Mycosis (Fungal Infections)
Mycosis (plural: mycoses) refers to a disease caused by fungi and includes a spectrum from superficial infections limited to skin, hair and nails (dermatophyte and yeast infections) to subcutaneous infections following traumatic inoculation, and invasive / systemic fungal diseases that may affect the lungs, bloodstream and deep organs, particularly in immunocompromised people. Aetiology, diagnostic approach, and therapy differ substantially between superficial and invasive forms; therefore, the classification into superficial, subcutaneous and systemic (deep) is clinically important (Reddy et al., 2022)
Last updated on : 21 Apr, 2026
Read time : 15 mins

Overview of Disease
Mycosis is a prevalent condition that affects millions of people worldwide. It is caused by fungi, which are living organisms that obtain their nutrients by decomposing organic matter or by forming symbiotic relationships with other organisms. While many fungi are harmless to humans, some can cause infections, ranging from mild to severe. In this article, we will explore the various aspects of mycosis, including its types, symptoms, diagnosis, treatment, and prevention.
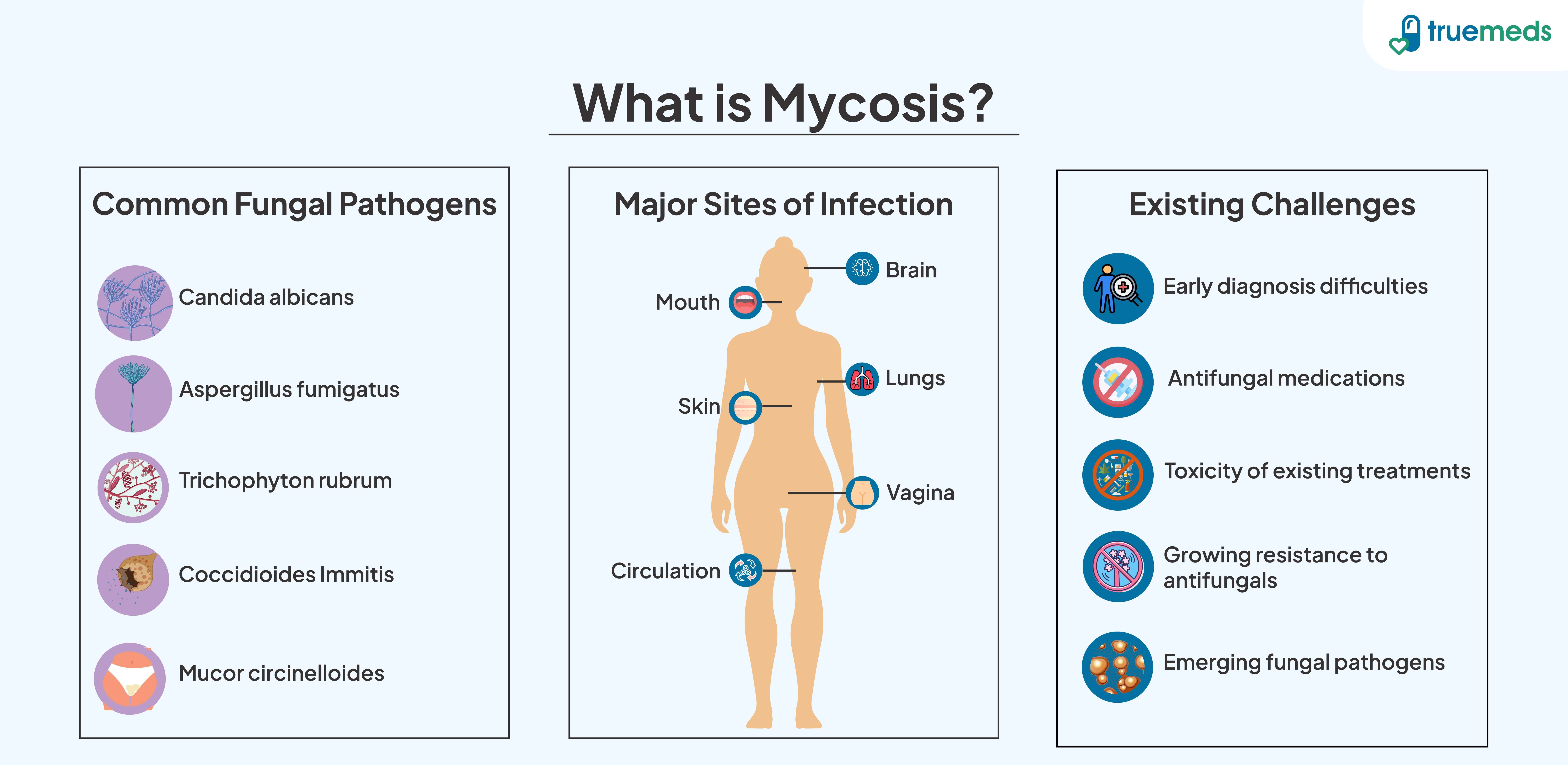
What is Mycosis (Fungal Infections)?
Mycosis is a group of diseases that arise from fungal infections, which may be caused by either yeasts or moulds. While these infections most frequently affect the skin and nails, where they are more visible and easily noticed, fungi are capable of invading much deeper into the body. They can infect internal organs and systems, such as the lungs, mouth, throat, urinary tract, and other areas, especially in individuals with weakened immune defences (Reddy et al., 2022).
Key Factors about Mycosis (Fungal Infections)
| Category | Details |
| Also Referred to as | Fungal infections, mycoses |
| Commonly Occurs In | Superficial mycoses — skin, hair and nails. Subcutaneous mycoses — deeper dermis, subcutaneous tissues and regional lymphatics. Systemic (invasive) mycoses — lungs, bloodstream and visceral organs (liver, spleen, brain, eyes) depending on pathogen and host immunity |
| Affected Organ | Skin, hair, nails, underlying tissues, bone, and organs |
| Type | Superficial, subcutaneous, and deep fungal infections |
| Common Signs | Itchy, ring-like lesions, scaly skin, redness, irritation, painful ulcerations, nodules, lumps |
| Consulting Specialist | Dermatologist, infectious disease specialist |
| Treatment Procedures | Topical antifungal medications, oral antifungal medications, and sometimes surgery |
| Managed By | Clotrimazole, miconazole, terbinafine, or ketoconazole |
| Mimicking Condition | Eczema, psoriasis |
Types of Mycosis (Fungal Infections)
Mycoses are broadly categorised into three main groups based on the depth and extent of the fungal invasion. These include:
1. Superficial fungal infections: These fungal infections are limited to the outermost layers of the skin and its appendages, such as hair and nails. These infections are usually not serious and can be treated with topical antifungal medications. Some common examples of superficial fungal infections include:
- Ringworm (tinea): A dermatophyte infection that can affect various parts of the body, such as the skin (tinea corporis), scalp (tinea capitis), groin (tinea cruris), and feet (tinea pedis).
- Onychomycosis: A fungal infection of the nails, typically caused by dermatophytes, resulting in thickening, discolouration, and separation of the nail from the nail bed.
- Candidiasis: A yeast infection caused by Candida species, which can affect the skin, mucous membranes, and internal organs. Superficial candidiasis includes conditions like oral thrush and vaginal candidiasis.
- Tinea versicolour/pityriasis versicolour: A superficial infection caused by Malassezia, characterised by patches of discoloured skin, often on the trunk and upper arms.
2. Subcutaneous fungal infections: These fungal infections involve the tissues beneath the skin and are often more challenging to treat than superficial infections. These infections typically occur when fungi enter the body through a cut, puncture wound, or other breaks in the skin. Some key examples of subcutaneous fungal infections include:
- Sporotrichosis: Caused by the fungus Sporothrix, this infection usually enters the body through a cut or puncture wound and can cause painful ulcerations and nodules along the lymphatic vessels.
- Chromoblastomycosis: A chronic infection of the skin and subcutaneous tissue, characterised by warty lesions, caused by various fungi, including Fonsecaea and Cladophialophora species.
- Eumycetoma: A chronic, progressive infection that affects the subcutaneous tissue and can extend into deeper structures, including bone. It is caused by various fungi and can lead to severe deformity and disability if left untreated.
3. Deep fungal infections: These fungal infections are serious and potentially life-threatening conditions that can affect internal organs. These infections occur when fungi invade deeper tissues and spread through the bloodstream. Some examples of deep fungal infections include:
- Histoplasmosis: Caused by the fungus Histoplasma, this infection primarily affects the lungs but can spread to other organs, such as the liver, spleen, and central nervous system.
- Coccidioidomycosis: This infection is caused by Coccidioides fungi and can cause flu-like symptoms, pneumonia, and, in severe cases, disseminated disease affecting multiple organs.
- Blastomycosis: Caused by the fungus Blastomyces, this infection can affect the lungs, skin, and other organs, leading to a range of symptoms, from mild respiratory illness to severe systemic disease.
- Aspergillosis: An infection caused by Aspergillus fungi, which can cause various respiratory conditions, from allergic reactions to invasive pulmonary disease, particularly in immunocompromised individuals.
- Invasive candidiasis: A bloodstream infection and deep-organ candidiasis seen in critically ill or immunocompromised patients; it may involve the heart, eyes, liver, spleen, and kidneys.
- Invasive aspergillosis: A primarily pulmonary disease in immunocompromised individuals, with potential angioinvasion and dissemination.
- Pneumocystis jirovecii pneumonia (PCP): Caused by Pneumocystis jirovecii (a fungal organism), it leads to severe pneumonia in people with impaired cellular immunity (e.g., advanced HIV or immunosuppressive therapy) and is managed with specific antibacterial/antipneumocystis agents (trimethoprim-sulfamethoxazole).
- Mucormycosis: A life-threatening angioinvasive infection caused by Mucorales, associated with poorly controlled diabetes, iron overload, and immunosuppression.
- Endemic mycoses (Histoplasma, Coccidioides, Blastomyces, etc.): Infections caused by fungi such as Histoplasma, Coccidioides, and Blastomyces; these are primarily pulmonary infections with potential dissemination in susceptible individuals.
Symptoms of Mycosis (Fungal Infections)
The symptoms of mycosis can vary depending on the type of fungal infection and the area of the body affected. Some common symptoms include:
- Red, itchy patches: These may appear suddenly and can be quite uncomfortable, often indicating an inflammatory response to the fungal infection.
- Scaly or flaky areas: Skin may begin to shed in patches, leading to a rough texture and visible flakes.
- Blisters or pustules: Fluid-filled bumps can develop, which may break open and cause further irritation.
- Discolouration of nails: Infected nails often turn yellow or white, indicating fungal growth beneath the nail. The nail may become unusually thick and prone to breakage, making it difficult to maintain.
- Persistent cough: This can be a sign of lung involvement, often caused by inhaling fungal spores.
- Shortness of breath: Difficulty breathing may occur as the infection affects lung function.
- Chest pain: Discomfort or pain in the chest can indicate inflammation or infection in the lung tissue.
- Fever and chills: Elevated body temperature is a common response to infection, often accompanied by shaking chills.
- Weight loss: Unexplained weight loss may occur due to the body’s increased metabolic demands in fighting the infection.
- Nausea and vomiting: This can occur due to irritation in the digestive tract from the fungal overgrowth. Some individuals may experience vomiting as a result of the body’s attempt to expel irritants.
- Diarrhoea: An increased frequency of loose stools may occur, disrupting normal digestion.
- Abdominal pain: Discomfort or cramping in the abdomen can be a result of gastrointestinal inflammation or irritation.
- Headaches: These can arise from increased pressure or irritation in the central nervous system.
- Confusion: Cognitive changes may occur, impacting clarity of thought and awareness.
- Seizures: In severe cases, fungal infections may provoke seizures due to inflammation in the brain.
Causes of Mycosis (Fungal Infections)
Mycosis, or fungal infections, can be caused by various factors, including:
- Weakened immune system: Conditions that impair the immune system, such as HIV/AIDS, diabetes, cancer, or the use of immunosuppressive medications, can increase the risk of developing mycosis.
- Warm, moist environments: Fungi thrive in warm, humid conditions. Wearing tight, non-breathable clothing or spending prolonged periods in damp areas can create an ideal environment for fungal growth.
- Poor hygiene: Inadequate personal hygiene, such as not washing regularly or failing to dry skin thoroughly, can contribute to the development of fungal infections.
- Contact with infected individuals or animals: Some types of mycosis, such as ringworm (tinea), can be transmitted through direct contact with infected people or animals.
- Prolonged antibiotic use: Antibiotics can disrupt the natural balance of microorganisms on the skin and in the body, allowing fungi to overgrow and cause infections.
- Hormonal changes: Hormonal fluctuations, such as those experienced during pregnancy or menstruation, can alter the body's pH levels and make individuals more susceptible to fungal infections.
- Underlying medical conditions: Certain medical conditions, such as diabetes or peripheral vascular disease, can impair circulation and increase the risk of fungal infections, particularly in the feet.
- Tinea pedis and heel fissures: Fungal infection of the feet (tinea pedis) may cause scaling and maceration that predisposes to fissures, but cracked heels are commonly multifactorial (dry skin, pressure, and footwear). When tinea pedis is suspected, clinical examination and KOH microscopy or culture can confirm dermatophyte infection and targeted topical or systemic antifungal therapy should be used.
Prevention of Mycosis (Fungal Infections)
Preventing mycosis involves a combination of good hygiene practices and lifestyle modifications. Here are some effective strategies to reduce the risk of fungal infections:
- Regularly wash your skin with soap and water, especially after exercising or sweating.
- Dry your skin thoroughly, particularly in areas prone to fungal growth, such as between the toes and under the breasts.
- Fungi thrive in moist environments, so it's essential to keep your skin dry. Use powder in areas where skin rubs against skin, like the groin or under the arms.
- Choose loose-fitting, lightweight clothing made from natural, breathable fabrics like cotton.
- Avoid tight, restrictive clothing that traps moisture against the skin.
- When using public showers, locker rooms, or swimming pools, wear flip-flops or sandals to prevent contact with contaminated surfaces.
- Do not share towels, hairbrushes, or other personal items that can harbour fungi.
- Eat a balanced diet, get regular exercise, and manage stress to support your immune function.
- Avoid walking barefoot in communal wet areas; keep feet dry; change socks frequently; rotate footwear to allow drying; and avoid sharing footwear or towels. Immunocompromised people should promptly report respiratory symptoms and may require prophylaxis (e.g., for PCP in HIV or prolonged high-dose steroid therapy) as advised by specialists.
Diagnosis & Tests
Diagnosis depends on the suspected syndrome. For superficial infections, bedside potassium hydroxide (KOH) microscopy of skin scrapings, hair or nail clippings and fungal culture (or PCR where available) are the primary tests to confirm fungi and identify dermatophytes, Candida or moulds (Reddy et al., 2022). Wood’s lamp can help identify some species (e.g., some Microsporum spp.), but it is not diagnostic for most dermatophytes. Dermoscopy can aid clinical assessment, but does not replace laboratory tests. For invasive disease, blood cultures (for Candida), antigen tests (e.g., galactomannan for Aspergillus, beta-D-glucan as a nonspecific fungal marker), molecular assays and tissue histopathology (with fungal stains) are commonly used. Choose tests according to the clinical presentation and likely pathogens.
Treatment & Management
Principles: Therapy depends on the pathogen (dermatophyte, Candida, Aspergillus, Mucorales, endemic fungi), site (skin/nails vs lung vs bloodstream), host immune status, and severity. Topical agents treat many superficial infections; systemic therapy is required for onychomycosis, extensive dermatophytosis, deep or disseminated infections, and in immunocompromised patients. For invasive infections, early diagnosis and prompt antifungal therapy with or without surgical debridement are critical.
1. Topical Antifungals (Superficial Disease)
Clotrimazole, miconazole, topical terbinafine, tolnaftate, ciclopirox, and topical nystatin (for cutaneous candidiasis) are commonly used. Duration depends on the site; for example, tinea corporis typically needs 1–2 weeks after visible clearing, whereas recalcitrant infections may need longer treatment or systemic therapy.
2. Oral Antifungals (Selected Indications)
- Terbinafine (oral) is first-line for dermatophyte onychomycosis (usual duration 6–12 weeks depending on fingernail/toenail) (Leung & Barankin, 2020).
- Itraconazole and fluconazole are alternatives (choice depends on organism, drug interactions, and hepatic function).
- Griseofulvin may still be used for tinea capitis in some settings, but it is less commonly used for adults; it requires prolonged courses.
- Systemic azoles (voriconazole, posaconazole, isavuconazole) are used for invasive mould infections (aspergillosis, mucormycosis [isavuconazole, posaconazole], etc.) according to guideline-recommended indications.
- Amphotericin B formulations (lipid formulations preferred) are reserved for life-threatening invasive mycoses (severe mucormycosis, severe disseminated disease) and for induction therapy in some settings.
Note: Oral ketoconazole for systemic use is generally avoided because of significant hepatotoxicity and adrenal effects, and is not recommended for systemic therapy in most modern guidelines. - Amorolfine nail lacquer is used topically for onychomycosis in some countries (not universally available everywhere). Topical nail lacquers have modest efficacy as monotherapy for dermatophyte onychomycosis and are often used for mild disease or when systemic therapy is contraindicated; systemic therapy (eg, oral terbinafine) is typically more effective for moderate–severe onychomycosis.
3. Antifungal therapy for Candida and invasive candidiasis
Echinocandins (caspofungin, micafungin, anidulafungin) are first-line empiric therapy for candidemia in critically ill patients; fluconazole is an acceptable option in selected stable, non-neutropenic patients when species and susceptibility permit. Central venous catheters should be removed if feasible in candidemia.
4. Therapy for Pneumocystis Jirovecii (PCP)
TMP-SMX (trimethoprim-sulfamethoxazole) is the treatment and prophylaxis of choice for PCP — note that PCP is caused by a fungal organism but is managed differently from other fungal pneumonias.
5. Adjunctive and surgical management
For subcutaneous mycoses (mycetoma, eumycetoma, chromoblastomycosis, sporotrichosis) and for mucormycosis, surgical debridement and source control are often required in addition to antifungal therapy. Control of underlying conditions (glycaemic control in diabetes, reversal of immunosuppression where possible) is essential.
6. Newer and targeted therapies for invasive fungal disease
Antifungal stewardship and consultation with infectious diseases specialists are advised for complex or refractory infections. Susceptibility testing and therapeutic drug monitoring (for some azoles) are often indicated in deep infections (Cornely et al., 2023).
Important safety notes: Many systemic antifungals (azole class) have significant drug–drug interactions (CYP450 inhibition) and potential hepatotoxicity. Check baseline liver function tests and review concomitant medications before initiating systemic azoles. Terbinafine may interact with certain antidepressants and other medicines; echinocandins generally have fewer drug interactions. Consultation with a pharmacist or an infectious disease specialist is recommended for complex patients.
Living with Disease
If you have been diagnosed with a fungal infection, here are some tips to manage your condition and prevent recurrences:
- Follow the prescribed treatment plan diligently, completing the full course of medications even if symptoms improve.
- Practice good hygiene, especially in affected areas. Keep the skin clean and dry.
- Avoid sharing personal items like towels, hairbrushes, or nail clippers to prevent the spread of infection.
- Wear loose, breathable clothing to minimise moisture retention, which can promote fungal growth.
- Protect your feet by wearing well-fitting, breathable shoes and clean, dry socks. Go barefoot at home when possible.
- Manage underlying health conditions that may increase your risk of fungal infections, such as diabetes or a weakened immune system.
- Avoid walking barefoot in public spaces like locker rooms, showers, or pools to reduce exposure to fungal spores.
When to See a Doctor?
If you suspect you have a fungal infection, it is important to see a doctor promptly. Persistent symptoms such as itching, redness, or rash that worsen despite self-care measures warrant medical attention. If you experience severe symptoms like pain while eating, white patches in the mouth, or discoloured and thick nails, consult your doctor immediately. Early diagnosis and treatment are key to effectively managing mycosis and preventing complications.
Key Takeaways
- Mycosis refers to fungal infections that can affect various parts of the body, including the skin, nails, hair, and internal organs.
- Common types of mycosis include dermatophytosis, candidiasis, aspergillosis, and other fungal infections.
- Symptoms of mycosis vary depending on the type and location of the infection, but may include skin rashes, itching, nail changes, and respiratory issues.
- Treatment for mycosis depends on the type and severity of the infection and may include topical or oral antifungal medications, as well as more complex therapies for deep or severe infections.
- Living with mycosis requires good hygiene, environmental protection, symptom monitoring, and adherence to prescribed treatment regimens.
- Seeking prompt medical attention for suspected fungal infections is essential, particularly for individuals with weakened immune systems or persistent symptoms.
FAQs
What causes mycosis?
How is mycosis transmitted?
Can mycosis be cured?
What is mycosis of the lungs?
How does mycosis start?
How do you treat skin mycosis?
How is mycosis detected or diagnosed?
How to remove fungal infection?
Which vitamin deficiency causes fungal infection?
How long does mycosis last?
Who kills fungus?
References
- Reddy, G. K. K., Mondal, S., & Chakrabarti, A. (2022). Fungal infections: Pathogenesis, antifungals, and alternative therapeutics. Journal of Fungi, 8(4), 354. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9325902/
- Leung, A. K. C., & Barankin, B. (2020). Onychomycosis: An updated review. Journal of Fungi, 6(4), 125. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7509699/
- Keshwania, P., et al. (2023). Superficial dermatophytosis across the world's populations: A review. ACS Omega, 2023. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC10483660/
- Cornely, O. A., et al. (2019). Global guideline for the diagnosis and management of mucormycosis (ECMM/MSG), with updates (2021–2023). Lancet Infectious Diseases. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8559573/
Check Related Salts
Browse Other Conditions
Latest health articles
Top Health Essentials
Disclaimer
Top-Selling Medicines:
...View more
Top-OTC medicines:
...View more
Company
About UsHealth ArticleHealth StoriesHealth LibraryDiseases & Health ConditionsAyurvedaUnderstanding Generic MedicinesAll MedicinesAll BrandsNeed HelpFAQSecuritySavings CalculatorSubscribe
Registered Office Address
Grievance Officer
Download Truemeds
Contact Us
Our customer representative team is available 7 days a week from 9 am - 9 pm.
v4.23.0
2026 - Truemeds | All rights reserved. Our content is for informational purposes only. See additional information.
Our Payment Partners
















































