Yeast Infection
Yeast infections, caused by an overgrowth of the Candida fungus, are common and can affect various body parts. Symptoms vary depending on the type of infection, but often include itching, burning, redness, and discharge. Treatment options are available, and prevention strategies can help reduce the risk of developing yeast infections.
Last updated on : 08 Apr, 2026
Read time : 13 mins
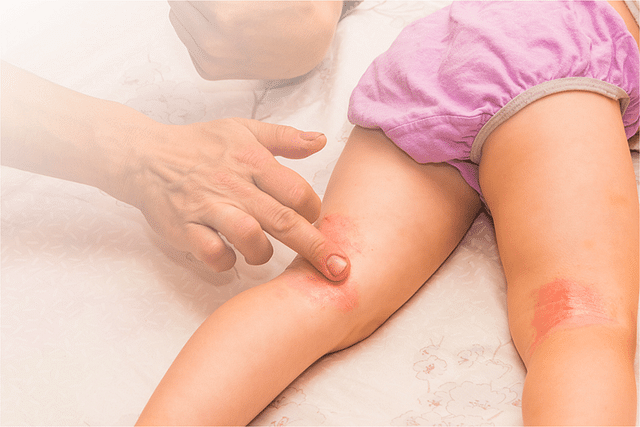
Overview of Disease
Yeast infections, medically known as candidiasis, are fungal infections caused by an overgrowth of the yeast Candida. This type of yeast naturally lives in small amounts in various parts of the body, including the mouth, throat, gut, and vagina. However, when the balance of healthy bacteria and yeast is disrupted, Candida can grow out of control, leading to an infection. Understanding the causes, symptoms, and treatment options for yeast infections is crucial for maintaining overall health and well-being.
What Is Yeast Infection?
A yeast infection occurs when the delicate balance between beneficial bacteria and Candida in the body is disrupted, allowing the fungus to multiply excessively. Various factors, such as changes in the physical environment, hormonal imbalances, or certain medications, can trigger this imbalance.
While yeast infections are more prevalent in women, they can also affect men. To better understand yeast infections, it is essential to know the different types and their specific characteristics.
Key Factors about Yeast Infection
| Category | Details |
| Also Referred as | Candidiasis, Vulvovaginal Candidiasis, Thrush |
| Commonly Occurs In | Women of childbearing age, infants, people with weakened immune systems, and those taking antibiotics |
| Affected Organ | Vagina, penis, mouth, throat, tongue, skin folds, nails |
| Type | Fungal infection caused by Candida species, typically Candida albicans |
| Common Signs | Itching, burning, redness, white discharge (like curdled milk or cottage cheese), painful sex, and urination discomfort |
| Consulting Specialist | Gynaecologist, Dermatologist, Primary Care Physician |
| Treatment Procedures | Antifungal medications (creams, suppositories, oral pills), medicated mouthwash or lozenges for thrush |
| Managed By | Antifungal medications |
| Mimicking Condition | Bacterial vaginosis (BV), sexually transmitted infections (STIs) |
Types of Yeast Infection
There are different types of yeast infections, each affecting various parts of the body:
- Vaginal Candidiasis: Also known as vaginal yeast infection, this is the most common type of yeast infection. It occurs when Candida yeast cells grow out of control in the vagina.
- Symptoms include itching, burning, redness, and swelling of the vulva, along with a thick, white, odour-free vaginal discharge.
- Oral Candidiasis (Thrush): It is an infection of the mouth and throat, according to the World Health Organization (2025). It is most common in newborns and adults with weakened immune systems.
- Symptoms include white patches that feel lumpy, pain, and difficulty swallowing.
- Cutaneous Candidiasis: This type of yeast infection occurs when Candida yeast cells grow out of control on the skin. It affects moist areas of the skin, such as the armpits, underarms, and the groin or diaper area.
- Symptoms include itchy red skin, rashes, and blisters.
- Invasive Candidiasis: This is a serious and life-threatening type of yeast infection that occurs when Candida yeast cells enter the bloodstream. They then spread to other parts of the body, such as the heart, brain, and bones.
- It is more common in individuals with weakened immune systems or recent hospital stays and carries a higher risk.
- Nail Candidiasis: This infection affects the nails, causing colour changes, thickening, and brittleness.
- It is common in people who often expose their hands to water or wear synthetic gloves.
- Penile Candidiasis: A yeast infection affecting men, particularly those who are uncircumcised or have a weakened immune system.
- Symptoms include redness, itching, and a white, lumpy discharge.
Symptoms of Yeast Infection
The symptoms of a yeast infection can vary depending on the area affected.
- The most common signs include intense itching, irritation, and burning sensations.
- In the case of vaginal candidiasis, women may experience redness and swelling of the vulva and vagina, accompanied by pain and soreness.
- A thick, white, odourless vaginal discharge resembling cottage cheese is another telltale symptom.
- Some women may also notice a watery discharge, a vaginal rash, or minor cuts and cracks in the skin of the vulva.
- Penile yeast infections often cause itching and burning at the head of the penis, along with redness. A thick white substance may collect in the skin folds, and shiny patches on the penis may also appear.
Causes of Yeast Infection
Yeast infections are caused by an overgrowth of the fungus Candida, usually Candida albicans. This overgrowth occurs when the natural balance of bacteria and yeast is disrupted. Several factors can disrupt the delicate balance of yeast and bacteria in the vagina, leading to an infection.
Antibiotics: Antibiotics kill healthy vaginal bacteria, allowing yeast to overgrow and cause infections.
Hormonal Changes: Pregnancy, menstruation, and hormonal contraceptives can disrupt the balance, leading to yeast infections.
Uncontrolled Diabetes: High blood sugar levels promote yeast growth, increasing the risk of infection.
Weakened Immune System: Conditions like HIV/AIDS or corticosteroid use weaken immunity, making yeast infections more likely.
Physical Irritants: Tight clothing, synthetic materials, and certain vaginal products create conditions that promote yeast growth.
Risk Factors
Several factors can increase the risk of developing a yeast infection.
- Antibiotic Use: Broad-spectrum antibiotics kill a wide range of bacteria, disrupting the natural vaginal flora and increasing yeast overgrowth.
- Increased Estrogen Levels: High estrogen levels, during pregnancy or with birth control and hormone therapy, can promote yeast growth.
- Uncontrolled Diabetes: Elevated blood sugar levels in uncontrolled diabetes encourage yeast overgrowth in the vaginal area.
- Weakened Immune System: A weakened immune system from illness or medications makes the body more vulnerable to yeast infections.
- Lifestyle Habits: Wearing tight-fitting clothing and using scented feminine products can create an environment that supports yeast growth.
Being aware of these risk factors can help individuals take preventive measures and seek prompt treatment if a yeast infection occurs.
Who's at Risk?
Several groups of people are more prone to yeast infections:
- Women: Yeast infections are much more common in women than in men due to the unique anatomy and hormonal fluctuations experienced by females.
- Individuals with Diabetes: Uncontrolled diabetes can lead to higher sugar levels in the body, providing an ideal environment for yeast to thrive. It can lead to oral candidiasis in around 25% of patients with uncontrolled diabetes. (Mohammed et al., 2021)
- People with Compromised Immune Systems: Those with weakened immune systems, such as individuals with HIV/AIDS or those undergoing chemotherapy, are more susceptible to yeast overgrowth.
- Pregnant Women: Hormonal changes during pregnancy can alter the vaginal environment, increasing the likelihood of yeast infections.
By identifying and addressing these risk factors, individuals can take proactive steps to prevent yeast infections and maintain their overall well-being.
Complications
If left untreated or not appropriately managed, yeast infections can lead to several complications.
- Vaginal Complications: Severe itching, redness, and inflammation can lead to skin infections if the area becomes cracked or scratched.
- Bacterial Infections: Scratching the affected area may introduce bacteria, increasing the risk of bacterial infections.
- Urethral Discomfort: The infection can spread towards the urethra, causing additional discomfort and irritation.
- Pregnancy Risks: Severe or untreated infections may be associated with complications such as discomfort or neonatal oral thrush, rather than directly causing miscarriage or premature labour.
- Oral Thrush Complications: Untreated oral thrush can spread to other organs in those with weak immune systems, leading to serious health issues.
- Invasive Candidiasis: Rarely, Candida can enter the bloodstream, leading to invasive candidiasis that affects major organs and requires urgent treatment.
Frequent yeast infections may signal an underlying condition, such as a weakened immune system or diabetes.
Prevention of Yeast Infection
Preventing yeast infections involves several strategies, including maintaining good hygiene, wearing appropriate clothing, managing underlying health conditions, and making lifestyle changes.
- Good Genital Hygiene: Maintain hygiene, but avoid harsh soaps or douching to prevent disrupting the natural balance of bacteria and fungi.
- Wear Breathable Clothing: Choose breathable fabrics and avoid tight, synthetic garments to reduce moisture that can encourage fungal growth.
- Control Blood Sugar Levels: For individuals with diabetes, managing blood sugar levels can help prevent yeast infections.
- Avoid Unnecessary Medications: Limit the use of antibiotics, steroids, and other medications that can weaken the immune system or disrupt natural flora.
- Manage Stress and Use Breathable Pads: Reducing stress and avoiding non-breathable panty liners or pads can help lower the risk of yeast infections.
Early detection and treatment of yeast infections are essential for preventing complications and ensuring a speedy recovery.
Diagnosis & Tests
Diagnosing a yeast infection typically involves a combination of physical examination and laboratory tests. During a physical exam, a healthcare provider will assess the affected area for signs of inflammation, redness, and discharge. They may ask about your symptoms and any potential risk factors for developing a yeast infection. This including recent antibiotic use or a weakened immune system.
Laboratory tests may be performed to confirm the presence of Candida and rule out other potential causes of the symptoms. These tests may include:
- Microscopy: A sample of the affected area is examined under a microscope to detect yeast cells.
- Culture: A sample is collected from the affected area and grown in a laboratory to identify the specific Candida species causing the infection.
- Blood Tests: In cases of suspected systemic candidiasis, blood tests may be performed to detect Candida in the bloodstream.
Accurately diagnosing a yeast infection is crucial in determining the most appropriate course of treatment and preventing potential complications.
Treatment & Management
The yeast infection treatment is focused on eliminating the fungal overgrowth, relieving associated symptoms, preventing recurrence, and restoring a healthy microbial balance. Early identification and consistent treatment are vital for achieving effective and sustained resolution. Below are the recommended therapeutic approaches for yeast infections:
1. Topical Azole Antifungals
Topical azoles are the first-line therapy for mild-to-moderate and uncomplicated vaginal yeast infections.
- Clotrimazole: Works by disrupting ergosterol synthesis, a key component of the fungal cell membrane, leading to cell death.
- Miconazole: Offers broad-spectrum antifungal coverage and provides quick symptom relief from itching and irritation.
Topical azoles help to:
- Alleviate localised itching, burning, and discharge
- Act directly at the site of infection
- Minimise systemic side effects
- Offer both OTC and prescription formulations for flexible use
2. Oral Azole Therapy
For recurrent or more severe yeast infections, systemic antifungal therapy is recommended.
- Fluconazole: A single oral dose is typically effective for uncomplicated cases. Longer or repeated dosing regimens are considered for recurrent infections.
Oral azoles help to:
- Provide convenient single-dose or short-course treatment
- Reach systemic or deep-seated fungal sites
- Reduce the risk of relapse in chronic sufferers
- Support maintenance therapy in recurrent vulvovaginal candidiasis
3. Prescription Intravaginal Therapy
For infections caused by azole-resistant Candida species or non-albicans strains, prescription-strength options are often required.
- Terconazole: A prescription-only intravaginal cream or suppository that effectively treats azole-resistant strains and persistent infections.
Intravaginal therapies help to:
- Target hard-to-treat Candida strains
- Offer stronger antifungal action than OTC options
- Improve response in patients with recurrent infections
- Provide alternative formulations for those intolerant to oral medication
4. Alternative Therapies
Used when standard treatments fail or for managing resistant cases.
- Boric Acid Suppositories: Particularly useful for treating infections caused by Candida glabrata. Due to its antifungal and antiseptic properties, it is a suitable second-line option, though it must be used under strict medical guidance.
Alternative therapies help to:
- Address treatment-resistant strains
Provide relief when conventional antifungals are ineffective - Reduce recurrence in chronic infections
- Offer cost-effective and local treatment
5. Polyenes for Mucocutaneous Candidiasis
Polyenes, such as nystatin, are widely used to treat oral and superficial fungal infections.
- Nystatin: Functions by binding to ergosterol in the fungal membrane, causing leakage of intracellular contents and fungal death.
Polyenes:
- Effectively treat oral thrush and cutaneous candidiasis
- Offer a non-azole alternative with minimal systemic absorption
- Prevent fungal colonisation in immunocompromised individuals
- Serve as prophylaxis in at-risk patients
- Enhance treatment in combination with other antifungals
When to See a Doctor?
While mild yeast infections can often be managed with over-the-counter treatments, there are certain situations where it is crucial to seek medical advice. If you experience symptoms of a yeast infection for the first time, consult a healthcare provider. This ensures you receive an accurate diagnosis. It's important to rule out other conditions with similar symptoms, such as bacterial vaginosis or a sexually transmitted infection (STI).
Seek prompt medical attention for severe symptoms like extensive redness, swelling, sores, fever, chills, or pelvic pain. These symptoms may indicate a more serious infection that requires specialised treatment.
According to the Office on Women’s Health (2025), you must consult a doctor if you have recurrent yeast infections — defined as four or more in a year. The doctor can identify underlying causes and develop a long-term treatment plan to prevent future infections.
Pregnant women and those with weakened immune systems, such as HIV/AIDS or chemotherapy patients, should consult a healthcare provider. They may be at higher risk for complications or need specialised treatment. Seeking timely medical advice ensures proper care and reduces the risk of complications or recurrent infections.
Key Takeaways
- Yeast infections are common fungal infections caused by an overgrowth of Candida yeast.
- Common symptoms include itching, burning, redness, and vaginal discharge.
- Risk factors include antibiotic use, diabetes, a weakened immune system, and hormonal changes.
- Diagnosis involves physical examination and laboratory tests.
- Antifungal medications, both over-the-counter and prescription, are the primary treatment.
- Some lifestyle measures, such as probiotics and hygiene practices, may support symptom management but do not replace antifungal treatment.
- Consult a doctor for first-time infections, uncertain diagnosis, or severe/persistent symptoms.
FAQs
What daily habits can lead to the development of a yeast infection?
How can I tell if I have a yeast infection?
Can yeast infections resolve without treatment?
What's the quickest way to cure a yeast infection?
How can I differentiate between a yeast infection and an STD?
Can a yeast infection cause serious health issues?
What steps should a female take if she has a yeast infection?
Are there any effective home remedies for treating yeast infections?
Is there an odour associated with yeast infections?
How much time does it take for a yeast infection to clear up?
References
- Centres for Disease Control and Prevention. (2022). Vaginal candidiasis. https://www.cdc.gov/fungal/diseases/candidiasis/genital/index.html
- Johns Hopkins Medicine. (n.d.). Yeast infection. https://www.hopkinsmedicine.org/health/conditions-and-diseases/candidiasis-yeast-infection
- National Health Service. (2021). Thrush in men and women. https://www.nhs.uk/conditions/thrush-in-men-and-women/
- The American College of Obstetricians and Gynecologists. (2020). Vaginitis. https://www.acog.org/womens-health/faqs/vaginitis
- MedlinePlus. (2021). Candidiasis. https://medlineplus.gov/candidiasis.html
- Office on Women's Health. (2021). Vaginal yeast infections. U.S. Department of Health and Human Services. https://www.womenshealth.gov/a-z-topics/vaginal-yeast-infections
- Pappas, P. G., Kauffman, C. A., Andes, D. R., Clancy, C. J., Marr, K. A., Ostrosky-Zeichner, L., Reboli, A. C., Schuster, M. G., Vazquez, J. A., Walsh, T. J., Zaoutis, T. E., & Sobel, J. D. (2016). Clinical practice guideline for the management of candidiasis: 2016 update by the Infectious Diseases Society of America. Clinical Infectious Diseases, 62(4), e1-e50. https://doi.org/10.1093/cid/civ933
- World Health Organization: WHO. (2025). Candidiasis (yeast infection). https://www.who.int/news-room/fact-sheets/detail/candidiasis-(yeast-infection)
- Mohammed, L., Jha, G., Malasevskaia, I., Goud, H. K., & Hassan, A. (2021). The interplay between sugar and yeast infections: Do diabetics have a greater predisposition to develop oral & vulvovaginal candidiasis Cureus.https://doi.org/10.7759/cureus.13407
Check Related Salts
Browse Other Conditions
Latest health articles
Top Health Essentials
Disclaimer
Top-Selling Medicines:
...View more
Top-OTC medicines:
...View more
Company
About UsHealth ArticleHealth StoriesHealth LibraryDiseases & Health ConditionsAyurvedaUnderstanding Generic MedicinesAll MedicinesAll BrandsNeed HelpFAQSecuritySavings CalculatorSubscribe
Registered Office Address
Grievance Officer
Download Truemeds
Contact Us
Our customer representative team is available 7 days a week from 9 am - 9 pm.
v4.25.3
2026 - Truemeds | All rights reserved. Our content is for informational purposes only. See additional information.
Our Payment Partners










































