Liver Cirrhosis
Liver cirrhosis is a serious condition characterised by the gradual scarring of the liver, leading to impaired liver function and potential liver failure. It is often the result of persistent liver damage over many years, commonly caused by alcohol, chronic viral hepatitis, metabolic disorders, and certain medicines. Liver cirrhosis progresses through several stages, each with distinct characteristics and symptoms.
Last updated on : 23 Apr, 2026
Read time : 15 mins

Overview of Disease
Liver cirrhosis is a serious condition that develops when the liver suffers long-term damage, often due to infection, other diseases, or chronic alcohol use. As the liver attempts to repair itself, scar tissue forms, gradually replacing healthy liver cells. This scarring process compromises the liver's ability to filter toxins, produce enzymes, synthesise proteins, store nutrients, and fight infections. Early detection and treatment of liver cirrhosis are crucial for preventing further damage and improving patient outcomes.
What is Liver Cirrhosis?
Liver cirrhosis is a progressive disease that occurs when scar tissue accumulates in the liver over an extended period. This scarring, known as fibrosis, is the liver's response to chronic injury or inflammation. As more scar tissue forms, the liver's structure and function become increasingly impaired. Cirrhosis can result from various causes, including viral hepatitis, excessive alcohol consumption, non-alcoholic fatty liver disease, and autoimmune disorders. Recognising the early signs and risk factors for liver cirrhosis is essential for timely diagnosis and treatment.
Key Factors about Liver Cirrhosis
| Category | Details |
| Also Referred to as | Scarring of the liver, hepatic fibrosis, hepatic cirrhosis, end-stage liver disease |
| Commonly Occurs In | People with a history of heavy alcohol use, overweight or obesity, type 2 diabetes, men, and those aged 40 or older |
| Affected Organ | Liver |
| Type | Compensated and Decompensated cirrhosis |
| Common Signs | Fatigue, weakness, weight loss, nausea, bruising or bleeding easily, swelling in legs, feet, or ankles, jaundice, ascites, hepatic encephalopathy |
| Consulting Specialist | Gastroenterologist, Hepatologist |
| Treatment Procedures | Lifestyle changes, medications, and liver transplantation |
| Managed By | Alcohol dependence (disulfiram, acamprosate), Viral hepatitis (lamivudine, entecavir, and tenofovir disoproxil fumarate), Wilson’s disease (D-penicillamine and trientine), Portal hypertension (propranolol), Hepatic encephalopathy (e.g., lactulose, rifaximin) |
| Mimicking Condition | Hepatic Fibrosis, Chronic Viral Hepatitis |
Types of Liver Cirrhosis
Liver cirrhosis can be classified based on the size and distribution of the scar tissue nodules in the liver. These include:
- Micronodular cirrhosis: Micronodular cirrhosis is characterised by the presence of small, uniformly distributed regenerative nodules (less than 3 mm) throughout the liver. This type of cirrhosis is often associated with chronic alcohol-related liver disease, where long-term alcohol use leads to widespread liver damage and scarring.
- Macronodular cirrhosis: Macronodular cirrhosis features larger regenerative nodules (greater than 3 mm) that are irregularly distributed throughout the liver. This type of cirrhosis is commonly associated with viral hepatitis and non-alcoholic fatty liver disease.
- Mixed cirrhosis: Mixed cirrhosis features both micronodular and macronodular characteristics, with varying sizes of regenerative nodules in the liver. It may arise from the progression of one type to another or the simultaneous presence of multiple causes of liver damage, such as chronic alcohol use and viral hepatitis.
Early Signs of Disease
The early signs of liver cirrhosis include:
- Persistent fatigue or weakness
- Skin itching
- Appetite loss and unintended weight loss
- Nausea and vomiting
- Mild pain or discomfort in the upper right abdominal area over the liver
- Muscle loss and weakness
- Swelling in the lower extremities (oedema)
- Spider angiomas (spider-like small blood capillaries) on the skin above the waist
- Palmar erythema (blotchy redness on the palms)
Recognising these early signs of liver cirrhosis is crucial for timely diagnosis and effective treatment.
Symptoms of Liver Cirrhosis
The symptoms of liver cirrhosis can vary based on the stage of the disease and may include:
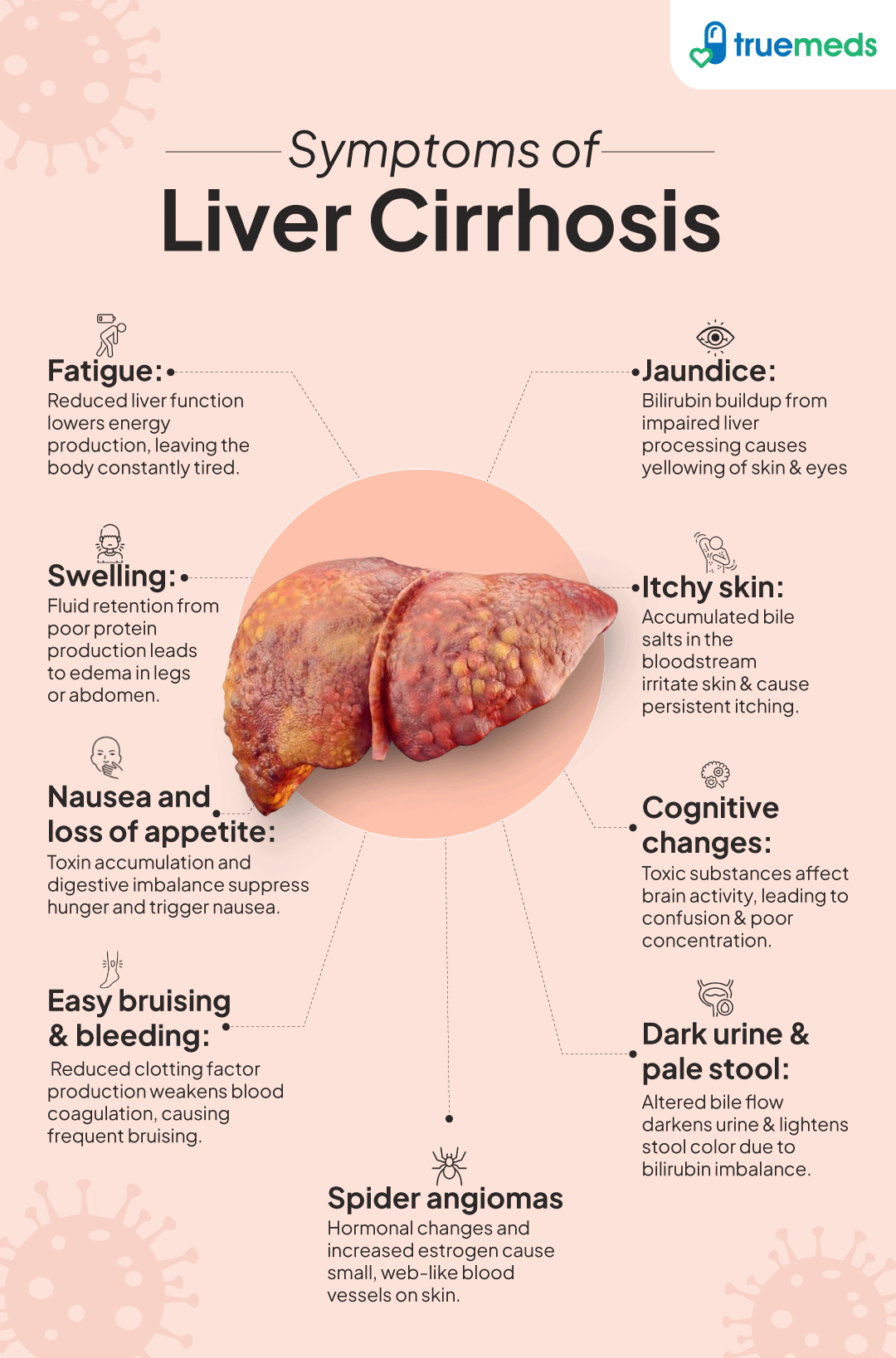
- Fatigue: Persistent tiredness and weakness are common early symptoms of liver cirrhosis, often resulting from the liver's impaired ability to function properly.
- Jaundice: This condition causes yellowing of the skin and eyes due to the buildup of bilirubin in the blood, a byproduct of red blood cell breakdown that the damaged liver cannot process efficiently.
- Swelling: Fluid retention, known as oedema, can occur in the legs, ankles, and abdomen (ascites) due to increased pressure in the blood vessels of the liver and changes in hormone levels.
- Itchy skin: Chronic itchiness may arise from the accumulation of bile salts in the skin, a result of the liver's impaired ability to excrete bile.
- Nausea and loss of appetite: Individuals may experience nausea, vomiting, and a reduced desire to eat, leading to weight loss and nutritional deficiencies.
- Easy bruising and bleeding: Cirrhosis can impair the liver's ability to produce clotting factors, resulting in easy bruising, prolonged bleeding from cuts, or the occurrence of nosebleeds.
- Spider angiomas: These small, spider-like blood vessels may appear on the skin, particularly on the face and upper body, as a result of hormonal changes and increased blood flow.
- Cognitive changes: Confusion, difficulty concentrating, and altered mental status can occur due to a buildup of toxins in the bloodstream, leading to a condition known as hepatic encephalopathy.
- Dark urine and pale stool: Changes in urine and stool colour can indicate liver dysfunction. Dark urine results from excess bilirubin, while pale or clay-coloured stools may indicate a lack of bile.
Stages of Liver Cirrhosis
Cirrhosis is classified based on clinical severity and complications. The stages of cirrhosis include:
Compensated Cirrhosis
Compensated cirrhosis is the stage where the liver still functions adequately despite scarring, and patients may not experience noticeable symptoms. At this stage, there are no major complications such as ascites, variceal bleeding, or hepatic encephalopathy. This stage can last for many years without apparent signs.
Decompensated Cirrhosis
Decompensated cirrhosis is the advanced stage of the disease, characterised by extensive scarring and the development of complications such as ascites, varices, and hepatic encephalopathy (European Association for the Study of the Liver, 2025). Symptoms at this stage may include fluid buildup in the abdomen (ascites) and legs (oedema), enlarged veins in the digestive tract (varices), confusion due to toxin buildup in the brain (hepatic encephalopathy), and an increased risk of liver cancer and infections such as spontaneous bacterial peritonitis.
End-Stage Liver Disease (ESLD)
End-stage liver disease (ESLD) is the most severe stage of cirrhosis, where the liver is unable to maintain essential metabolic, synthetic, and detoxification functions. Patients may require a liver transplant to survive. Symptoms at this stage can include severe jaundice, itching, easy bruising, and fluid buildup in the abdomen and legs.
Causes of Liver Cirrhosis
Liver cirrhosis can result from a variety of factors that cause long-term damage to the liver. Some of the causes include:
- Alcohol-associated liver disease: This results from excessive alcohol consumption over an extended period. The liver is responsible for processing alcohol, and chronic exposure to high levels of alcohol can lead to inflammation, scarring, and ultimately, cirrhosis.
- Non-alcoholic fatty liver disease (NAFLD): This condition is often associated with obesity, metabolic syndrome, or type 2 diabetes. If left untreated, NAFLD can progress to non-alcoholic steatohepatitis (NASH) and eventually cirrhosis.
- Chronic hepatitis B and C infections: Long-term infections with hepatitis B or C viruses can also cause liver cirrhosis. These viral infections damage liver cells over time, leading to inflammation and scarring.
- Autoimmune hepatitis: In some cases, the body's immune system may mistakenly attack the liver, causing a condition known as autoimmune hepatitis. This chronic inflammation can lead to liver damage and cirrhosis if not properly managed.
- Inherited liver diseases: Certain inherited liver diseases, such as Wilson disease, haemochromatosis, and alpha-1 antitrypsin deficiency, can also contribute to the development of liver cirrhosis. These conditions involve the accumulation of toxic substances or abnormal proteins in the liver, causing damage over time.
- Blockage of the bile ducts: Diseases that cause blockage of the bile ducts, such as primary biliary cholangitis and primary sclerosing cholangitis, can lead to liver cirrhosis. These conditions prevent the normal flow of bile, leading to inflammation and scarring of the liver.
- Long-term use of certain medications: In rare cases, long-term use of certain medications, such as methotrexate or amiodarone, can cause liver damage and cirrhosis. It is essential for individuals taking these medications to be closely monitored by their doctor.
Risk Factors
Certain risk factors can increase an individual's likelihood of developing liver cirrhosis, including:
- Excessive alcohol consumption
- Obesity
- Type 2 diabetes
- High blood pressure
- High cholesterol
- Exposure to toxins, such as industrial chemicals or pesticides
- Family history of liver disease
- Shared needles
- Unprotected sexual contact with an infected person
- Blood transfusions before 1992 (when screening for hepatitis C began)
Who's at Risk?
Certain populations are more vulnerable to liver cirrhosis, including:
- Individuals with a history of excessive alcohol use
- People with obesity, type 2 diabetes, or metabolic syndrome
- Those with chronic viral hepatitis (hepatitis B or C)
- Individuals with autoimmune disorders affecting the liver
- People with inherited liver diseases, such as haemochromatosis or Wilson disease
- Individuals exposed to certain toxins or medications that can damage the liver
- People with a family history of liver disease
Complications
Liver cirrhosis is a severe condition that can lead to a range of complications affecting various body systems. Some of the most common complications include:
- Hepatic encephalopathy: Hepatic encephalopathy occurs when the liver is unable to remove toxins from the blood, causing them to accumulate in the brain. This can lead to mental confusion, difficulty concentrating, and, in severe cases, unresponsiveness or coma.
- Ascites: Ascites is the buildup of fluid in the abdomen caused by increased pressure in the portal vein (portal hypertension) and the liver's reduced ability to produce blood proteins like albumin. This can cause swelling in the abdomen and lower body.
- Variceal bleeding: Variceal bleeding is a life-threatening complication that occurs when veins in the oesophagus or stomach rupture due to increased pressure from portal hypertension.
- Hepatorenal syndrome: Hepatorenal syndrome is a type of functional kidney failure that can occur in patients with advanced liver disease. It is characterised by increased creatinine levels, concentrated urine with low sodium excretion, and low urinary sodium excretion and has a very poor prognosis.
- Jaundice: Jaundice, or the yellowing of the skin and eyes, results from the accumulation of bilirubin in the blood due to the liver's impaired ability to process it.
- Portal hypertension: Portal hypertension refers to increased blood pressure in the portal vein, which can lead to serious complications, including ascites and variceal bleeding.
- Hepatopulmonary syndrome: Hepatopulmonary syndrome is characterised by lung dysfunction due to liver disease, leading to symptoms such as shortness of breath and reduced oxygen levels in the blood.
- Portopulmonary hypertension: Portopulmonary hypertension is a type of pulmonary hypertension associated with portal hypertension, causing increased pressure in the blood vessels of the lungs.
- Sarcopenia: Sarcopenia refers to the loss of muscle mass and strength, which can occur in patients with liver cirrhosis and contribute to overall frailty and decreased physical function.
- Increased risk of liver cancer: Individuals with liver cirrhosis face an increased risk of developing liver cancer, particularly hepatocellular carcinoma, due to ongoing liver damage and regeneration.
Preventing the progression of liver cirrhosis is crucial to minimising the risk of these potentially life-threatening complications.
Prevention of Liver Cirrhosis
Preventing liver cirrhosis involves addressing the underlying causes and risk factors associated with the condition. Some key strategies for preventing liver cirrhosis include:
- Limiting alcohol consumption: Excessive alcohol consumption is one of the leading causes of liver cirrhosis. Limiting or avoiding alcohol altogether can significantly reduce the risk of developing the condition.
- Maintaining a healthy weight: Obesity and being overweight are risk factors for non-alcoholic fatty liver disease (NAFLD), which can progress to cirrhosis. Maintaining a healthy weight through a balanced diet and regular exercise can help prevent NAFLD and subsequent cirrhosis.
- Managing chronic hepatitis: Chronic hepatitis B and C infections can lead to liver cirrhosis if left untreated. Regular monitoring, appropriate antiviral therapy, and adherence to treatment plans can help manage these infections and prevent the development of cirrhosis.
- Avoiding exposure to toxins: Exposure to certain toxins, such as industrial chemicals and certain medications, can damage the liver and increase the risk of cirrhosis. Taking precautions to avoid or minimise exposure to these toxins can help protect the liver.
- Vaccinations: Getting vaccinated against hepatitis A and B can prevent these viral infections, which can cause liver damage and increase the risk of cirrhosis.
Early detection and management of liver disease are crucial in preventing the progression of cirrhosis.
Diagnosis & Tests
Diagnosing liver cirrhosis involves a combination of physical examinations, laboratory tests, imaging studies, and, in some cases, a liver biopsy. These tests include:
- Physical examination: A doctor may perform a physical exam to look for signs of liver disease, such as jaundice, abdominal swelling (ascites), and enlarged liver or spleen.
- Blood tests: Blood tests can help assess liver function and identify underlying causes of liver damage. Common blood tests include liver function tests (LFTs), complete blood count (CBC), and tests for viral hepatitis.
- Imaging studies: Imaging studies, such as ultrasound, computed tomography (CT) scans, and magnetic resonance imaging (MRI), can help visualise the liver and assess its size, shape, and texture. These tests can also detect signs of cirrhosis, such as nodularity and portal hypertension.
- Liver biopsy: Liver biopsy is considered a gold standard for confirming cirrhosis, but non-invasive methods such as elastography and blood-based tests are increasingly used and may be preferred in many cases due to lower risk. During a biopsy, a small sample of liver tissue is removed and examined under a microscope.
- Elastography: Elastography is a non-invasive technique that measures liver stiffness, which can indicate the presence of fibrosis or cirrhosis. Techniques such as transient elastography (FibroScan) and acoustic radiation force impulse (ARFI) imaging are increasingly being used to assess liver fibrosis.
Treatment & Management
The management of liver cirrhosis focuses on addressing underlying causes, preventing disease progression, and managing complications. Here are the key treatment lines:
1. Antiviral Therapy for Hepatitis-Related Cirrhosis
For Hepatitis B, antiviral medications such as entecavir and tenofovir are preferred first-line therapies, while lamivudine and telbivudine are less commonly used due to resistance. These help suppress viral replication and slow disease progression. For Hepatitis C, direct-acting antivirals like sofosbuvir, velpatasvir, glecaprevir, and voxilaprevir effectively clear the infection and prevent further liver damage.
2. Diuretics for Ascites Management
Spironolactone (first-line) and furosemide (added if needed) help reduce fluid accumulation in the abdomen by promoting urination, thereby helping reduce fluid accumulation due to liver dysfunction.
3. Hepatic Encephalopathy Treatment
Lactulose, a non-absorbable disaccharide, is the first-line treatment to lower ammonia levels, while rifaximin, an antibacterial medicine, is often added to prevent recurrence.
4. Antibiotics for Infection Control
Third-generation cephalosporins such as ceftriaxone are commonly used as first-line treatment for spontaneous bacterial peritonitis (SBP), while fluoroquinolones like ciprofloxacin and levofloxacin may be used for prophylaxis in selected patients.
5. Steroids for Autoimmune Liver Disease
Prednisolone is commonly used in autoimmune hepatitis to reduce inflammation and prevent further liver damage.
6. Hepatoprotective and Supportive Agents
Ursodeoxycholic acid (UDCA) is primarily indicated for cholestatic liver diseases (e.g., primary biliary cholangitis) and is not routinely recommended for cirrhosis unless a specific indication exists.
Ademetionine, metadoxine, and methionine may support liver function; however, evidence for routine use in cirrhosis is limited.
7. Beta-Blockers for Portal Hypertension
Non-selective beta-blockers like propranolol and nadolol are used for primary and secondary prevention of variceal bleeding by reducing portal pressure.
When to See a Doctor?
If you experience any signs or symptoms of liver cirrhosis, it is essential to consult a doctor promptly. Early signs may include fatigue, weakness, loss of appetite, and unintentional weight loss. As the disease progresses, more severe symptoms can develop, such as jaundice, abdominal pain, swelling in the legs and abdomen, confusion, and bleeding or bruising easily. Regular check-ups with your doctor are crucial for monitoring the progression of cirrhosis and managing complications effectively.
Key Takeaways
- Liver cirrhosis management involves addressing the underlying cause and preventing further liver damage.
- Treatment for the underlying cause may include alcohol cessation, weight loss, blood sugar control, and medications for hepatitis B or C and other liver diseases.
- Complications of cirrhosis, such as ascites, hepatic encephalopathy, portal hypertension, infections, and hepatorenal syndrome, require specific management strategies.
- Medication plays a crucial role in managing cirrhosis and its complications, including diuretics, lactulose, rifaximin, beta-blockers, antibiotics, and antiviral medications.
- Early recognition of signs and symptoms and regular check-ups with a doctor are essential for effectively managing liver cirrhosis and its complications.
FAQs
How long can you live with liver cirrhosis?
Can liver cirrhosis be reversed?
What is the best treatment for liver cirrhosis?
How many stages are there in liver cirrhosis?
What are the symptoms associated with the different stages of liver cirrhosis?
Can a liver fully recover from cirrhosis?
Is death from liver failure a prolonged process?
Is liver cirrhosis a lifelong condition?
Can cirrhosis be cured?
At what age does cirrhosis start?
References
- European Association for the Study of the Liver. (2025). EASL Clinical Practice Guidelines on abdominal extrahepatic surgery in cirrhosis and advanced chronic liver disease. https://easl.eu/publication-category/clinical-practice-guidelines/
- Fadlallah, H. (2025). Update on the Complications and Management of Liver Cirrhosis. Journal of Clinical Medicine, 14(3), 456–470. https://pmc.ncbi.nlm.nih.gov/articles/PMC11843904/
- Singh, J. (2023). Advances in the management of complications from cirrhosis. Gastroenterology, 165(6), 1423–1435. https://academic.oup.com/gastro/article/doi/10.1093/gastro/goae072/7727525
- Arroyo, V. (2020). Grading and staging of liver diseases. Hepatology Textbook. https://www.hepatologytextbook.com/book/chapter_08.php
Check Related Salts
Browse Other Conditions
Latest health articles
Top Health Essentials
Disclaimer
Top-Selling Medicines:
...View more
Top-OTC medicines:
...View more
Company
About UsHealth ArticleHealth StoriesHealth LibraryDiseases & Health ConditionsAyurvedaUnderstanding Generic MedicinesAll MedicinesAll BrandsNeed HelpFAQSecuritySavings CalculatorSubscribe
Registered Office Address
Grievance Officer
Download Truemeds
Contact Us
Our customer representative team is available 7 days a week from 9 am - 9 pm.
v4.23.0
2026 - Truemeds | All rights reserved. Our content is for informational purposes only. See additional information.
Our Payment Partners
















































