Jaundice
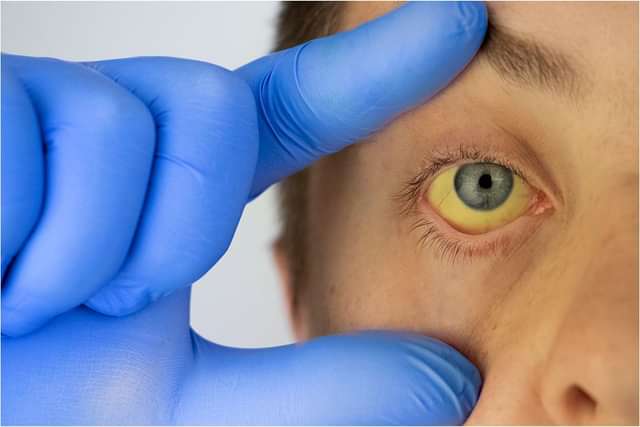
Jaundice, or hyperbilirubinemia, is the yellow discolouration of the eyes, skin, or mucous membrane that occurs due to elevated bilirubin levels in the blood. It is common in newborns, less common in older children, and frequently seen in adults. It can be a sign of something serious, such as liver disease, gallbladder issues, or bile duct obstruction. It results from increased bilirubin production or impaired excretion. Jaundice can be a sign of an underlying health problem, and it is important to seek medical attention to determine the cause.
Last updated on : 17 Apr, 2026
Read time : 16 mins
Overview of Disease
Jaundice (Piliya) occurs when the skin or the whites of the eyes turn yellow. It primarily occurs due to elevated bilirubin levels. The condition primarily affects the liver. It occurs more commonly in newborns but can also occur in adults.
This overview will help you review the jaundice definition, types, management, diagnosis, key facts, and other crucial aspects of the condition, equipping readers with the insights needed to understand and manage it.
What is Jaundice (Piliya)?
Jaundice is a clinical sign characterised by the yellowing of the skin, sclerae, and mucous membranes due to an excessive buildup of bilirubin, a byproduct of red blood cell breakdown (MedlinePlus). It is a clinical manifestation rather than a disease, as it mainly reflects disorders affecting the liver and biliary system. It is not contagious and occurs due to impaired bilirubin metabolism or excretion caused by underlying conditions.
It often affects newborn babies. About 50%–60% of newborns develop jaundice, sometimes referred to as icterus, during the first few days of life. In adults, it is less common but usually indicates an underlying medical condition (Ullah et al., 2016).
Jaundice, caused by bilirubin buildup, is associated with serious conditions like alcohol-related liver disease, gallstones, hepatitis, pancreatitis, or sickle cell disease, with treatments varying depending on the cause. This condition is often a sign of an underlying disease, so prompt diagnosis and appropriate management of jaundice depend on an awareness of the causes, risk factors, and symptoms associated with the condition.
Key Factors about Jaundice
| Category | Details |
| Also Referred to as | Piliya, icterus |
| Commonly Occurs In | Neonates, but also in adult men and women |
| Affected Organs | Liver, gallbladder, and biliary system |
| Type | Manageable (depends on underlying cause) |
| Common Signs | Yellowing of the skin, eyes, and mucous membranes, fever, loss of appetite, weakness, itching, abdominal pain, chills, dark urine, confusion (in severe cases), and irritability |
| Specialist | Physician, Gastroenterologist or Hepatologist |
| Treatment Procedure | Management includes treating the underlying cause, antihistamines (for itching), phototherapy (in neonates), and surgical intervention (in obstructive causes) |
| Management | Ursodeoxycholic acid, Cholestyramine and symptomatic management |
| Diagnosis | CBC, SGOT, SGPT, bilirubin levels, imaging (ultrasound/CT), hepatitis tests, prothrombin time, and biopsy |
| Prevention | Maintaining a healthy lifestyle, limiting alcohol consumption, and ensuring early diagnosis and treatment |
| Prevalence | Neonatal jaundice affects roughly 5–6 per 1,000 children under five years, while in the general population, it is approximately 2–3 per 1,000 individuals |
| Home Remedies | Consume sugarcane juice, eat light meals, limit fatty foods, stay hydrated, consume fruits and vegetables, and take adequate rest |
Types of Jaundice
Jaundice can be categorised into three main types, based on where bilirubin accumulates in the body. A blood test can help identify the specific type.
- Prehepatic: Prehepatic jaundice occurs when bilirubin accumulates before reaching the liver. This indicates that red blood cells are being broken down, producing more bilirubin than the liver is able to handle.
- Hepatic: Hepatic jaundice refers to the condition in which the liver is unable to process bilirubin effectively.
- Posthepatic (Obstructive): When bilirubin accumulates after passing through the liver and the body is unable to remove it at a sufficient rate, this is known as posthepatic jaundice, also called obstructive jaundice. It may occur due to bile duct blockage (e.g., gallstones or tumours).
Early Signs of Jaundice
Early signs of jaundice include mild yellowing of the sclera, skin, and dark urine; fatigue; abdominal discomfort; and loss of appetite. In some cases, jaundice may be asymptomatic. The most common sign is the yellowing of the sclera, skin, and mucous membranes. [NHS, 2024].
Symptoms of Jaundice
General Symptoms are as Follows:
- Fever
- Stomach pain
- Chills
- Dark urine
- Clay-coloured stools
- Loss of appetite
- Weakness
- Itchy skin
- Vomiting (may occur in severe conditions)
- Confusion
- Drowsiness
- Weight loss
- Irritability
- Bruising and bleeding
- Flu-like symptoms (typically associated with underlying infections such as viral hepatitis)
Stages of Jaundice
The development of jaundice involves three main stages: (Fan Y, 2023)
1. Prehepatic Stage (Before the Liver)
In this stage, red blood cells break down naturally after about 120 days or when damaged. This breakdown happens in the reticuloendothelial system, mainly in the spleen. When red blood cells break, they release a protein called haemoglobin into the bloodstream.
Haemoglobin is then split into two parts:
- Heme (which contains iron)
- Globin (a protein)
The heme part is broken down further:
- First, it is converted into biliverdin (a green pigment) by an enzyme called heme oxygenase.
- Then, biliverdin is converted into bilirubin (a yellow pigment) by biliverdin reductase.
Most bilirubin in the body is produced this way. A small amount also comes from the breakdown of other heme-containing proteins, such as muscle myoglobin and cytochromes. This type of bilirubin is called unconjugated bilirubin, and it is not water-soluble, so it travels in the blood attached to a protein called albumin.
2. Hepatic Stage (In the Liver)
When unconjugated bilirubin reaches the liver, it is processed by an enzyme called UDP-glucuronosyltransferase (UGT). This enzyme converts it into a water-soluble form called conjugated bilirubin (also known as bilirubin diglucuronide).
This conversion is essential because the body can only remove bilirubin once it becomes water-soluble. The liver then releases this conjugated bilirubin into the bile, which is stored in the gallbladder.
3. Posthepatic Stage (After the Liver)
When bile is released into the intestines during digestion, it carries conjugated bilirubin into the gut. In the intestines, natural bacteria convert bilirubin into a compound called urobilinogen.
From here:
- Most urobilinogen is turned into stercobilin, which gives faeces their brown colour.
- Some urobilinogen is reabsorbed into the bloodstream and returns to the liver.
A small amount is filtered by the kidneys and excreted in urine as urobilin, giving urine its yellow colour.
Causes of Jaundice
There are multiple causes of jaundice, such as alcoholism, hepatitis, genetic conditions, and other systemic conditions, as discussed below.
- Hepatitis: Liver inflammation, which can result from a virus, an autoimmune illness, alcohol or medicine consumption, blood transfusion, or chemical exposure, is known as hepatitis. It could be chronic, meaning it lasts at least six months, or acute, meaning it lasts for a short duration. Jaundice can result from liver injury caused by prolonged inflammation.
- Alcohol-related liver disease: Consistent heavy drinking over an extended period, usually eight to ten years, can seriously harm the liver. The liver is mainly affected by two conditions: alcoholic hepatitis and alcoholic cirrhosis, which could lead to jaundice and associated symptoms.
- Other liver diseases: Hepatitis, autoimmune disorders, and genetic disorders that run in your family can all lead to cirrhosis. Nonalcoholic fatty liver disease can lead to a serious condition called nonalcoholic steatohepatitis. In this type of liver illness, fat accumulation in the liver is accompanied by inflammation, leading to progressive liver damage.
- Blocked bile ducts: These are narrow tubes that transport bile, a fluid produced by the liver and gallbladder, to the small intestine. Jaundice can occur if gallstones, cancer, inflammation, or rare liver disorders obstruct the bile ducts.
- Pancreatic cancer: It can obstruct the bile duct, resulting in jaundice.
- Specific medications: Liver illness has been associated with certain medicines, including steroids, birth control pills, penicillin, and acetaminophen, which could cause liver injury and may lead to jaundice.
- Blood clots: Bilirubin levels might rise if the body reabsorbs a large blood clot (haematoma) beneath the skin, but this is uncommon.
- Haemolytic anaemia: The body occasionally eliminates damaged blood cells from circulation too quickly, which raises bilirubin levels.
- Gilbert's syndrome and Crigler-Najjar syndrome: As a result of impaired UGT1A1 activity, which is essential for bilirubin conjugation, these genetic liver disorders result in elevated blood levels of unconjugated bilirubin. Gilbert's syndrome is quite common and generally mild, and it is frequently discovered by chance during routine blood tests.
In contrast, Crigler-Najjar syndrome, especially Type I, is a rarer and more severe illness that can lead to dangerously high bilirubin levels, particularly in infants and newborns. Unlike Gilbert's syndrome, Crigler-Najjar often requires active management, such as phototherapy or, in severe cases, liver transplantation. - G6PD deficiency: Glucose-6-phosphate dehydrogenase (G6PD) deficiency is a common enzymatic disorder that can lead to haemolytic jaundice, especially in newborns or after exposure to certain medicines, foods, or infections.
Red blood cells rupture prematurely (haemolysis) in individuals with G6PD deficiency, releasing a large amount of heme and, consequently, unconjugated bilirubin, which the liver may have trouble processing quickly. This condition can lead to neonatal jaundice and requires prompt management to prevent complications such as kernicterus. - Breastfeeding Jaundice and Breast Milk Jaundice: These are two distinct kinds of neonatal jaundice. Breastfeeding jaundice, which is caused by insufficient milk intake that delays bilirubin clearance, typically manifests within the first week of life (CDC, 2025).
In contrast, breast milk jaundice appears after the first week and can linger for several weeks. It is believed that some of the substances found in breast milk interfere with the breakdown of bilirubin. Both conditions are usually mild and do not require stopping breastfeeding, but they do require monitoring to exclude more serious causes.
Risk Factors
The risk of developing jaundice depends on the underlying cause. If it is a virus, it may become chronic or spread. However, if the liver is failing due to jaundice, complications from your liver illness might include coma and even death.
- Alcohol Overuse: Excessive alcohol intake may predispose an individual to develop jaundice due to impaired liver function.
- Viral Infection: Hepatitis (i.e., liver inflammation) may lead to jaundice.
- Certain Cancers: Cancer of the pancreas, gall bladder, and liver may lead to jaundice.
- Neonates: Immature bilirubin metabolism may lead to elevated bilirubin levels.
- Liver Disease: Cirrhosis or other liver conditions may lead to jaundice due to bilirubin accumulation.
- Genetics: Genetic hyperbilirubinaemia (e.g., Gilbert’s or Dubin–Johnson syndrome) may cause jaundice
Who is at risk?
Newborn infants, patients with sickle cell anaemia, haemolytic anaemia, hepatitis, gallstones, alcohol dependence, autoimmune or genetic conditions, and pancreatic cancer are at a higher risk of developing jaundice.
Complications
- Neurological dysfunction: Neonates with significant hyperbilirubinaemia are at risk of developing bilirubin-induced neurologic dysfunction (BIND) (Ansong-Assoku et al., 2024).
- Kernicterus: This refers to the deposition of bilirubin in brain tissues, which is a severe form of bilirubin encephalopathy in untreated newborns (Ansong-Assoku et al., 2024).
- Liver failure or cirrhosis: It may lead to progressive chronic jaundice.
- Hepatic encephalopathy (HE): A neurological complication of advanced jaundice and liver failure is hepatic encephalopathy. When the liver cannot eliminate toxins such as ammonia and other waste products, these compounds build up and impair brain activity, causing disorientation, confusion, or even coma. Elevated bilirubin levels, especially the bilirubin/albumin ratio, may be associated with a greater risk of HE.
- Hepatorenal Syndrome (HRS): A type of kidney failure seen in people with advanced liver impairment and prolonged jaundice is called hepatorenal syndrome. Changes in circulation and vasoconstriction caused by liver failure reduce blood flow to the kidneys. Usually appearing in advanced cirrhosis or cholestatic jaundice, this condition is characterised by rapid loss of kidney function without structural kidney damage.
If jaundice is not treated promptly, the condition may worsen and lead to severe complications, including coma or death.
Prevention of Jaundice
The following are simple ways to help avoid most cases of jaundice.
- Avoid herbal supplements without medical advice, as some may harm the liver and cause jaundice.
- Refrain from smoking, drinking alcohol, and using intravenous substances.
- Do not take more than the prescribed dose of any medicine.
- See your physician if you observe yellowish discolouration on your skin or eyes.
- Practice safe sex to reduce the risk of hepatitis transmission (CDC, 2025).
- Jaundice due to hepatitis A and B is vaccine-preventable (CDC, 2025).
- Maintain a healthy weight.
- Promote awareness about the disease through education and counselling activities.
- Before travelling abroad, ensure you receive the recommended vaccinations.
- Maintain healthy cholesterol levels.
- Avoid excessive intake of fatty foods, dairy products, and cheese.
- Ensure timely and recommended vaccinations, especially when travelling.
Diagnosis & Tests
Diagnosis of jaundice involves a clinical evaluation, followed by laboratory tests and imaging to confirm the presence of jaundice, identify its underlying cause, and assess the extent of liver involvement.
- Physical Examination and Medical History: The diagnostic process usually starts with a careful assessment of symptoms and medical history. Your doctor will enquire about recent infections, alcohol intake, family history of liver disease, and medicine use. The doctor will look for yellowing of the skin and eyes and examine the abdomen to detect swelling or tenderness in the liver region.
- Blood Tests for Bilirubin Levels: Blood tests will be ordered by your physician to confirm jaundice and assess its severity. Measurements of total and direct bilirubin levels, liver function tests, and a complete blood count (CBC) are included in these tests. Jaundice is marked by elevated bilirubin levels, indicating that the liver is not properly removing or processing bilirubin.
- Hepatitis Panel: This blood investigation detects hepatitis A, B, and C infections (MedlinePlus). If antibodies for these viruses are found, it might mean either ongoing infection or past exposure. Absence of antibodies may suggest no prior exposure or resolved infection.
- Tests for Liver Enzymes: Liver function is evaluated based on the levels of several enzymes found in the liver, such as alanine aminotransferase (ALT), aspartate aminotransferase (AST), alkaline phosphatase (ALP), and gamma-glutamyl transferase (GGT) (NCBI, 2023). Abnormal levels of these enzymes may indicate liver inflammation, damage, or bile duct obstruction, all of which can lead to jaundice.
- Scans: Imaging examinations are frequently undertaken to provide a better view of the bile ducts and liver. Imaging is vital for detecting tumours, gallstones, or liver enlargement; it includes ultrasound, CT scans, and magnetic resonance cholangiopancreatography (MRCP), a specialised MRI that assesses structural blockages or narrowing in the gallbladder and bile ducts.
- Biopsy: Your doctor might advise a liver biopsy in certain situations to assess liver tissue under a microscope. A needle inserted through the skin, a vein in the neck, or a surgical incision is used to get a little tissue sample. This test assists in determining the degree of liver damage and provides detailed information on liver diseases, including cirrhosis, hepatitis, or cancer.
- Prothrombin Time (PT): A blood test called prothrombin time examines how long your blood takes to clot. A prolonged clotting time may indicate impaired liver function, as the liver produces most of the proteins needed for blood clotting. The typical PT range is approximately 10–13 seconds. Prolongation may indicate reduced liver synthetic function.
Treatment & Management
Jaundice itself is a clinical sign rather than a disease, so management focuses on treating the underlying cause and providing supportive care.
- Due to Viral Hepatitis: Jaundice often resolves as liver function improves in acute viral hepatitis (MedlinePlus). Supportive care and monitoring are usually sufficient.
- Due to a Blocked Bile Duct: If jaundice is caused by bile duct obstruction, your doctor may recommend procedures such as endoscopic removal or surgery to relieve the blockage.
- Itching (Pruritus): Cholestyramine may be prescribed to relieve itching by binding bile acids and reducing their accumulation in the body (Paumgartner & Beuers, 2002).
- Medication: Ursodeoxycholic acid may help improve bile flow and protect liver cells from bile acid toxicity (Paumgartner & Beuers, 2002).
Note: This medication requires proper dosing based on body weight and underlying condition. Regular monitoring of liver function is necessary during treatment.
- Phototherapy for Jaundice: Phototherapy uses blue-spectrum light to convert bilirubin into a form that can be easily excreted. It is primarily indicated in neonatal jaundice (Ansong-Assoku et al., 2024).
- Supportive Care: Eat home-cooked meals, follow a low-fat diet, maintain hygiene, take adequate rest, and stay well hydrated. Fruits such as sugarcane may be consumed in moderation for hydration support.
- Lifestyle Measures: Limiting alcohol intake, getting vaccinated against hepatitis, and reducing high-fat food intake can help manage underlying liver conditions and prevent worsening.
Disclaimer: Home remedies are supportive measures only and do not replace medical treatment. Always consult your healthcare provider before implementing any home care regimen.
Living with Jaundice
Until the symptoms subside, regular monitoring of liver function tests (SGOT, SGPT), complete blood count (CBC), adherence to prescribed medicines, maintaining a balanced diet with light foods, patient education, limiting alcohol intake, maintaining hygiene to prevent infections, and following a healthy lifestyle are recommended.
When to See a Doctor?
Early detection and treatment of jaundice are crucial to identify the underlying cause and manage the condition effectively.
Seek medical attention if dark urine, pale stools, abdominal pain, fever, or mental changes persist for more than a few days or worsen over time.
Key Takeaways
- Elevated bilirubin levels cause jaundice. Bilirubin is the waste product of red blood cells, which is processed by the liver for excretion. Elevated bilirubin levels lead to yellowing of the skin, eyes, and mucous membranes, which is the first indication of the condition. It should be reported to a physician for prompt and timely management. Regular monitoring of bilirubin levels and blood parameters should be done to prevent complications.
- Maintaining adequate hydration is important; fluids such as water and oral rehydration options can help support recovery.
- Once the condition is confirmed, stay hydrated, take rest, and take home-cooked light foods like khichdi, fruits, vegetables, and juices.
- Monitor complete blood counts, bilirubin levels, and swelling or tenderness in the liver region.
- Timely treatment is needed for newborns to avoid encephalopathy.
- Limit alcohol and high-fat foods.
Disclaimer: This information is for educational purposes only and should not replace professional medical advice. Always consult with qualified healthcare providers for diagnosis, treatment, and medical decisions regarding jaundice or any other health condition.
FAQs
What is jaundice?
What is bilirubin?
How do infectious and non-infectious causes differ from one another?
How can prehepatic, hepatic, and posthepatic jaundice be distinguished?
Which diet is best for jaundice patients?
Can a newborn have jaundice?
Is jaundice contagious?
Is it possible to cure jaundice?
What are the dietary restrictions for a patient with jaundice?
Can jaundice cause death?
Why is there dark urine in jaundice?
References
- National Health Service (NHS). (2024). Jaundice. https://www.nhs.uk/conditions/jaundice/
- MedlinePlus. (2025). Jaundice (Icterus). U.S. National Library of Medicine. https://medlineplus.gov/jaundice.html
- MedlinePlus. (2025). Jaundice causes. U.S. National Library of Medicine. https://medlineplus.gov/ency/article/007491.htm
- Ansong-Assoku, B., Adnan, M., Daley, S. F., & Ankola, P. A. (2024). Neonatal jaundice. StatPearls Publishing. https://www.ncbi.nlm.nih.gov/books/NBK532930/
- Centers for Disease Control and Prevention (CDC). (2025). Viral hepatitis and jaundice. https://www.cdc.gov/hepatitis/
- National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK). (2023). Liver disease and jaundice.https://www.niddk.nih.gov/health-information/liver-disease
- Paumgartner, G., & Beuers, U. (2002). Ursodeoxycholic acid in cholestatic liver disease: Mechanisms of action and therapeutic use revisited. Hepatology, 36(3), 525–531. https://doi.org/10.1053/jhep.2002.36088
Browse Other Conditions
Latest health articles
Top Health Essentials
Disclaimer
Top-Selling Medicines:
...View more
Top-OTC medicines:
...View more
Company
About UsHealth ArticleHealth StoriesHealth LibraryDiseases & Health ConditionsAyurvedaUnderstanding Generic MedicinesAll MedicinesAll BrandsNeed HelpFAQSecuritySavings CalculatorSubscribe
Registered Office Address
Grievance Officer
Download Truemeds
Contact Us
Our customer representative team is available 7 days a week from 9 am - 9 pm.
v4.23.1
2026 - Truemeds | All rights reserved. Our content is for informational purposes only. See additional information.
Our Payment Partners
















































