Prolactinoma
Prolactinoma is a benign tumour of the pituitary gland that produces excessive amounts of the hormone prolactin. It is the most common type of pituitary tumour and can cause symptoms such as infertility, irregular periods, and decreased libido. Treatment options include medication, surgery, and radiation therapy, depending on the size and severity of the tumour.
Last updated on : 06 May, 2026
Read time : 13 mins
Overview of Disease
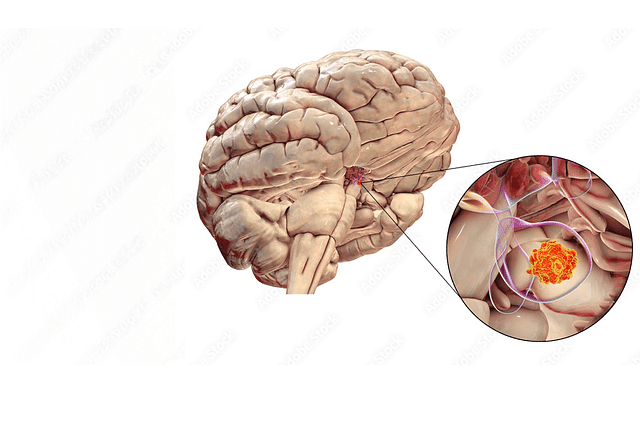
Prolactinoma is a noncancerous tumour that develops in the pituitary gland, a small endocrine gland situated at the base of the brain. The pituitary gland regulates various bodily functions, including hormone production.
Among all pituitary adenomas, prolactinoma is the most prevalent, accounting for roughly 40% of cases (Yatavelli & Bhusal, 2023).
Understanding the nature of prolactinoma is essential for those affected by this condition.
What is Prolactinoma?
Prolactinoma is a tumour that arises from the abnormal growth of lactotroph cells in the pituitary gland, which are responsible for producing the hormone prolactin. Normally, prolactin stimulates milk production in women during pregnancy and breastfeeding.
However, in individuals with prolactinoma, the tumour cells secrete excessive amounts of prolactin, leading to hyperprolactinemia. This hormonal imbalance can cause various symptoms, such as infertility, irregular menstrual periods, and milky nipple discharge in women, as well as erectile dysfunction, decreased libido, and infertility in men.
Although the precise cause of prolactinoma remains unclear, genetic mutations and hormonal imbalances may play a role in its development. In some cases, prolactinoma may be associated with familial syndromes like multiple endocrine neoplasia type 1 (MEN1).
As we delve further into the classification of prolactinomas, it becomes evident that their size and secretory status can significantly affect presentation and management.
Key Factors about Prolactinoma
| Category | Details |
| Also Referred as | Pituitary adenoma, Microprolactinoma, Macroprolactinoma |
| Commonly Occurs In | More common in women than in men, particularly in individuals under 40 years of age |
| Affected Organ | Pituitary gland |
| Type | Benign (noncancerous) tumour |
| Common Signs | Women: Irregular menstruation, galactorrhoea, infertility, vaginal dryness Men: Erectile dysfunction, low testosterone, infertility Both: Vision problems, headaches, osteoporosis |
| Consulting Specialist | Endocrinologist |
| Treatement Procedures | Medication (dopamine agonists), Surgery, Radiation therapy |
| Managed By | Bromocriptine, cabergoline (dopamine agonists) |
| Mimiciking Condition | Hyperprolactinaemia from other causes (medications, thyroid issues, etc.) |
Types of Prolactinoma
Prolactinomas are primarily classified into two types based on their size: (Prolactinoma, 2025)
- Microprolactinoma: These are small tumours measuring less than 10 mm in diameter. Microprolactinomas are the most common type of prolactinoma and are often asymptomatic, meaning they may not cause noticeable symptoms.
- Macroprolactinoma: These tumours are larger than 10 mm in diameter. Due to their size and location, macroprolactinomas can cause compressive symptoms such as headaches, visual field defects, and cranial nerve palsy.
In some instances, prolactinomas may be further categorised into:
- Giant prolactinoma: These tumours exceed 4 cm in diameter and can cause significant compressive symptoms.
- Mixed tumours: These tumours secrete multiple hormones, including prolactin, and may require a more complex treatment approach.
The classification of prolactinomas by size and secretory status is crucial for determining the most appropriate treatment strategy, which may include medication, surgery, or radiation therapy. By understanding the different types of prolactinomas, healthcare professionals can provide targeted care to manage symptoms and improve patient outcomes.
Symptoms of Prolactinoma
The symptoms of prolactinoma can vary depending on the individual, the size of the tumour, and prolactin levels. Some common symptoms include:
- Infertility: High prolactin levels can interfere with the production of sex hormones, leading to fertility issues in both men and women.
- Bone loss (osteoporosis): Reduced levels of estrogen and testosterone can weaken bones and increase the risk of osteoporosis.
- Loss of interest in sexual activity: Both men and women may experience a decrease in libido due to hormonal imbalances caused by the tumour.
In addition to these general symptoms, there are also gender-specific symptoms that can occur.
Symptoms in Women
Women with prolactinoma may experience the following symptoms:
- Irregular or absent menstrual periods: High prolactin levels can disrupt the menstrual cycle, causing irregular periods or amenorrhea (absence of menstruation).
- Milky discharge from the breasts (galactorrhoea): This is a common symptom in women who are not pregnant or breastfeeding.
- Painful intercourse: Low estrogen levels can lead to vaginal dryness, causing discomfort during sexual intercourse.
- Acne and excessive body and facial hair growth: Some women may experience hirsutism (excessive hair growth) and acne due to hormonal imbalances.
These symptoms can be distressing for women and may have a significant impact on their quality of life. However, prolactinoma treatment can help alleviate these symptoms and restore hormonal balance.
Symptoms in Men
Men with prolactinoma may experience the following symptoms:
- Erectile dysfunction: High prolactin levels can cause difficulties in achieving or maintaining an erection, as well as decreased libido.
- Decreased body and facial hair: Low testosterone levels can lead to reduced hair growth on the body and face.
- Smaller muscles: Testosterone deficiency can lead to muscle atrophy and decreased muscle mass.
- Enlarged breasts (gynecomastia): Elevated prolactin levels can cause breast tissue enlargement in men.
These symptoms may affect a man's self-esteem and confidence. Seeking prompt medical attention and appropriate prolactinoma treatment can help manage these symptoms effectively.
Symptoms Due to Tumour Size and Location
In some cases, the size and location of the prolactinoma can cause additional symptoms, such as:
- Vision problems: Large prolactinomas can press on the optic nerve or optic chiasm, causing vision issues like loss of peripheral vision.
- Headaches: Pressure from the tumour can lead to headaches, which may be severe or persistent.
- Low levels of other pituitary hormones: Larger tumours can compress the healthy part of the pituitary gland, reducing the production of other essential hormones, such as thyroid hormones and cortisol.
These symptoms can be more severe and may require urgent medical attention. Regular monitoring of the tumour size and hormone levels is crucial for individuals with prolactinoma to prevent complications and ensure timely intervention when necessary.
Stages of Prolactinoma
Prolactinomas are not classified into stages. Prolactinomas are clinically classified based on tumour size and behaviour, which helps guide diagnosis and management.
Causes of Prolactinoma
The exact cause of prolactinoma remains poorly understood, but several factors and conditions have been identified as potential contributors to its development.
- Genetic Factors: Most prolactinomas occur sporadically, but a small percentage are attributable to genetic predisposition. Familial cases are rare but can occur as part of multiple endocrine neoplasia type 1 (MEN1) or other familial syndromes.
- Hormonal Influence: The exact cause of prolactinoma remains unclear. It is believed to result from genetic mutations that disrupt the normal function of the pituitary gland cells. These mutations lead to uncontrolled growth and prolactin secretion.
- Other Factors: Some prolactinomas may be influenced by external factors such as certain medications (e.g., antipsychotics, antidepressants), stress, and thyroid disorders. These factors do not cause prolactinomas but may lead to secondary hyperprolactinaemia, which can mimic prolactinoma.
Understanding the potential role of these factors can help in the diagnosis and management of prolactinoma.
Risk Factors
Prolactinomas are more common in women than in men and are rare in children. Women of reproductive age are more likely to be diagnosed earlier due to symptoms such as irregular menstrual periods. In contrast, postmenopausal women and men may be diagnosed later when tumours are larger and cause more noticeable symptoms like headaches and vision problems.
Rarely, inherited disorders such as multiple endocrine neoplasia type 1 (MEN1) and familial isolated pituitary adenoma (FIPA) can increase the risk of developing a prolactinoma. However, in most cases, there are no clear risk factors, and the tumours develop sporadically.
Complications
Prolactinomas can lead to several complications if left untreated or not managed properly:
- Vision Problems: Large prolactinomas can put pressure on the optic nerves, leading to vision difficulties such as double vision, a narrowed field of vision, or even loss of peripheral vision.
- Infertility: Excess prolactin can disrupt the reproductive system, leading to hypogonadism. In women, this can cause irregular or no menstrual periods, anovulation, and infertility. In men, it can result in decreased sperm production, erectile dysfunction, and reduced testosterone levels.
- Bone Loss (Osteoporosis): Decreased levels of oestrogen and testosterone due to high prolactin levels can lead to weakened, brittle bones, increasing the risk of osteoporosis.
- Hormonal Imbalance: Large prolactinomas can compress the pituitary gland, interfering with the production and release of other essential hormones such as thyroid hormones and cortisol.
- Pregnancy Complications: During pregnancy, increased oestrogen levels may lead to tumour enlargement, particularly in untreated macroprolactinomas; therefore, close monitoring is required.
- Galactorrhea: The most common symptom is the production of breast milk in men or in women who are not pregnant or breastfeeding.
Addressing these complications is a key focus of prolactinoma treatment. Medication aimed at reducing prolactin levels is often the first line of treatment to alleviate symptoms and prevent further complications.
Prevention of Prolactinoma
While the exact causes of prolactinoma are not fully understood, making prevention challenging, some steps can be taken to reduce the risk of complications associated with this condition.
Managing medications that can lead to elevated prolactin levels, such as certain antipsychotics and high blood pressure medications, is one way to help prevent hyperprolactinemia, a key symptom of prolactinomas.
For individuals with familial syndromes like multiple endocrine neoplasia type 1 (MEN1), which increases the risk of developing prolactinomas, close monitoring is essential. Regular check-ups and screenings for those with a family history of pituitary tumours can facilitate early detection and timely treatment.
Although prevention may not always be possible, early diagnosis through awareness of prolactinoma symptoms is crucial for effective management and the prevention of long-term complications.
Diagnosis & Tests
Diagnosing a prolactinoma involves a multi-faceted approach:
- Physical Exam and Medical History: The first step is a thorough physical examination and review of the patient's medical history to identify any symptoms or signs suggestive of a prolactinoma.
- Blood Tests: Laboratory tests measure prolactin levels. Consistently high prolactin levels are a strong indicator of a prolactinoma. Other hormonal tests may also be performed to assess pituitary function and rule out other potential causes of high prolactin levels.
- Imaging Tests: If blood tests reveal elevated prolactin levels, imaging tests such as an MRI (magnetic resonance imaging) or CT (computed tomography) scan of the brain are used to visualise the pituitary gland and detect a tumour. These scans can also help determine the size and location of the tumour.
- Visual Field Test: For larger prolactinomas that may be compressing the optic nerves, a visual field test may be performed to assess any impact on vision.
A combination of these diagnostic tools allows healthcare professionals to accurately diagnose a prolactinoma and develop an appropriate treatment plan tailored to the individual patient's needs.
Treatment & Management
Prolactinoma is managed through medication, surgery, and radiation therapy. The choice of treatment depends on tumour size, symptoms, and response to therapy.
1. Medication for Prolactinoma
The primary treatment for prolactinoma involves dopamine agonists, which reduce prolactin levels and shrink the tumour.
- Cabergoline: Cabergoline is a long-acting dopamine agonist preferred due to its efficacy and fewer side effects. It is typically the first-line medication.
- Bromocriptine: Bromocriptine is another dopamine agonist used when cabergoline is not tolerated. It requires more frequent dosing and has a higher side-effect profile compared to cabergoline.
- Quinagolide: Quinagolide is an alternative dopamine agonist, particularly for patients who do not tolerate cabergoline or bromocriptine.
2. Surgery
When medication fails to control prolactin levels or when the tumour exerts pressure on surrounding structures, transsphenoidal surgery may be required. The surgery involves accessing the pituitary gland through the nasal cavity to remove the tumour while attempting to preserve normal pituitary function. However, tumour recurrence is possible, and some patients may still need medication after surgery to regulate prolactin levels.
3. Radiation Therapy
For aggressive or recurrent prolactinomas, radiation therapy may be necessary, particularly in cases where the tumour continues to grow despite medication and surgery, malignant prolactinomas, or patients who cannot undergo surgery.
Living with Disease
Living with a prolactinoma requires ongoing management and monitoring. Patients often need long-term treatment with dopamine agonists to prevent the tumour from growing back. Regular follow-up appointments with an endocrinologist are crucial to monitor prolactin levels and tumour size.
If the tumour shrinks significantly and prolactin levels remain normal for at least two years, the medication may be tapered off under medical supervision. However, prolactin levels can rise again after stopping the medication, necessitating its restart. During pregnancy, special precautions are needed, and close collaboration between the endocrinologist and obstetrician is essential to ensure the safety of both the mother and the developing fetus.
Emotional support from family, friends, and support groups can be invaluable in coping with the challenges of living with a prolactinoma.
When to See a Doctor?
It is important to consult a healthcare professional if you experience symptoms suggestive of a prolactinoma, such as persistent headaches, vision changes, irregular menstrual cycles, infertility, or milky nipple discharge (galactorrhoea). Other conditions may also cause these symptoms, so a proper diagnosis is crucial. If you have been diagnosed with a prolactinoma, you should see your endocrinologist regularly to monitor your prolactin levels and tumour size. Any changes in your symptoms, such as worsening headaches or vision problems, should prompt an immediate medical evaluation. Additionally, if you are planning to become pregnant or are currently pregnant, it is essential to discuss your condition with your healthcare provider to ensure appropriate management and monitoring throughout your pregnancy.
Key Takeaways
- Prolactinomas are benign tumours of the pituitary gland that cause excess production of the prolactin hormone.
- Common prolactinoma symptoms include irregular menstrual periods, infertility, and milky discharge from the breasts in women, and low libido, erectile dysfunction, and infertility in men.
- Prolactinomas are usually diagnosed through blood tests measuring prolactin levels and brain imaging scans like MRI.
- Treatment for prolactinomas typically involves medications called dopamine agonists, such as cabergoline and bromocriptine, which reduce prolactin production.
- Surgery to remove the tumour may be considered if medications are ineffective or not tolerated, or if the tumour is large and pressing on surrounding brain structures.
- Regular monitoring with blood tests and periodic MRI scans is important to assess treatment response and check for any tumour regrowth.
- With appropriate prolactinoma treatment, symptoms usually improve, and the tumour often shrinks in size, allowing restoration of regular menstrual cycles and fertility in women.
- Most people with prolactinomas have an excellent prognosis and can lead normal lives with medical therapy; the medications are generally well-tolerated and effective in controlling the disease.
FAQs
What exactly is a prolactinoma?
Is it possible to cure a prolactinoma completely?
What are the common symptoms experienced with a prolactinoma?
What are the signs of elevated prolactin levels?
What causes high prolactin levels in unmarried women?
Can a prolactinoma be malignant?
What are some natural ways to lower prolactin levels?
How quickly do prolactinomas typically grow?
Is it possible for high prolactin levels to return to normal?
Can stress contribute to the development of a prolactinoma?
References
- Drummond, J. B., Molitch, M. E., & Korbonits, M. (2025, April 9). Prolactinoma management. Endotext - NCBI Bookshelf. https://www.ncbi.nlm.nih.gov/books/NBK279174/
- Petersenn, S., Fleseriu, M., Casanueva, F. F., Giustina, A., Biermasz, N., Biller, B. M. K., Bronstein, M., Chanson, P., Fukuoka, H., Gadelha, M., Greenman, Y., Gurnell, M., Ho, K. K. Y., Honegger, J., Ioachimescu, A. G., Kaiser, U. B., Karavitaki, N., Katznelson, L., Lodish, M., . . . Melmed, S. (2023). Diagnosis and management of prolactin-secreting pituitary adenomas: a Pituitary Society international Consensus Statement. Nature Reviews Endocrinology, 19(12), 722–740. https://doi.org/10.1038/s41574-023-00886-5
- Recent advances in the tumorigenic mechanism and clinical management of pituitary tumors. (2021, May 18). Frontiers Research Topic. https://www.frontiersin.org/research-topics/22096/recent-advances-in-the-tumorigenic-mechanism-and-clinical-management-of-pituitary-tumors/magazine
- Yatavelli, R. K. R., & Bhusal, K. (2023c, July 31). Prolactinoma. StatPearls - NCBI Bookshelf. https://www.ncbi.nlm.nih.gov/books/NBK459347/
- Prolactinoma. (2025, August 12). National Institute of Diabetes and Digestive and Kidney Diseases. https://www.niddk.nih.gov/health-information/endocrine-diseases/prolactinoma
Check Related Salts
Browse Other Conditions
Latest health articles
Top Health Essentials
Disclaimer
Top-Selling Medicines:
...View more
Top-OTC medicines:
...View more
Company
About UsHealth ArticleHealth StoriesHealth LibraryDiseases & Health ConditionsAyurvedaUnderstanding Generic MedicinesAll MedicinesAll BrandsNeed HelpFAQSecuritySavings CalculatorSubscribe
Registered Office Address
Grievance Officer
Download Truemeds
Contact Us
Our customer representative team is available 7 days a week from 9 am - 9 pm.
v4.25.6
2026 - Truemeds | All rights reserved. Our content is for informational purposes only. See additional information.
Our Payment Partners










































