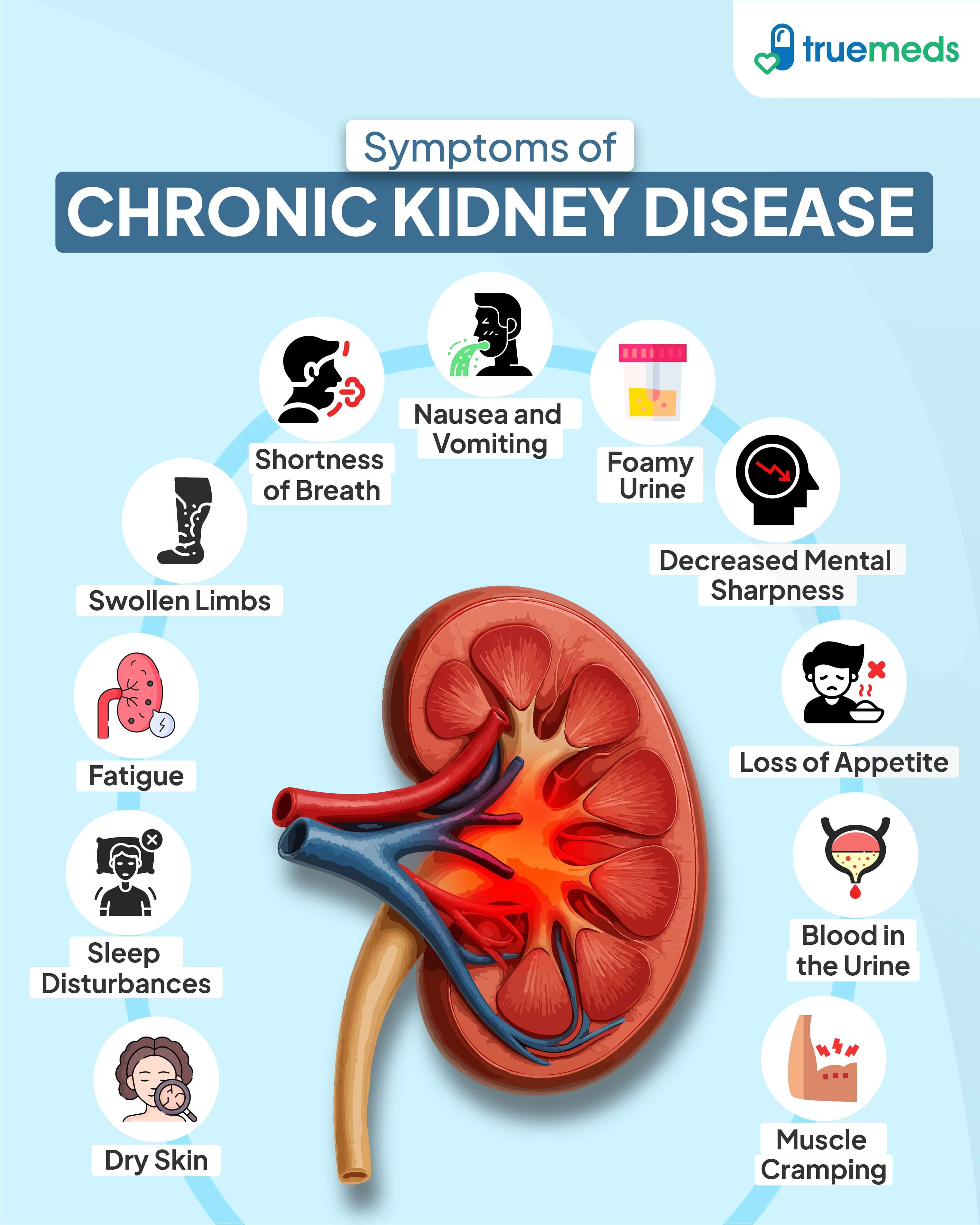
- Fatigue: Feeling constantly tired or weak is a common symptom of chronic kidney disease. This happens because the kidneys are not effectively removing toxins from the body, leading to persistent exhaustion.
- Swollen Limbs: Swelling in the ankles, feet, or hands occurs when the kidneys are unable to regulate fluid and sodium levels. This fluid retention results in noticeable swelling in the limbs.
- Shortness of Breath: Difficulty breathing may occur due to fluid buildup in the lungs. When the kidneys cannot manage excess fluid, it can accumulate in the lungs, causing breathing difficulties.
- Nausea and Vomiting: Nausea and vomiting are often caused by the accumulation of waste products in the body. As kidney function declines, these waste materials can upset the stomach.
- Loss of Appetite: A decreased interest in food is a symptom of chronic kidney disease. The buildup of toxins can reduce appetite, making it difficult to maintain a normal eating routine.
- Sleep Disturbances: Difficulty sleeping can result from discomfort and conditions like sleep apnoea. Fluid retention and other symptoms can interfere with the ability to get restful sleep.
- Foamy Urine: Foamy urine can indicate that protein is leaking into the urine, which is a sign of kidney damage. The kidneys are not filtering proteins properly, leading to this appearance in the urine.
- Blood in the Urine: Seeing blood in the urine suggests that the kidney filters are damaged. This leakage of blood cells into the urine is a sign of underlying kidney issues.
- Dry Skin: Dry skin can be a result of waste buildup in the body. When the kidneys are not functioning well, it can lead to dryness and irritation of the skin.
- Muscle Cramping: Muscle cramps may occur due to imbalances in electrolytes, which are regulated by the kidneys. When kidney function is impaired, it can disrupt electrolyte levels, causing muscle spasms.
- Decreased Mental Sharpness: A decline in mental sharpness and cognitive function can occur when toxins build up in the brain. Impaired kidney function can lead to a buildup of these waste products, affecting mental clarity.
It is important to note that these symptoms may not always indicate CKD, as they can be associated with other health conditions.
Stages of Chronic kidney disease
Chronic kidney disease is divided into five stages based on the level of kidney function, as measured by the glomerular filtration rate (GFR). The GFR is a measure of how much blood the kidneys can filter per minute and is used to determine the severity of kidney damage. The KDIGO (2024) update introduces refinements to the risk stratification grid for CKD progression (Navaneethan et al., 2024). The staging ideally uses both the GFR category and the albuminuria category (CGA framework). The five stages of CKD are as follows:
- Stage 1 (Mild CKD): GFR ≥90 mL/min/1.73 m² with evidence of kidney damage (e.g., albuminuria or structural abnormality). Although filtration appears preserved, damage is present, and signs may be subtle.
- Stage 2 (Mild CKD): The GFR is between 60–89 mL/min/1.73 m², indicating a mild reduction in kidney function. Microalbuminuria may be present, and there may be mild symptoms such as swelling in the hands and feet, itchy skin, or increased urination.
- Stage 3 (Moderate CKD): The GFR is between 30–59 mL/min/1.73 m², indicating a moderate reduction in kidney function. Symptoms become more pronounced at this stage. Stage 3 of chronic kidney disease (CKD) is divided into two sub-stages. Stage 3a, with a glomerular filtration rate (GFR) of 45–59 mL/min/1.73 m², shows a moderate decrease in kidney function with few symptoms. Stage 3b, with a GFR of 30–44 mL/min/1.73 m², indicates a moderate to severe decline in kidney function, accompanied by more noticeable symptoms such as fatigue, swelling, and changes in urination.
- Stage 4 (Severe CKD): The GFR is between 15–29 mL/min/1.73 m², indicating a severe reduction in kidney function. Symptoms become more severe, such as fatigue, shortness of breath, muscle cramps, and changes in appetite. Complications, such as anaemia and bone disease, may also develop.
Stage 5 (End-Stage Renal Disease or ESRD): GFR <15 mL/min/1.73 m² or persistent need for kidney replacement therapy (dialysis or transplant) to sustain life or a decision for conservative non-dialysis care.
It is important to note that CKD can progress through these stages over time, but with proper treatment and management, the progression can be slowed or even halted.
Causes of Chronic kidney disease
Chronic kidney disease is often caused by underlying health conditions that strain the kidneys over time. Common causes of CKD include:
- High Blood Pressure: High blood pressure can damage the small blood vessels in the kidneys. Over time, this damage impairs the kidneys' ability to filter blood effectively, contributing to chronic kidney disease.
- Diabetes: Diabetes leads to high glucose levels in the blood, which can harm the kidney filtering units. Persistent high blood sugar can cause damage to the kidneys' filters, resulting in chronic kidney disease.
- High Cholesterol: High cholesterol levels result in the accumulation of fatty substances in the blood vessels. This buildup can impair kidney function by reducing blood flow and causing damage to the kidney tissues.
- Kidney Infections: Kidney infections cause inflammation and scarring of the kidneys. Repeated or severe infections can damage the kidney tissue and lead to chronic kidney disease.
- Glomerulonephritis: Glomerulonephritis is an inflammation of the kidneys' filtering units, known as glomeruli. This inflammation can damage the kidneys' ability to filter blood properly, leading to chronic kidney disease.
- Polycystic Kidney Disease: Polycystic kidney disease is an inherited condition characterised by the formation of cysts on the kidneys. These cysts can interfere with kidney function and cause chronic kidney disease.
- Blockages in Urine Flow: Blockages in the flow of urine, such as those caused by kidney stones or an enlarged prostate, can increase pressure in the kidneys. This increased pressure can damage the kidney tissues and lead to chronic kidney disease.
- Medications: Long-term use of certain medications, such as lithium and non-steroidal anti-inflammatory drugs (NSAIDs), can strain the kidneys. Prolonged use of these medicines can impair kidney function and contribute to chronic kidney disease.
- Autoimmune Diseases: Autoimmune diseases, such as lupus and IgA nephropathy, can cause the immune system to attack the kidneys. This immune response damages the kidney filters and can lead to chronic kidney disease.
- Inherited Kidney Defects: Inherited kidney defects are congenital anomalies that affect the structure and function of the kidneys. These defects can impair kidney function from birth and increase the risk of chronic kidney disease.
Understanding the causes of CKD can help in identifying risk factors and implementing preventive measures.
Risk Factors
Several factors can increase your likelihood of developing chronic kidney disease. These risk factors include:
Diabetes
High blood pressure
Heart disease and/or heart failure
Obesity
Age over 60 years
Family history of CKD or kidney failure
Personal history of acute kidney injury (AKI)
Smoking and/or tobacco use
Genetic conditions such as ADPKD
Autoimmune diseases like lupus and IgA nephropathy
Who's at Risk?
While anyone can develop chronic kidney disease, certain groups are at a higher risk:
Older adults
Individuals with diabetes
People with high blood pressure
Those with a family history of kidney disease
Individuals with cardiovascular disease
Certain ethnic groups (African Americans, Hispanics, and Native Americans)
If you fall into any of these high-risk categories, it's essential to discuss your kidney health with your doctor and undergo regular screenings for early detection and management of CKD.
Complications
Chronic kidney disease can lead to a range of complications that affect various organs and systems in the body. Some of the most common complications associated with CKD include:
- Cardiovascular Disease: CKD increases the risk of heart disease, heart attacks, and strokes due to the buildup of fluid and waste products in the body.
- Anaemia: As the kidneys become less effective at producing erythropoietin, a hormone that stimulates red blood cell production, patients may develop anaemia, leading to fatigue and weakness.
- Mineral and Bone Disorders: CKD can disrupt the balance of minerals like calcium and phosphorus, leading to weakened bones, fractures, and other skeletal problems.
- High Blood Pressure: Damage to the kidneys can cause hypertension, which further exacerbates kidney damage.
- Fluid Retention: As the kidneys struggle to remove excess fluid, patients may experience swelling in the legs, ankles, and feet, as well as fluid accumulation in the lungs (pulmonary oedema).
- Increased Risk of Infections: CKD weakens the immune system, making patients more susceptible to infections, particularly urinary tract infections.
- Nervous System Problems: Waste buildup can damage nerves, causing numbness, tingling, and weakness in the extremities.
Early intervention based on risk stratification can improve renal and cardiovascular outcomes (McEwan et al., 2024).
Prevention of Chronic kidney disease
Preventing chronic kidney disease involves managing risk factors and adopting a healthy lifestyle. Some key strategies for reducing the risk of developing CKD or slowing its progression include:
Managing Blood Pressure: Keeping blood pressure within a healthy range through medication, diet, and exercise can help protect the kidneys from damage.
Controlling Blood Sugar: For patients with diabetes, maintaining good blood sugar control is crucial to prevent kidney damage caused by high glucose levels.
Maintaining a Healthy Weight: Obesity increases the risk of CKD and other related conditions, so achieving and maintaining a healthy BMI is essential.
Eating a Balanced Diet: A diet low in sodium, processed foods, and added sugars but rich in fruits, vegetables, whole grains, and lean proteins can support kidney health.
Exercising Regularly: Engaging in moderate physical activity for at least 30 minutes a day, five times a week, can help control weight, blood pressure, and blood sugar levels.
Quitting Smoking: Smoking can damage blood vessels and increase the risk of CKD and other cardiovascular diseases.
Limiting Alcohol Consumption: Excessive alcohol intake can harm the kidneys and contribute to CKD development.
Staying Hydrated: Drinking adequate water helps the kidneys flush out toxins and maintain proper function.
By implementing these preventive measures, individuals can significantly reduce their risk of developing chronic kidney disease and its associated complications.
Diagnosis & Tests
Diagnosing chronic kidney disease involves a combination of physical examinations, laboratory tests, and imaging studies. The following tests are commonly used to diagnose CKD:
- Blood Tests: These tests measure the levels of creatinine and urea in the blood, which are waste products that the kidneys normally filter out. High levels of these substances can indicate impaired kidney function.
- Urine Tests: These tests check for the presence of albumin or other proteins in the urine, which can be early signs of kidney damage.
- Glomerular Filtration Rate (GFR): This test estimates how well the kidneys are filtering waste from the blood. GFR is calculated using a formula that considers factors such as age, sex, and blood creatinine levels.
- Imaging Tests: Ultrasound, CT scans, or MRI may be used to visualise the kidneys and detect any structural abnormalities or obstructions.
- Kidney Biopsy: In some cases, a small sample of kidney tissue may be removed and examined under a microscope to determine the cause of kidney damage and help guide treatment decisions.
- According to KDIGO (2024), routine laboratory tests such as serum creatinine, eGFR, and urine albumin remain the mainstay of diagnosis.
- In people with diabetes, hypertension, or other risk factors, regular measurement of eGFR and urinary albumin-creatinine ratio (ACR) is recommended; referral to a nephrologist is advised when eGFR drops to <30 mL/min/1.73 m², albuminuria is ≥300 mg/g, or there is a rapid decline in kidney function.
Early diagnosis of CKD is crucial for effective management and prevention of complications. If you have risk factors for CKD, such as diabetes, high blood pressure, or a family history of kidney disease, it is important to undergo regular screening tests to monitor your kidney function.
Treatment & Management
The management of chronic kidney disease involves a multifaceted approach aimed at slowing the progression of the disease and managing associated complications. The key treatment lines include:
- Blood Pressure Control: Managing hypertension is crucial in slowing CKD progression. Recent guidelines suggest aiming for systolic blood pressure <120 mmHg when tolerated, using standardised office measurement techniques. Medications such as ACE inhibitors and ARBs are commonly used.
- Glycaemic Control: For diabetic patients, controlling blood sugar levels is vital in preventing further kidney damage.
- Dietary Changes: A healthy diet low in salt, fat, and appropriate protein intake can help reduce the strain on the kidneys.
- Physical Activity: Regular exercise helps manage blood pressure, improves overall health, and reduces the risk of cardiovascular disease.
- Smoking Cessation: Quitting smoking slows CKD progression and reduces the risk of cardiovascular disease.
- Anaemia Management: Medications such as erythropoiesis-stimulating agents (ESAs) are used to treat anaemia associated with CKD.
- Multidisciplinary Approach: A team of healthcare professionals, including nephrologists, primary care physicians, dietitians, and social workers, works together to provide comprehensive care.
- Regular Monitoring: Regular monitoring of kidney function, blood pressure, and proteinuria helps track disease progression and adjust treatment accordingly.
Medications for Chronic Kidney Disease (CKD)
Managing chronic kidney disease (CKD) involves a comprehensive medication regimen aimed at slowing disease progression, controlling comorbidities, and addressing complications. Medication selection is tailored based on the patient's CKD stage, underlying cause, associated conditions, and overall health.
1. Blood Pressure Control
Controlling hypertension is crucial for slowing CKD progression and reducing cardiovascular risks.
- ACE Inhibitors:
- Enalapril: It dilates blood vessels and lowers blood pressure, improving symptoms in heart failure.
- Lisinopril: It helps reduce afterload and improve heart function by relaxing blood vessels in hypertension and heart failure.
- Ramipril: It lowers blood pressure and reduces strain on the heart, which is beneficial in managing hypertension and heart failure.
- Perindopril: It helps lower blood pressure and reduce proteinuria, offering kidney protection in chronic kidney disease.
- ARBs (Angiotensin II Receptor Blockers):
- Losartan: Lowers blood pressure and reduces protein loss in urine, helping slow kidney damage progression in CKD.
- Valsartan: Blocks the effects of angiotensin II to reduce blood pressure and protect kidney function in patients with CKD.
- Telmisartan: Offers blood pressure control and renal protection by blocking angiotensin II receptors, often preferred in hypertensive CKD patients.
- Olmesartan: Helps control high blood pressure and reduce kidney strain by blocking angiotensin II, aiding in CKD management.
2. Diuretics
- Loop Diuretics:
- Furosemide: A loop diuretic that reduces fluid overload and swelling, commonly used in CKD patients with oedema or hypertension.
- Torsemide: A long-acting loop diuretic that helps control fluid retention and supports blood pressure control in CKD.
- Bumetanide: A potent loop diuretic that removes excess fluid in patients with advanced CKD and heart failure.
- Thiazide and Thiazide-like Diuretics:
- Hydrochlorothiazide: A thiazide diuretic that helps lower blood pressure and reduce mild fluid retention in the early stages of CKD.
- Chlorthalidone: A long-acting thiazide-like diuretic used to manage hypertension in CKD, especially when combined with loop diuretics.
- Metolazone: Enhances diuresis when combined with loop diuretics, helpful in managing resistant fluid overload in CKD.
3. Lipid Management
CKD patients are at high risk of cardiovascular events; lipid-lowering agents are often indicated.
- Statins:
- Atorvastatin: A statin that lowers LDL cholesterol and reduces cardiovascular risk in CKD patients.
- Rosuvastatin: A potent statin used to manage dyslipidemia and prevent cardiovascular complications in CKD.
- Simvastatin: Lowers cholesterol and helps reduce heart disease risk in patients with moderate to severe CKD.
- Pravastatin: A statin with fewer drug interactions, useful for lipid control in CKD patients with multiple medications.
4. Anaemia Management
- Erythropoiesis-Stimulating Agents (ESAs):
- Epoetin alfa: Stimulates red blood cell production, used to manage anemia commonly seen in chronic kidney disease.
- Darbepoetin alfa: A long-acting ESA that increases hemoglobin levels and reduces the need for frequent dosing in CKD-related anemia.
- Methoxy polyethylene glycol-epoetin beta: A continuous erythropoiesis receptor activator that provides sustained anemia control with less frequent injections in CKD.
- Iron Supplements (oral or IV):
- Ferrous sulfate: An oral iron supplement used to treat iron deficiency anaemia commonly seen in CKD patients.
- Ferric carboxymaltose: An intravenous iron formulation that replenishes iron stores effectively in CKD patients, especially when oral iron is not tolerated.
- Iron sucrose: An IV iron therapy often used in dialysis-dependent CKD patients to correct iron deficiency anemia.
- Ferric gluconate: A parenteral iron supplement that helps improve hemoglobin levels in patients undergoing hemodialysis.
5. Mineral and Bone Disorder (CKD-MBD) Management
- Phosphate Binders:
- Calcium acetate: A phosphate binder that reduces high phosphate levels in CKD patients by preventing phosphate absorption from food.
- Calcium carbonate: Works similarly to calcium acetate in binding dietary phosphate to control hyperphosphatemia in CKD.
- Sevelamer: A non-calcium phosphate binder used to manage elevated phosphate levels without increasing calcium load.
- Lanthanum carbonate: A chewable phosphate binder that helps control serum phosphate levels in advanced CKD.
- Ferric citrate: A dual-action agent that binds phosphate and provides iron, useful in treating hyperphosphatemia and iron deficiency anemia.
- Vitamin D Analogues:
- Calcitriol: The active form of vitamin D used to manage secondary hyperparathyroidism by regulating calcium and phosphate metabolism.
- Alfacalcidol: A vitamin D analog used to support calcium absorption and suppress parathyroid hormone (PTH) in CKD.
- Paricalcitol: A selective vitamin D receptor activator that helps control PTH levels with a lower risk of hypercalcemia.
- Doxercalciferol: Another vitamin D analog that helps reduce elevated PTH in patients with CKD or on dialysis.
- Calcimimetics:
- Cinacalcet: A calcimimetic that lowers PTH, calcium, and phosphate levels in CKD patients with secondary hyperparathyroidism.
- Etelcalcetide: An IV calcimimetic used in dialysis patients to control PTH levels by enhancing the sensitivity of calcium-sensing receptors.
SGLT2 inhibitors (for example, dapagliflozin) and non-steroidal mineralocorticoid receptor antagonists (for example, finerenone) have emerged as effective therapies to slow CKD progression in many patients with or without diabetes KDIGO (2024).
When to See a Doctor?
Recognising the signs and symptoms of chronic kidney disease is crucial for early detection and intervention. If you experience fatigue, swelling, nausea, or difficulty concentrating, it is essential to consult a doctor. Additionally, individuals with risk factors such as diabetes, hypertension, a family history of CKD, or age over 60 should undergo regular kidney function assessments. If your estimated glomerular filtration rate (eGFR) drops below 30 mL/min/1.73 m² or if there are significant changes in kidney function, prompt medical attention is necessary to prevent further damage and manage the condition effectively.
Key Takeaways
Chronic kidney disease is a progressive condition that damages the kidneys and impairs their ability to filter waste from the blood.
Common causes include diabetes, hypertension, glomerulonephritis, polycystic kidney disease, and prolonged obstruction of the urinary tract.
Early stages of CKD often have no symptoms. As the disease progresses, symptoms like fatigue, swelling, poor appetite, and changes in urination may develop.
Diagnosis involves blood and urine tests, imaging studies, and sometimes kidney biopsy. The eGFR and albuminuria levels are used to stage CKD.
Management focuses on treating the underlying cause, slowing progression, and preventing complications through blood pressure control, glycaemic control, dietary changes, smoking cessation, medications, and a multidisciplinary approach.
Early referral to a nephrologist is crucial for specialised care in advanced CKD. Regular monitoring helps adjust treatment and track progression.
Screening for CKD is important in high-risk groups like those with diabetes, hypertension, and a family history of kidney disease. Early detection and intervention improve outcomes.
FAQs
Can I live a normal life with CKD?
With proper management and care, many individuals with CKD can lead fulfilling lives, although lifestyle adjustments may be necessary.
Can chronic kidney disease be treated?
CKD treatment focuses on managing underlying causes and symptoms through lifestyle modifications, medications, and in advanced stages, dialysis or kidney transplantation.
How can I clean my kidneys naturally?
Maintaining a healthy lifestyle, including a balanced diet, staying hydrated, regular exercise, stress management, and avoiding smoking and excessive alcohol, can support kidney health.
Which fruit is best for the kidneys?
Low-sugar, low-phosphorus, and low-potassium fruits like berries (blueberries, raspberries, strawberries) and citrus fruits (oranges, grapefruits) can be incorporated into a kidney-friendly diet.
Can you live 30 years with CKD?
Life expectancy with CKD depends on factors such as age, kidney damage severity, and other health conditions, but advancements in treatment are improving outcomes over time.
References
- Nishimura, M., Yonezawa, K., Sawamura, M., Tanaka, T., Yamamoto, Y., Taki, H., Hatao, M., Takeda, M., Hida, K., Koide, J., Saito, M., Nobuyuki Koriyama, Watanabe, T., Nakajima, R., & Yoshiharu Hoshiyama. (2025). Identification of biomarkers to predict renal function decline and its deceleration in patients with type 2 diabetes and diabetic kidney disease. Journal of Diabetes and Its Complications, 40(1), 109208–109208. https://doi.org/10.1016/j.jdiacomp.2025.109208
- McEwan, P., Gabb, P. D., Davis, J. A., Jose, J., C David Sjöström, Barone, S., Pavlos Kashioulis, Ouwens, M., Syd Cassimaty, Correa-Rotter, R., Rossing, P., Wheeler, D. C., & Hiddo J L Heerspink. (2024). The long-term effects of dapagliflozin in chronic kidney disease: a time-to-event analysis. Nephrology Dialysis Transplantation, 39(12). https://doi.org/10.1093/ndt/gfae106
- Navaneethan, S. D., Bansal, N., Cavanaugh, K. L., Chang, A., Crowley, S., Delgado, C., Estrella, M. M., Cybele Ghossein, T. Alp Ikizler, Koncicki, H., Peter, W. S., Tuttle, K. R., & William, J. (2024). KDOQI US Commentary on the KDIGO 2024 Clinical Practice Guideline for the Evaluation and Management of CKD. American Journal of Kidney Diseases, 85(2). https://doi.org/10.1053/j.ajkd.2024.08.003
- Awdishu, L., Maxson, R., Gratt, C., Rubenzik, T., & Battistella, M. (2025). KDIGO 2024 clinical practice guideline on evaluation and management of chronic kidney disease: A primer on what pharmacists need to know. American Journal of Health-System Pharmacy: AJHP: Official Journal of the American Society of Health-System Pharmacists, zxaf044. https://doi.org/10.1093/ajhp/zxaf044
- KDIGO. (2024). Clinical Practice Guideline for the Evaluation and Management of Chronic Kidney Disease. https://kdigo.org/wp-content/uploads/2024/03/KDIGO-2024-CKD-Guideline.pdf
Check Related Salts
Browse Other Conditions
Latest health articles
Top Health Essentials
Disclaimer
Top-Selling Medicines:
...View more
Top-OTC medicines:
...View more
Company
About UsHealth ArticleHealth StoriesHealth LibraryDiseases & Health ConditionsAyurvedaUnderstanding Generic MedicinesAll MedicinesAll BrandsNeed HelpFAQSecuritySavings CalculatorSubscribe
Registered Office Address
Grievance Officer
Download Truemeds
Contact Us
Our customer representative team is available 7 days a week from 9 am - 9 pm.
v4.23.0
2026 - Truemeds | All rights reserved. Our content is for informational purposes only. See additional information.
Our Payment Partners
















































