Pancreatitis
Pancreatitis is a serious condition involving inflammation of the pancreas, an organ crucial for digestion and blood sugar regulation. It can be acute (sudden and short-term) or chronic (long-lasting) and is often caused by factors such as gallstones, alcohol use, gallstones, alcohol use, hypertriglyceridemia, medications, infections, post-ERCP complications, or genetic disorders. Treatment typically involves managing symptoms, providing supportive care, and addressing the underlying cause.
Last updated on : 30 Apr, 2026
Read time : 12 mins
Overview of Disease
Pancreatitis is a serious health issue that affects the pancreas, a vital organ located behind the stomach. The pancreas plays a crucial role in digestion and blood sugar regulation by producing digestive enzymes and hormones like insulin. When the pancreas becomes inflamed, it can lead to a range of symptoms and complications that require prompt medical attention. In this article, we will explore the causes, symptoms, stages, and treatment options for pancreatitis.
What is Pancreatitis?
Pancreatitis is the inflammation of the pancreas, which can occur suddenly (acute pancreatitis) or develop over time (chronic pancreatitis). One common cause of pancreatitis is gallstone pancreatitis, which happens when a gallstone blocks the pancreatic duct, leading to premature activation of digestive enzymes within the pancreas, resulting in inflammation. Other factors that can contribute to pancreatitis include heavy alcohol use, certain medications, infections, and genetic disorders. Understanding the underlying cause of pancreatitis is essential for determining the most appropriate treatment approach.
Key Factors about Pancreatitis
| Category | Details |
| Also Referred to as | Gallstone Pancreatitis, Pancreas Inflammation |
| Commonly Occurs In | Adults, particularly men, more often than women |
| Affected Organ | Pancreas |
| Type | Acute Pancreatitis, Chronic Pancreatitis |
| Common Signs | Abdominal Pain Radiating to the Back, Nausea, Vomiting, Fever, Abdominal Swelling, and Tenderness |
| Consulting Specialist | Gastroenterologist, General Surgeon |
| Treatment Procedures | IV Fluids, Pain Medication, Antibiotics, Nasogastric Tube, ERCP, Surgery |
| Managed By | Intravenous fluids, Medications such as acetaminophen, opioids, or non-steroidal anti-inflammatory drugs (NSAIDs) |
| Mimicking Condition | Cholecystitis, Appendicitis, Peptic Ulcer Disease, Gastroesophageal Reflux Disease |
Types of Pancreatitis
There are several different types of pancreatitis, each with its own characteristics:
- Acute pancreatitis: This is a sudden inflammation of the pancreas that typically lasts for a short period. It can range from mild discomfort to a severe, life-threatening condition. Most people with acute pancreatitis recover completely with supportive care.
- Chronic pancreatitis: This is a long-term, progressive condition characterised by ongoing inflammation and scarring of the pancreas. Over time, it can lead to permanent damage and impairment of the pancreas's functions.
- Autoimmune pancreatitis: In this type, the body's immune system mistakenly attacks the pancreatic tissue, causing inflammation.
- Hereditary pancreatitis: This inherited form of pancreatitis can cause recurrent episodes of acute pancreatitis and may progress to chronic pancreatitis over time.
Understanding the different types of pancreatitis is important for accurate diagnosis and appropriate management of the condition.
Symptoms of Pancreatitis
The symptoms of pancreatitis can vary depending on whether it is acute or chronic. Some of the common symptoms include:
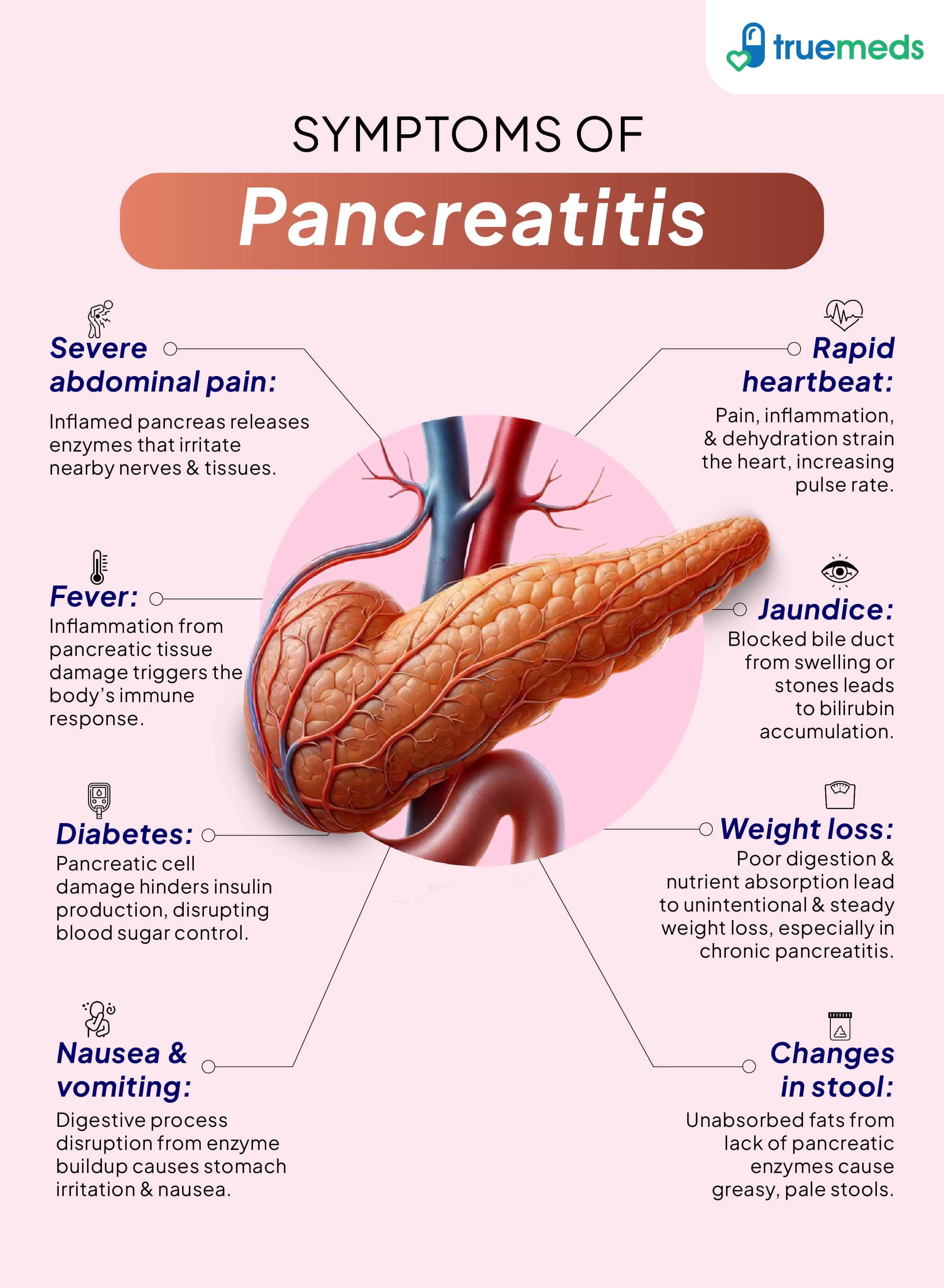
- Severe abdominal pain: Pancreatitis often causes intense upper abdominal pain that may radiate to the back. The pain is persistent and can worsen after eating, especially fatty foods.
- Nausea and vomiting: Nausea and vomiting are common, contributing to dehydration and a decreased appetite, which complicate the condition.
- Fever: A fever can develop in response to inflammation or infection associated with pancreatitis, signalling systemic effects and the body’s response to the inflammation.
- Rapid heartbeat: An elevated heart rate may occur as part of the body's response to inflammation and fever in pancreatitis, indicating a potential systemic reaction.
- Weight loss: Weight loss often results from a significant loss of appetite and the body's inability to effectively absorb nutrients due to impaired pancreatic function.
- Changes in stool: Stool may become pale, greasy, and foul-smelling due to the pancreas’s diminished production of digestive enzymes, leading to poor fat absorption.
- Jaundice: Jaundice, characterised by yellowing of the skin and eyes, can develop if inflammation affects the bile ducts, leading to a buildup of bilirubin in the blood.
- Diabetes: Chronic pancreatitis can damage insulin-producing cells in the pancreas, potentially leading to diabetes, with symptoms such as increased thirst, frequent urination, and unexplained weight loss.
Stages of Pancreatitis
The two major forms, acute and chronic, have distinct staging:
Acute Pancreatitis
There are 3 stages of Acute Pancreatitis:
- Stage 1 Mild AP
It is the most common form, with no organ failure, no local or systemic complications; it usually resolves within the first week. Around 80% of all cases fall into this category, with only interstitial changes in the pancreas.
- Stage 2 Moderately Severe AP
It is characterised by transient local or systemic complications or transient organ failure lasting fewer than 48 hours. Necrotising pancreatitis, involving pancreatic or peripancreatic tissue death, is typically seen at this stage.
- Stage 3 Severe AP
It is defined by single or multiple organ failure persisting for more than 48 hours.
Chronic Pancreatitis
Chronic pancreatitis is the end-stage of continuous inflammation and fibrosis, evolving from acute, recurrent acute, early, and finally end-stage disease. There are four stages of CP:
- Stage-1 At Risk
The individual is asymptomatic before the first pancreatic injury but carries genetic, environmental, or lifestyle risk factors.
- Stage-2 Acute Recurrent Acute Pancreatitis
The first (sentinel) episode of acute pancreatitis occurs, followed by recurrent episodes. Early detection and prevention are critical here, given the irreversible nature of established chronic pancreatitis.
- Stage-3 Early Chronic Pancreatitis
At this stage, the condition may either resolve or progress if further injury or stress occurs. Early diagnosis at this point, before irreversible damage sets in, represents a critical and currently unmet challenge, as imaging often cannot yet detect the subtle structural changes.
- Stage-4 Established to End-Stage Chronic Pancreatitis
End-stage chronic pancreatitis is characterised by pancreatic atrophy, fibrosis, pain syndromes, duct distortion and strictures, calcifications, and both exocrine and endocrine dysfunction. Clinically, this means malabsorption and type 3c diabetes (pancreatogenic diabetes). Exocrine insufficiency occurs when over 90% of the organ is damaged, affecting up to 85% of patients with severe disease.
Causes of Pancreatitis
Several factors can contribute to the development of pancreatitis, including:
- Gallstones: Gallstone pancreatitis is the most common cause of acute pancreatitis. It occurs when a gallstone blocks the pancreatic duct, leading to inflammation.
- Alcohol use: Long-term, heavy alcohol consumption is a leading cause of chronic pancreatitis. Alcohol can damage pancreatic cells and lead to inflammation.
- High triglycerides: Hypertriglyceridemia, or elevated levels of triglycerides in the blood, can trigger pancreatitis.
- Genetic factors: Certain inherited genetic mutations, such as in the PRSS1, SPINK1, CFTR, and CTRC genes, can increase the risk of developing pancreatitis.
- Autoimmune disorders: In some cases, the immune system mistakenly attacks the pancreas, causing inflammation and pancreatitis.
- Infections: Viral infections like mumps, hepatitis A, and cytomegalovirus (CMV) can sometimes lead to pancreatitis.
- Medications: Certain medications, such as oestrogens, corticosteroids, and some antibiotics, may cause an increased risk of pancreatitis.
- Abdominal trauma or surgery: Injury to the pancreas or surgical procedures near the organ can trigger inflammation.
By understanding these potential causes, doctors can better diagnose and treat pancreatitis, as well as recommend preventive measures for at-risk individuals.
Risk Factors
Several factors can increase the risk of developing pancreatitis. Some of the most common risk factors include:
- Excessive alcohol consumption
- Gallstones
- Certain inherited genetic disorders, such as cystic fibrosis
- Smoking
- Being overweight or obese
- Severe abdominal injuries
- Some medications, including certain antibiotics, diuretics, and immunosuppressants
- Hypertriglyceridaemia (especially >1000 mg/dL)
Understanding these risk factors can help in identifying individuals who may be more susceptible to developing pancreatitis.
Complications
Pancreatitis can lead to several serious complications, especially if left untreated or if the condition becomes chronic. Some of the potential complications include:
- Pseudocysts: Fluid-filled sacs that can develop in the pancreas, which may become infected or rupture, causing further complications.
- Pancreatic necrosis: Severe inflammation can cause portions of the pancreas to die, leading to infection and potentially life-threatening complications.
- Organ failure: In severe cases, pancreatitis can cause multi-organ failure, affecting the lungs, kidneys, and cardiovascular system (Tenner et al., 2024).
- Malnutrition: Chronic pancreatitis can lead to malabsorption of nutrients, as the damaged pancreas may not produce enough digestive enzymes.
- Diabetes: Damage to the insulin-producing cells in the pancreas can result in the development of diabetes.
- Pancreatic cancer: Chronic pancreatitis is associated with an increased risk of developing pancreatic cancer, although this is relatively rare.
Prompt diagnosis and appropriate treatment of pancreatitis are essential to minimise the risk of these complications and ensure the best possible outcomes for patients.
Prevention of Pancreatitis
While not all cases of pancreatitis can be prevented, there are several steps you can take to reduce your risk. These include:
- Limit alcohol consumption: If you choose to drink alcohol, do so in moderation. Heavy alcohol use is a leading cause of chronic pancreatitis.
- Maintain a healthy weight: Obesity increases your risk of gallstones and hypertriglyceridemia, both of which can lead to pancreatitis. Eating a balanced diet and exercising regularly can help you maintain a healthy weight.
- Quit smoking: Smoking is associated with an increased risk of pancreatitis. If you smoke, consider quitting or seeking help to stop.
- Stay hydrated: Drinking plenty of fluids, particularly water, can help prevent the formation of gallstones.
- Manage other health conditions: If you have other conditions that increase your risk of pancreatitis, such as autoimmune disorders or hypertriglyceridemia, work with your doctor to manage these effectively.
By making lifestyle changes and managing any underlying health conditions, you can significantly reduce your risk of developing pancreatitis (Tenner et al., 2024).
Diagnosis & Tests
Diagnosing pancreatitis involves a combination of clinical evaluation, laboratory tests, and imaging studies. These include:
- Medical history: A thorough evaluation begins with discussing symptoms like abdominal pain, nausea, and vomiting, along with any recent digestive changes. The doctor will also ask about risk factors such as alcohol use, recent abdominal trauma, and a history of gallstones or specific medications.
- Physical examination: The doctor will examine the abdomen for tenderness, swelling, or other signs like fever. This helps assess the severity of pancreatitis and identify potential complications.
- Amylase and lipase tests: Elevated levels of these pancreatic enzymes, particularly if ≥3 times the upper limit of normal, are a key diagnostic criterion for acute pancreatitis, but must be combined with clinical symptoms or imaging findings for confirmation (Cruz-Monserrate et al., 2021).
- Complete blood count (CBC): This test can reveal signs of infection or inflammation, like an elevated white blood cell count.
- Liver function tests: These help identify bile duct obstruction, a potential cause of pancreatitis.
- Ultrasound: An ultrasound may be used initially to evaluate the gallbladder for gallstones, which are a common cause of pancreatitis.
- Computed tomography (CT) scan: A CT scan can confirm pancreatitis and show complications such as necrosis or pseudocysts.
- Magnetic resonance imaging (MRI): MRI is useful for diagnosing pancreatitis, especially if bile duct obstruction is suspected.
- Magnetic resonance cholangiopancreatography (MRCP): Magnetic resonance cholangiopancreatography is useful for evaluating pancreatic and biliary ducts.
Treatment & Management
Treatment for pancreatitis depends on the type and severity of the condition. Some of the treatment options include:
1. Fluid Replacement
- Intravenous fluids are administered to prevent dehydration and maintain blood pressure.
2. Pain Management
- Paracetamol (Acetaminophen) is commonly used to relieve mild to moderate abdominal pain.
- Opioids such as morphine or fentanyl and Tramadol may be prescribed for more severe pain management.
3. Nutritional Support
- In mild acute pancreatitis, early oral feeding (within 24–48 hours) is recommended unless contraindicated. In severe cases, enteral nutrition via a nasogastric tube may be needed (Tenner et al., 2024).
4. Antibiotic Therapy
- Antibiotics are reserved for cases of infected pancreatic necrosis or confirmed infection, not for routine acute pancreatitis (Tenner et al., 2024).
5. Treating Underlying Causes
- ERCP is indicated only for gallstone pancreatitis with cholangitis or persistent biliary obstruction, not for uncomplicated cases (Cruz-Monserrate et al., 2021).
- Alcohol-induced pancreatitis requires complete abstinence from alcohol along with counseling or support programs.
6. Lifestyle Changes
- Patients should follow a low-fat diet and avoid smoking and alcohol consumption to prevent recurrent episodes.
7. Pancreatic Enzyme Replacement
- If the pancreas fails to produce enough digestive enzymes, supplemental pancreatic enzymes may be prescribed to aid digestion.
8. Managing Complications
- Diabetes caused by pancreatitis may require insulin therapy for blood sugar control.
- Pseudocysts that develop may need surgical or endoscopic drainage to prevent further complications.
9. Surgical Intervention
- In severe cases, surgery may be required to remove damaged pancreatic tissue or correct structural abnormalities.
- Endoscopic procedures can help manage complications, remove blockages, or drain fluid collections.
When to See a Doctor?
If you experience severe abdominal pain, especially if it radiates to your back, accompanied by nausea, vomiting, or fever, it is essential to seek medical attention promptly. These symptoms could indicate pancreatitis or another serious condition. Additionally, if you have chronic abdominal pain, unexplained weight loss, or persistent digestive issues, consult your doctor. Early diagnosis and intervention can prevent complications and improve outcomes in pancreatitis.
Key Takeaways
- Pancreatitis is an inflammation of the pancreas, which can be acute or chronic.
- Common causes include gallstones, alcohol abuse, and certain medications.
- Diagnosis involves clinical evaluation, laboratory tests (amylase, lipase, CBC, liver function), and imaging studies (CT, MRI).
- Treatment for acute pancreatitis focuses on supportive care, medications, and sometimes ERCP.
- Chronic pancreatitis management includes pain control, nutritional support, and occasionally surgery.
- Seek medical attention promptly for severe abdominal pain, nausea, vomiting, or fever.
- Early diagnosis and intervention are crucial for preventing complications and improving outcomes.
FAQs
Is pancreatitis a very serious condition?
Can pancreatitis be cured?
What is the main cause of pancreatitis?
Is pancreatitis a lifelong condition?
What foods cause pancreatitis?
Can the pancreas repair itself?
Can you live without a pancreas?
Does pancreatitis cause gas?
How to avoid pancreatitis?
References
- Tenner, S., Vege, S. S., & Yadav, D. (2024). Management of Acute Pancreatitis. American Journal of Gastroenterology, 119(4), 597–613. https://pubmed.ncbi.nlm.nih.gov/38857482/
- Cruz-Monserrate Z, Gumpper K, Pita V, Hart PA, Forsmark C, Whitcomb DC, Yadav D, Waldron RT, Pandol S, Steen H, Anani V, Kanwar N, Vege SS, Appana S, Li L, Serrano J, Rinaudo JAS, Topazian M, Conwell DL; Consortium for the Study of Chronic Pancreatitis, Diabetes, and Pancreatic Cancer. Biomarkers of Chronic Pancreatitis: A Systematic Literature Review. Pancreatology. 2021 Mar;21(2):323-333. doi: 10.1016/j.pan.2021.01.006 https://pubmed.ncbi.nlm.nih.gov/33558189/
- Xu, B., et al. (2025). Global Burden of Pancreatitis Among Individuals Aged 15–99 Years: A Systematic Analysis. EClinicalMedicine, 73, 103018. https://pmc.ncbi.nlm.nih.gov/articles/PMC12150401/
- Garami, A., et al. (2023). The Future of Acute Pancreatitis Care. Function, 4(3), zqad015. https://doi.org/10.1093/function/zqad015
- Párniczky, A., et al. (2025). International Association of Pancreatology Revised Guidelines for Acute Pancreatitis. Pancreatology, 25(2), 147–155. https://doi.org/10.1016/j.pan.2025.01.005
Latest health articles
Top Health Essentials
Disclaimer
Top-Selling Medicines:
...View more
Top-OTC medicines:
...View more
Company
About UsHealth ArticleHealth StoriesHealth LibraryDiseases & Health ConditionsAyurvedaUnderstanding Generic MedicinesAll MedicinesAll BrandsNeed HelpFAQSecuritySavings CalculatorSubscribe
Registered Office Address
Grievance Officer
Download Truemeds
Contact Us
Our customer representative team is available 7 days a week from 9 am - 9 pm.
v4.22.3
2026 - Truemeds | All rights reserved. Our content is for informational purposes only. See additional information.
Our Payment Partners
















































