Nail Infection (Paronychia)
Paronychia is a common skin infection that occurs around the fingernails or toenails, caused by bacteria or fungi. It can be acute or chronic, with acute paronychia being a sudden and painful infection. In contrast, chronic paronychia is a long-standing infection that can cause persistent inflammation and damage to the nail. Treatment depends on the type and severity of the infection, and prevention involves proper nail care and avoiding irritants.
Last updated on : 08 Apr, 2026
Read time : 12 mins
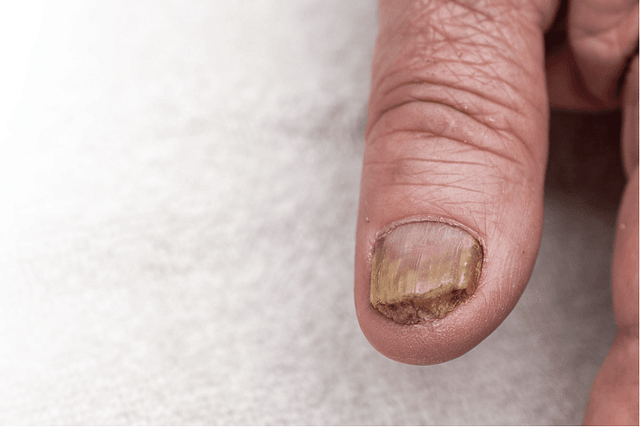
Overview of Disease
Paronychia is a prevalent skin condition that affects the area around the nails. It can cause significant discomfort and, in some cases, lead to more severe complications if left untreated. In this article, we will explore the various aspects of paronychia, including its causes, types, symptoms, and treatment options.
What is Nail Infection (Paronychia)?
Paronychia is an infection of the skin surrounding the fingernails or toenails, usually occurring at the base (cuticle) or along the sides of the nail. This infection is typically caused by bacteria or fungi that gain entry into the skin through a break, injury, or other means, such as biting, chewing, or picking at the nails.
Exposure to harsh chemicals or excessive moisture can also contribute to the development of paronychia. While it can affect people of all ages, certain factors may increase the risk of developing this nail infection. Understanding the different types of paronychia is crucial for accurate diagnosis and effective treatment.
Key Factors about Nail Infection (Paronychia)
| Category | Details |
| Also Referred as | Nail infection, Nail fold infection |
| Commonly Occurs In | Fingers, Toes |
| Affected Organ | Skin around the nail, Nail fold, Nail bed |
| Type | Acute and Chronic |
| Common Signs | Acute: Redness, swelling, pain, pus or abscess. Chronic: Swollen, red, tender nail folds, thickened and discoloured nails |
| Consulting Specialist | Dermatologist, Emergency Medicine Specialist |
| Treatment Procedures | Warm-water soaks, antimicrobial therapy, surgical drainage, topical antifungal, topical steroid, and steroid injection |
| Managed By | Oral Antibiotics (Ampicillin, Doxycycline & Clindamycin), Oral Antifungals (Itraconazole, Fluconazole & Terbinafine), Topical Antibiotics (Mupirocin, Fusidic acid & Retapamulin), Topical Antifungals (Ciclopirox, Amorolfine & Antifungal dusting powder), Topical Antiseptics (Povidone Iodine & Chlorhexidine), Topical steroids, Surgery, Laser therapy |
| Mimicking Condition | Herpetic whitlow, felon, acrokeratosis paraneoplastica |
Types of Nail Infection (Paronychia)
There are two main types of paronychia: (Dulski & Edwards, 2023)
- Acute paronychia: This type of paronychia develops rapidly and is most often caused by a bacterial infection, particularly Staphylococcus aureus. Acute paronychia is characterised by pain, swelling, and redness around the affected nail, and may result in the formation of a pus-filled abscess.
- Chronic paronychia: This type of paronychia is a long-term infection that is usually caused by a fungal infection, particularly Candida albicans. It is often seen in individuals who have repeated exposure to moist environments or irritants, such as housekeepers, dishwashers, and bartenders. Chronic paronychia can cause the nail to become thickened, discoloured, and separated from the skin.
Early Signs of Nail Infection (Paronychia)
The early signs of paronychia include:
- Pain, swelling, and redness around the base or sides of the nail
- Throbbing pain, warmth, and swelling in the skin surrounding a nail
- Presence of pus-filled abscesses or blisters, particularly with bacterial nail infections
- Nail changes such as detachment, abnormal shape, or unusual colouration
- In chronic cases, breakdown of the cuticle and separation of the nail from the skin
If you notice these early signs of paronychia, it is essential to seek prompt treatment to prevent the nail infection from worsening.
Symptoms of Nail Infection (Paronychia)
Paronychia is an infection of the skin surrounding the nails, often characterised by the following symptoms:
- Redness and swelling: The area around the nail becomes red and swollen, indicating inflammation. This may be accompanied by tenderness and warmth to the touch.
- Pain: Affected individuals often experience varying degrees of pain in the area around the nail. The pain can be sharp or throbbing, particularly if the infection is severe.
- Pus formation: In cases of bacterial paronychia, pus may accumulate under the skin or around the nail. This can create a noticeable bump or blister that may need to be drained.
- Nail changes: The nail itself may become discoloured, thickened, or distorted in shape. In chronic cases, the nail may separate from the nail bed.
- Sensitivity: The surrounding skin may feel sensitive or painful when pressure is applied. This can make everyday activities, like typing or gripping objects, uncomfortable.
If you experience these symptoms, it is essential to consult a doctor for an accurate diagnosis and appropriate treatment.
Causes of Nail Infection (Paronychia)
Paronychia is an infectious condition that is most commonly caused by a staphylococcal infection, specifically due to the bacterium Staphylococcus aureus. (DermNet, 2023). However, other bacteria, such as Streptococcus pyogenes, can also be responsible. These bacteria typically enter the skin through:
- Cuts, broken skin, or hangnails
- Ingrown nails, especially common with ingrown toenails
- Skin irritation caused by frequent exposure to water or chemicals
- Trauma to the nailbed or cuticle area, often from accidents, nail biting, or repeated manicures and pedicures
In some cases, paronychia can also be triggered by certain medications. These include retinoids, chemotherapy medicines, HIV treatments, and some antibiotics.
Risk Factors
Several factors can increase the likelihood of developing paronychia, including:
- Frequent exposure to moisture (e.g., dishwashing or wet work)
- Diabetes
- Weakened immune system, such as in individuals with HIV or those taking immunosuppressive medications after an organ transplant
- Occupational exposure to prolonged hand moisture or harsh chemicals, such as in dishwashers, bartenders, and food handlers
- Engaging in improper nail care practices, including biting, picking, or trimming nails too short and damaging the skin around the nails
Identifying and addressing these risk factors can help reduce the likelihood of developing paronychia.
Complications
If left untreated, paronychia can lead to various complications that may cause significant discomfort and potentially serious health issues. Some of the complications associated with paronychia include:
- Abscess formation: In acute paronychia, pus-filled pockets or abscesses can develop, causing increased pain, swelling, and redness. If not drained properly, the infection may spread to deeper tissues.
- Nail damage: Chronic paronychia can lead to permanent nail changes, including thickening, hardening, and deformation. In severe cases, the nail may separate from the nail bed or fall off entirely.
- Spread of infection: If the infection is not managed promptly, it can spread to surrounding tissues, including tendons, bones, or, rarely, the bloodstream, leading to more serious complications.
- Cellulitis: In some cases, the infection may spread to the surrounding skin, causing cellulitis — a potentially severe bacterial skin infection that can lead to swelling, redness, and pain.
Prevention of Nail Infection (Paronychia)
Preventing paronychia involves a combination of good hygiene practices and protective measures. Here are some effective strategies:
- Maintain proper nail care: Keeping nails trimmed and well-groomed can help prevent injuries that lead to infection. Avoid biting or picking at nails and surrounding skin, and use proper tools when trimming nails and cuticles.
- Protect hands from moisture: Limit prolonged exposure to moisture by wearing gloves when doing dishes or cleaning. Keeping hands dry can reduce the risk of fungal infections associated with paronychia.
- Practice good hygiene: Regularly washing hands with soap and water can help prevent bacterial infections. Dry hands thoroughly after washing, as damp skin is more susceptible to irritation and infection.
- Manage underlying health conditions: For individuals with diabetes or weakened immune systems, managing these conditions is crucial. Regular check-ups and proper medication adherence can help minimise the risk of developing paronychia.
- Avoid irritants: Steer clear of harsh chemicals or irritants that can damage the skin around the nails. If working with such substances, use protective gloves to safeguard the skin.
By following these preventive measures, you can significantly reduce your risk of developing paronychia.
Diagnosis & Tests
Diagnosing paronychia typically involves a clinical evaluation and may include specific tests to determine the underlying cause. Here’s how the process generally works:
- Medical history: Your doctor may ask about your medical history, including any recent injuries or exposures that could have led to the development of paronychia.
- Physical examination: Your doctor will carefully examine the affected area, looking for signs of infection such as redness, swelling, warmth, and the presence of pus-filled blisters or abscesses.
- Culture tests: In cases where the infection is severe or does not respond to initial treatment, a sample of pus may be taken and cultured in a laboratory to determine the specific type of bacteria causing the infection. This helps identify the specific bacteria or fungi causing the infection, allowing for targeted treatment.
- Imaging tests: Although not commonly required, imaging tests such as X-rays may be used if there is concern about underlying bone involvement. This can help assess whether the infection has spread deeper into the tissues.
Based on the examination results and any additional tests, your doctor will be able to confirm the diagnosis of paronychia and recommend an appropriate course of treatment.
Treatment & Management
The treatment and management of paronychia depend on the severity of the infection and whether bacteria or fungi are the cause. Here are the common approaches:
- Antibiotic therapy: For bacterial paronychia, oral or topical antibiotics are often prescribed to eliminate the infection. Standard options include dicloxacillin or cephalexin for oral treatment and mupirocin for topical application.
- Antifungal treatment: Antifungal medications may be necessary if a fungal infection causes paronychia. Depending on the severity and type of fungal infection, these can include topical treatments like clotrimazole or oral medications such as fluconazole.
- Drainage of pus: In cases of significant pus accumulation, the doctor may need to drain the infected area. This procedure can relieve pressure and promote more effective healing.
- Proper nail care: Proper nail hygiene is essential for recovery and preventing recurrence. This includes trimming nails, avoiding irritants, and not picking at the nails or surrounding skin.
Regular follow-up with a doctor is essential to monitor the healing process and ensure the infection does not recur. If symptoms persist or worsen, further evaluation may be needed.
Living with Nail Infection (Paronychia)
Living with paronychia requires careful management to prevent complications and recurrence. Here are some key pointers:
- Keep the affected area clean and dry by regularly soaking it in warm water to help with drainage and healing. Ensure the area is thoroughly dried after soaking.
- Avoid irritants such as chemicals, detergents, and other substances that can exacerbate the condition. Wear rubber gloves with an absorbent cotton lining when exposed to such substances.
- Practice proper nail care by avoiding injuring your nails and fingertips. Do not bite or pick your nails, and keep them trimmed and smooth. Avoid cutting nails too short and scraping or trimming your cuticles.
- For chronic paronychia, keep your hands dry and free from chemicals. Change socks regularly and avoid wearing the same shoes consecutively to allow them to dry out completely.
- Use protective gear, such as waterproof gloves that do not irritate the skin, if your job involves frequent exposure to water or harsh chemicals.
- Manage underlying conditions, such as diabetes or weakened immune systems, by maintaining good glycaemic control and following your doctor's recommendations to prevent severe infections.
By following these guidelines, you can effectively manage paronychia and reduce the risk of recurrence. However, it is crucial to know when to seek medical attention for proper treatment.
When to See a Doctor?
If your symptoms are severe, such as significant pain, swelling, redness, or visible pus accumulation near or under the nail, it is important to consult a doctor promptly. Systemic symptoms, such as fever, chills, or red streaks appearing on the skin that run from the infected area towards the body, are warning signs that the infection may be spreading and require immediate medical attention.
Key Takeaways
- Paronychia is an infection of the skin around the nail, often caused by bacteria or fungi.
- Symptoms of paronychia include redness, swelling, pain, and the presence of pus around the affected nail.
- Acute paronychia is often caused by direct or indirect trauma to the cuticle, while chronic paronychia is more commonly seen in individuals whose hands are frequently exposed to moisture or irritants.
- Paronychia treatment depends on the severity and type of infection, ranging from home remedies to antibiotics or surgical intervention in more severe cases.
- To prevent paronychia, practice good hand and nail hygiene, avoid biting or picking at nails, and protect your hands from excessive moisture and irritants.
- If you suspect you have paronychia, monitor your symptoms closely and seek medical attention if they worsen or do not improve with home care.
FAQs
What is the main cause of paronychia?
What is the fastest way to cure paronychia?
Will paronychia go away on its own?
Which antibiotic is best for paronychia?
Does salt water help paronychia?
What deficiency causes paronychia?
Which cream is best for paronychia?
Is Betadine good for paronychia?
What to avoid with paronychia?
Can paronychia be treated at home?
References
- Dulski, A., & Edwards, C. W. (2023). Paronychia. In StatPearls [Internet]. StatPearls Publishing. https://www.ncbi.nlm.nih.gov/books/NBK544307/
- Harvard Health. (2023). Paronychia. https://www.health.harvard.edu/a_to_z/paronychia-a-to-z
- MedlinePlus. (n.d.). Paronychia. https://medlineplus.gov/ency/article/001444.htm
- DermNet. (2023). Paronychia (Nail fold infection): Causes, images, treatment, and more. https://dermnetnz.org/topics/paronychia
Latest health articles
Top Health Essentials
Disclaimer
Top-Selling Medicines:
...View more
Top-OTC medicines:
...View more
Company
About UsHealth ArticleHealth StoriesHealth LibraryDiseases & Health ConditionsAyurvedaUnderstanding Generic MedicinesAll MedicinesAll BrandsNeed HelpFAQSecuritySavings CalculatorSubscribe
Registered Office Address
Grievance Officer
Download Truemeds
Contact Us
Our customer representative team is available 7 days a week from 9 am - 9 pm.
v4.25.1
2026 - Truemeds | All rights reserved. Our content is for informational purposes only. See additional information.
Our Payment Partners
















































