Coeliac Disease Sprue
Coeliac disease sprue is a chronic autoimmune disorder that affects the small intestine in genetically predisposed individuals who develop an intolerance to gluten. When individuals with coeliac disease consume gluten, their immune system reacts by damaging the lining of the small intestine, leading to malnutrition and various symptoms. The primary treatment for coeliac disease is a strict, lifelong gluten-free diet (ACG Clinical Guidelines, 2023).
Last updated on : 22 Apr, 2026
Read time : 13 mins
Overview of Disease
Coeliac disease sprue is a chronic autoimmune disorder that affects the small intestine, causing inflammation and damage to the villi when gluten is consumed. This condition can lead to a wide range of symptoms and complications, making it essential for individuals with coeliac disease to adhere to a strict gluten-free diet. In this article, we will explore the various aspects of coeliac disease sprue, including its causes, symptoms, diagnosis, and treatment options.
What is Coeliac Disease Sprue?
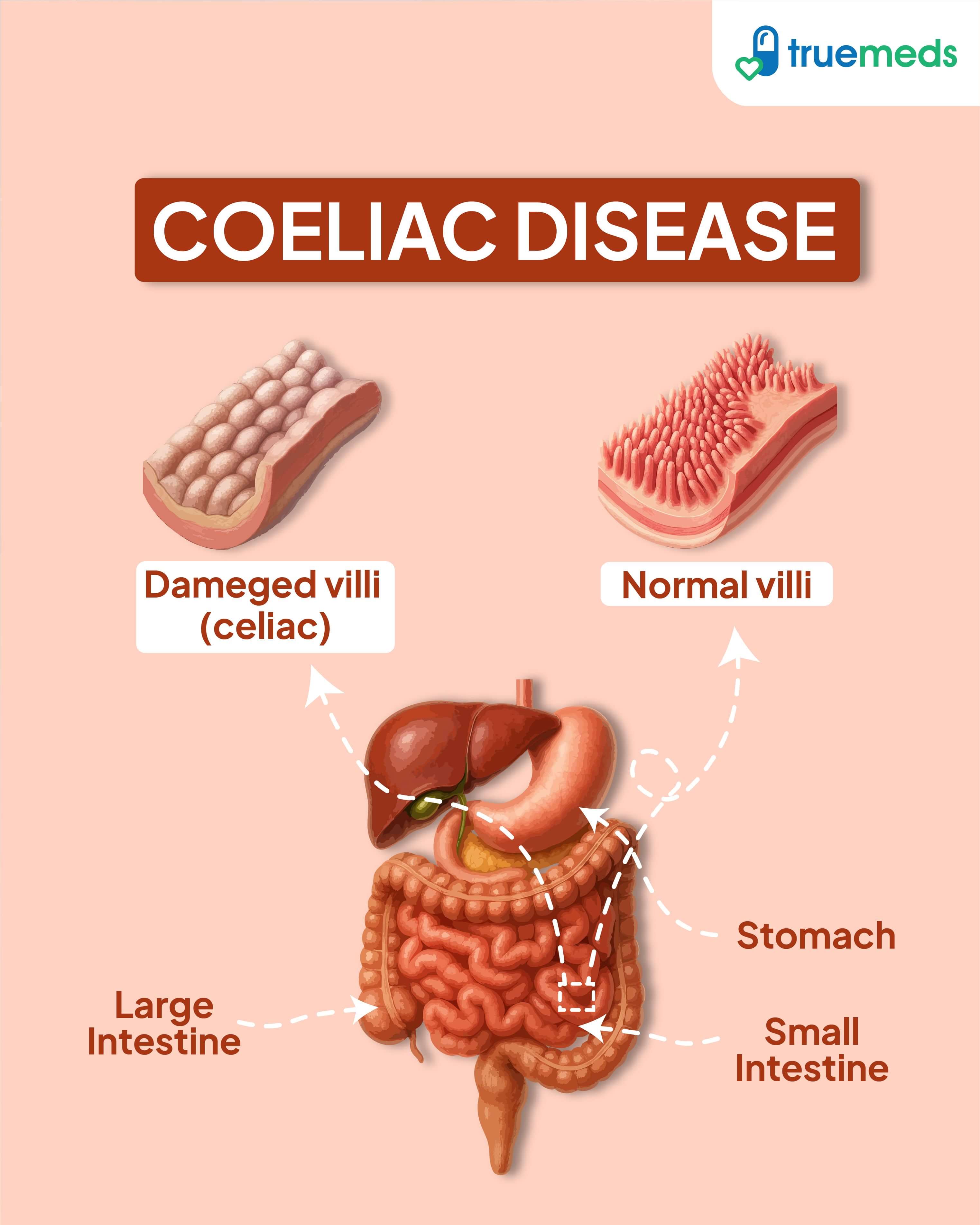
Coeliac disease sprue is an autoimmune condition in which the body's immune system mistakenly attacks the small intestine when gluten is consumed. Gluten is a protein found in wheat, barley, rye, and other grains. The immune system's reaction to gluten leads to inflammation and damage to the villi, small finger-like projections lining the small intestine. This damage impairs the absorption of nutrients, causing various symptoms and potential complications. Coeliac disease is a genetic condition that can develop at any age, and symptoms may vary significantly from one individual to another.
Key Factors about Coeliac Disease Sprue
| Category | Details |
| Also Referred as | Coeliac sprue, nontropical sprue, gluten-sensitive enteropathy |
| Commonly Occurs In | Genetically predisposed individuals, Europeans, those with family history, certain autoimmune disorders |
| Affected Organ | Small intestine |
| Type | Autoimmune disorder |
| Common Signs | Diarrhoea, lethargy, abdominal distension and discomfort/pain, vomiting, constipation, unexplained weight loss, iron deficiency anaemia, ataxia, chronic headaches, delayed menarche |
| Consulting Specialist | Gastroenterologist |
| Treatement Procedures | Lifelong gluten-free diet, vitamin and mineral supplements |
| Managed By | Nutritional supplements (e.g., iron or vitamin D) |
| Mimiciking Condition | Irritable bowel syndrome (IBS), microscopic colitis, other autoimmune disorders |
Symptoms of Coeliac Disease Sprue
The symptoms of coeliac disease sprue can vary widely among individuals and may affect different parts of the body. Some common symptoms include:
Gastrointestinal symptoms: Common gastrointestinal symptoms include chronic diarrhoea, abdominal pain, bloating, and gas. Many individuals may also experience nausea and vomiting. These symptoms result from the body’s inability to properly absorb nutrients due to damage in the intestinal lining.
Nutritional deficiencies: Coeliac disease can lead to malabsorption of essential nutrients, resulting in deficiencies. Symptoms may include fatigue, weakness, anaemia (often iron-deficiency anaemia), and osteoporosis due to calcium and vitamin D malabsorption.
Skin conditions: Some individuals develop dermatitis herpetiformis, an itchy, blistering rash associated with coeliac disease. This rash often appears on the elbows, knees, and buttocks and improves with a gluten-free diet.
Neurological symptoms: Coeliac disease may also present with neurological symptoms, including headaches, migraines, peripheral neuropathy (tingling or numbness in the limbs), and difficulties with concentration or memory, sometimes referred to as "brain fog."
Reproductive issues: Women with coeliac disease may experience reproductive challenges, including irregular menstrual cycles, infertility, or complications during pregnancy.
Growth delays in children: In children, coeliac disease can lead to delayed growth and development, including short stature and delayed puberty. This is often due to malnutrition resulting from nutrient absorption issues.
Behavioural changes: Some individuals, particularly children, may exhibit behavioural changes such as irritability, mood swings, or anxiety, which can be related to nutrient deficiencies or the impact of the disease itself.
Recognising these symptoms is crucial for early diagnosis and effective management through a strict gluten-free diet.
How Does Coeliac Disease Sprue Affect Your Body?
Coeliac disease sprue primarily affects the small intestine, damaging the villi responsible for nutrient absorption. When an individual with coeliac disease consumes gluten, their immune system overreacts, causing injury to the villi and impairing the absorption of vital nutrients. This malabsorption can lead to various health problems, including malnutrition, weakened bones, mood changes, and reproductive issues. The disease can develop at any age, and its impact on the body can vary significantly among affected individuals.
Coeliac Disease Sprue in Children
In children, coeliac disease sprue may present with different symptoms compared to adults. Common manifestations in children include abdominal bloating and pain, chronic diarrhoea, constipation, failure to thrive, fatigue, gas, headaches, and irritability. Children with coeliac disease may also have pale, foul-smelling stools. Additionally, they may experience delayed puberty, short stature, and tooth enamel defects. Early diagnosis and strict adherence to a gluten-free diet are essential for children with coeliac disease sprue to prevent long-term complications and ensure proper growth and development.
Stages of Coeliac Disease Sprue
The progression of coeliac disease can be categorised into several stages based on the extent of intestinal damage, often assessed using the Marsh Score system (ACG Clinical Guidelines, 2023). These stages include:
Stage 0 (Marsh 0): Normal biopsy with no villous changes.
Stage 1 (Marsh 1 – Increased intraepithelial lymphocytes): Shows increased intraepithelial lymphocytes (IELs) in the intestinal lining. Villous structure remains normal. This can occur in early coeliac disease or other conditions (infection, autoimmune disease, IBS).
Stage 2 (Marsh 2 – Crypt hyperplasia): Shows increased IELs and crypt hyperplasia (elongation of crypts indicating mucosal stress).
Stage 3 (Marsh 3 – Villous atrophy): Villous flattening with crypt hyperplasia and increased IELs.
- Stage 3a: Mild villous atrophy
- Stage 3b: Moderate villous atrophy
- Stage 3c: Severe villous atrophy
Stage 3 correlates with nutrient malabsorption symptoms and may be seen in patients with dermatitis herpetiformis.
Causes of Coeliac Disease Sprue
Coeliac disease sprue is caused by an immune reaction to gluten, a protein found in wheat, barley, rye, and sometimes oats. The exact cause is not fully understood, but it involves the following factors:
Genetic factors: Individuals with a family history of coeliac disease are at a higher risk of developing the condition.
Environmental triggers: Consumption of gluten triggers an autoimmune response that damages the villi in the small intestine, leading to malabsorption of nutrients.
When gluten is consumed, the immune system of a person with coeliac disease reacts by attacking the villi, which are crucial for nutrient absorption. This leads to a range of complications that can affect various parts of the body.
Risk Factors
Several factors can increase the risk of developing coeliac disease, including:
- Family history
- People with other autoimmune conditions, such as type 1 diabetes, autoimmune thyroid disease, and Addison's disease
- Individuals with genetic disorders, such as Down syndrome and Turner syndrome
- Certain genetic variations, particularly in the HLA-DQ2 and HLA-DQ8 genes (ACG Clinical Guidelines, 2023)
- Age (most commonly diagnosed between 40 and 60 years, but can occur at any age)
While having these risk factors does not necessarily mean you will develop coeliac disease, being aware of them can help with early detection and management.
Complications
If coeliac disease is left untreated or poorly managed, it can lead to various complications that include:
Malnutrition: Damage to the small intestine can result in malabsorption of essential nutrients, such as iron, folate, calcium, and vitamin D, leading to deficiencies and related health problems.
Osteoporosis: Malabsorption of calcium and vitamin D can lead to reduced bone mineral density, increasing the risk of osteoporosis and fractures.
Infertility and miscarriage: Untreated coeliac disease may contribute to reproductive issues, such as infertility, recurrent miscarriages, and low birth weight babies.
Neurological problems: Some people with coeliac disease may experience neurological symptoms, such as peripheral neuropathy, ataxia (impaired coordination), and epilepsy.
Lactose intolerance: Damage to the small intestine can cause temporary lactose intolerance, leading to bloating, diarrhoea, and abdominal pain after consuming dairy products.
Intestinal cancers: Although rare, people with coeliac disease have a slightly increased risk of developing intestinal lymphoma and small bowel cancer.
Diagnosis & Tests
Diagnosing coeliac disease typically involves a combination of clinical evaluation, blood tests, and intestinal biopsy. The tests may include:
- Serological tests: Blood tests are used to detect specific antibodies associated with coeliac disease. The first-line test is the tissue transglutaminase IgA (tTG-IgA) test.
Total serum IgA must be measured at the same time, because 2–3% of people with coeliac disease have IgA deficiency, which can lead to false-negative results on IgA-based tests. If total IgA is low/deficient, clinicians should instead use IgG-based tests, such as IgG-DGP (deamidated gliadin peptide) or IgG-tTG, to improve diagnostic accuracy ESPGHAN (2020). Additional confirmatory tests may include endomysial antibody (EMA) testing.
- Genetic testing: Genetic tests can be used to detect the presence of HLA-DQ2 and HLA-DQ8 genes, which are found in most people with coeliac disease. However, having these genes does not necessarily mean an individual will develop coeliac disease (ACG Clinical Guidelines, 2023).
- Intestinal biopsy: If blood tests and clinical evaluation suggest coeliac disease, an intestinal biopsy is usually performed to confirm the diagnosis. During this procedure, small tissue samples are taken from the small intestine to be examined under a microscope for damage to the villi (small, finger-like projections lining the intestine).
Do not start a gluten-free diet (GFD) before diagnostic testing unless directed; in selected children with very high tTG IgA and positive EMA, ESPGHAN provides criteria for a biopsy-sparing diagnosis ESPGHAN (2020). However, it is crucial to consult a doctor before starting a gluten-free diet, as it can affect the accuracy of diagnostic tests.
Treatment & Management
The treatment of coeliac disease is personalised based on symptom severity, degree of intestinal damage, nutritional status, and the presence of extra-intestinal manifestations. A multidisciplinary approach is often employed, involving dietary modification, anti-inflammatory agents, and targeted therapies to relieve symptoms, promote intestinal healing, and manage associated conditions.
1. Glucocorticoids
Glucocorticoids may be required in refractory coeliac disease where the intestine does not heal despite dietary adherence.
- Prednisolone: It reduces inflammation in the small intestine and supports nutrient absorption in patients not responding to a gluten-free diet alone.
2. Anti-Inflammatory Agents
Used in cases where coeliac disease presents with associated skin conditions like dermatitis herpetiformis.
- Dapsone: It provides rapid relief from the severe itching and blistering caused by dermatitis herpetiformis, although a gluten-free diet remains essential.
3. Immunomodulators
Immunosuppressive therapy is occasionally necessary in rare, resistant cases of coeliac disease, particularly type II refractory coeliac.
- Infliximab: It is a monoclonal antibody that blocks TNF-α to reduce persistent intestinal inflammation in severe, treatment-resistant cases.
4. Strict Gluten-Free Diet
This forms the cornerstone of long-term management in coeliac disease.
- Gluten-Free Diet: The complete elimination of wheat, rye, and barley allows the intestinal mucosa to heal, alleviates gastrointestinal symptoms, and prevents further immune system activation.
5. Nutritional Support and Supplementation
Due to malabsorption, many individuals require dietary supplementation to restore nutritional balance.
- Iron: Corrects iron-deficiency anaemia due to chronic intestinal inflammation.
- Calcium and Vitamin D: Support bone health and reduce the risk of osteoporosis.
- Vitamin B12 and Folate: Help restore energy levels and improve neurological function affected by deficiencies.
6. Label Reading and Food Safety
Ongoing education in identifying gluten sources and preventing cross-contamination is essential for long-term success.
- Label Reading: Involves checking food labels and product ingredients for hidden gluten.
- Food Safety: This includes avoiding cross-contact in shared kitchens and verifying the gluten-free status of medications and personal care items.
Living with Disease
Living with coeliac disease sprue involves several important considerations, including:
Adherence to a gluten-free diet is key to managing coeliac disease sprue. This heals the damage to the villi in the small intestine and prevents further damage.
Seek help from a registered dietitian who specialises in coeliac disease to ensure a balanced and nutritious diet.
Be aware of hidden sources of gluten in foods, medicines, and non-food products.
Read labels carefully to identify ingredients that may contain gluten.
Communicate your dietary needs to friends, family, and restaurant staff to avoid accidental gluten exposure.
Join support groups or online communities to connect with others who have coeliac disease sprue and share experiences and tips.
When to See a Doctor?
If you experience persistent digestive symptoms, such as diarrhoea, abdominal pain, bloating, or unexplained weight loss, consult your doctor. These symptoms may indicate coeliac disease sprue or another digestive disorder. Additionally, if you have been diagnosed with coeliac disease sprue and your symptoms persist or worsen despite following a strict gluten-free diet, consult your doctor to rule out other potential causes or complications.
Key Takeaways
Coeliac disease sprue is an autoimmune disorder triggered by the consumption of gluten, a protein found in wheat, barley, rye, and triticale.
Common symptoms include chronic diarrhoea, abdominal pain, bloating, and unexplained weight loss, but some individuals may be asymptomatic.
The only effective treatment for coeliac disease is a strict, lifelong gluten-free diet, which helps heal the small intestine and alleviate symptoms.
Regular follow-up with doctors, dietary counselling, and nutritional monitoring are essential for managing coeliac disease successfully.
Early diagnosis and treatment are crucial to prevent complications and improve quality of life.
FAQs
What is the life expectancy of individuals with coeliac disease?
People with coeliac disease can generally expect a normal lifespan if they adhere to a strict gluten-free diet, although there may be a slightly increased mortality risk.
What damage does coeliac disease cause to the body?
Coeliac disease causes inflammation and damages the small intestine's villi, impairing nutritional absorption. If untreated, it can lead to anaemia, osteoporosis, and other complications.
What is gluten enteropathy or coeliac sprue?
Gluten enteropathy and coeliac sprue are alternative names for coeliac disease, characterised by an immune reaction to gluten that damages the small intestine.
What foods should coeliacs avoid?
Those with coeliac disease must avoid foods containing gluten, such as wheat (including varieties like spelt and kamut), barley, rye, and triticale.
Does coeliac ever go away?
Coeliac disease is a lifelong condition that does not go away but can be effectively managed by following a gluten-free diet.
Can the effects of coeliac disease be reversed?
While intestinal damage caused by coeliac disease can heal with a strict gluten-free diet, the condition itself is not reversible, and continued gluten exposure will cause symptoms to recur.
Can coeliacs live a normal life?
People with coeliac disease can lead a normal life by carefully managing their diet and avoiding gluten-containing foods, which helps prevent symptoms and complications.
What is coeliac disease most often caused by?
Coeliac disease is an autoimmune disorder triggered by the ingestion of gluten in genetically predisposed individuals, leading to an immune reaction that damages the small intestine.
What is the best treatment for coeliac disease?
The best treatment for coeliac disease is a lifelong adherence to a strict gluten-free diet, which allows the small intestine to heal and prevents further damage.
Can you recover from coeliac disease?
While the small intestine can heal and symptoms can resolve with a gluten-free diet, coeliac disease is a chronic condition that requires lifelong management through dietary changes.
References
- Khaouli, M., Verdu, E. F., & Pinto, I. (2023). Exploring novel therapies for coeliac disease: are safe drugs tolerable? The Lancet Gastroenterology & Hepatology, 8(8), 688–689. https://doi.org/10.1016/s2468-1253(23)00112-7
- Schuppan, D., Mäki, M., Lundin, K. E. A., Isola, J., Friesing-Sosnik, T., Taavela, J., Popp, A., Koskenpato, J., Langhorst, J., Hovde, Ø., Lähdeaho, M.-L., Fusco, S., Schumann, M., Török, H. P., Kupcinskas, J., Zopf, Y., Lohse, A. W., Scheinin, M., Kull, K., & Biedermann, L. (2021). A Randomized Trial of a Transglutaminase 2 Inhibitor for Celiac Disease. New England Journal of Medicine, 385(1), 35–45. https://doi.org/10.1056/nejmoa2032441
- Husby, S., Koletzko, S., Korponay-Szabó, I., Kurppa, K., Mearin, M. L., Ribes-Koninckx, C., Shamir, R., Troncone, R., Auricchio, R., Castillejo, G., Christensen, R., Dolinsek, J., Gillett, P., Hróbjartsson, A., Koltai, T., Maki, M., Nielsen, S. M., Popp, A., Bucharest, & Størdal, K. (2019). European Society Paediatric Gastroenterology, Hepatology and Nutrition Guidelines for Diagnosing Coeliac Disease 2020. Journal of Pediatric Gastroenterology and Nutrition, 70(1), 1. https://doi.org/10.1097/mpg.0000000000002497
- Rubio-Tapia, A., Hill, I. D., Semrad, C., Kelly, C. P., & Lebwohl, B. (2022). American College of Gastroenterology Guidelines Update: Diagnosis and Management of Celiac Disease. American Journal of Gastroenterology, 118(1), 59–76. https://doi.org/10.14309/ajg.0000000000002075
Browse Other Conditions
Latest health articles
Top Health Essentials
Disclaimer
Top-Selling Medicines:
...View more
Top-OTC medicines:
...View more
Company
About UsHealth ArticleHealth StoriesHealth LibraryDiseases & Health ConditionsAyurvedaUnderstanding Generic MedicinesAll MedicinesAll BrandsNeed HelpFAQSecuritySavings CalculatorSubscribe
Registered Office Address
Grievance Officer
Download Truemeds
Contact Us
Our customer representative team is available 7 days a week from 9 am - 9 pm.
v4.25.6
2026 - Truemeds | All rights reserved. Our content is for informational purposes only. See additional information.
Our Payment Partners










































