Knee Bursitis
Knee bursitis is a painful condition caused by inflammation of the bursae, small fluid-filled sacs that cushion the knee joint. Prepatellar bursitis, a common type of knee bursitis, occurs when the bursa in front of the kneecap becomes inflamed. Treatment for knee bursitis depends on whether it is traumatic, overuse-related, crystal-related, or infectious. Most non-infectious cases improve with rest, ice, activity modification, NSAIDs, and physical therapy. Septic bursitis requires urgent medical evaluation and antibiotics.
Last updated on : 23 Apr, 2026
Read time : 12 mins
Overview of Disease
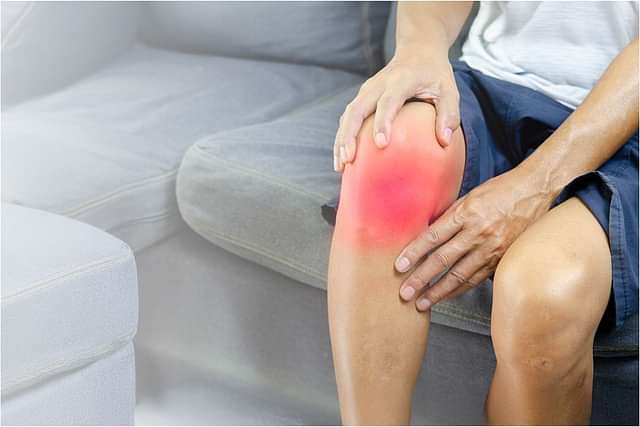
Knee bursitis is a common condition that can cause significant discomfort and limit mobility. It occurs when the small, fluid-filled sacs called bursae, which act as cushions between bones, tendons, and muscles, become inflamed. This inflammation can be caused by repetitive motion, injury, or infection. In this blog post, we will explore the causes, symptoms, and treatment options for knee bursitis, with a focus on prepatellar bursitis, a specific type of knee bursitis affecting the front of the kneecap.
What is Prepatellar Bursitis?
Prepatellar bursitis, also known as “housemaid's knee” or “carpenter's knee”, is a condition that occurs when the bursa located in front of the kneecap (patella) becomes inflamed. This bursa acts as a cushion between the kneecap and the skin, reducing friction and preventing irritation (Rishor-Olney et al., 2024). When the prepatellar bursa becomes inflamed, it can cause swelling, pain, and tenderness in the front of the knee.
Prepatellar bursitis is often caused by repetitive kneeling, which puts pressure on the bursa and can lead to inflammation over time. This is why the condition is commonly seen in individuals who frequently kneel for work or leisure activities, such as cleaners, carpenters, and gardeners. Other associated conditions include rheumatoid arthritis and gout; in these cases, bursitis results from systemic inflammation or crystal deposition rather than mechanical pressure alone. Symptoms of prepatellar bursitis may include swelling, pain, warmth, and redness in the affected area, as well as a limited range of motion in the knee. If left untreated, the condition can become chronic and lead to further complications. Fortunately, there are several effective knee bursitis treatment options available, which we will discuss in the following sections.
Key Factors about Knee Bursitis
| Category | Details |
| Also Referred to as |
|
| Commonly Occurs In |
|
| Affected Organ |
|
| Type |
|
| Common Signs |
|
| Consulting Specialist |
|
| Treatment Procedures |
|
| Managed By |
|
| Mimicking Condition |
|
Symptoms of Knee Bursitis
Knee bursitis is a condition characterised by the inflammation of the bursae around the knee joint. This inflammation can lead to a range of symptoms that may vary depending on the specific bursa affected and the underlying cause of the inflammation.
- Pain: One of the most common symptoms of knee bursitis is pain, especially when moving the knee or applying pressure to it. The pain may be localised to the affected area or radiate to the surrounding tissues.
- Swelling: Visible swelling and redness over the affected bursa are common findings, especially in prepatellar bursitis. The swelling may be more pronounced in certain types of bursitis, such as prepatellar bursitis, where the swelling occurs over the kneecap.
- Warmth: The affected area may feel warm to the touch, indicating the presence of inflammation.
- Tenderness: The affected area may be sensitive to touch or pressure, causing discomfort or pain.
- Limited mobility: In some cases, the pain and swelling associated with knee bursitis can lead to difficulty in moving the knee, limiting the range of motion and affecting daily activities.
In addition to these general symptoms, specific types of knee bursitis may present with unique signs. For example, pes anserine bursitis is more common in people with medial knee osteoarthritis, obesity, or altered lower-limb biomechanics, but it can occur in a wide range of individuals. Infectious bursitis may also present with additional symptoms such as fever, chills, and skin changes indicative of an infection.
Causes of Knee Bursitis
Prepatellar bursitis is a specific type of knee bursitis that affects the bursa located in front of the kneecap (patella). This condition can be caused by various factors, leading to inflammation, pain, and swelling in the affected area.
- Repeated pressure: One of the most common causes of prepatellar bursitis is frequent and prolonged kneeling, particularly on hard surfaces. This repeated pressure can irritate the bursa and lead to inflammation.
- Direct trauma: A direct blow to the knee, such as from a fall or impact during sports, can cause damage to the prepatellar bursa and trigger inflammation.
- Infection: Septic bursitis is caused by bacterial infection—most commonly Staphylococcus aureus entering through skin breaks—and presents with pronounced redness, warmth, fever, and significant tenderness. This requires urgent medical assessment and antibiotics (Darrieutort-Laffite et al., 2024).
Risk Factors
Prepatellar bursitis can affect individuals from various demographics and professions. Prepatellar bursitis occurs across all age groups; repetitive kneeling occupations are the strongest predictor (Rishor-Olney et al., 2024). Some studies report a higher incidence in adult men due to occupational exposure, but it is not limited to ages 40–60.
- Occupational risks: Individuals with jobs that involve frequent kneeling, such as plumbers, roofers, carpet layers, coal miners, gardeners, carpenters, and housemaids, are at higher risk of developing prepatellar bursitis.
- Athletes and sports: Athletes participating in sports that involve direct blows or falls on the knee, like football, wrestling, or basketball, are also at increased risk of knee bursitis.
- Underlying health conditions: People with chronic inflammatory diseases, such as rheumatoid arthritis or gout, and those with immunosuppressive conditions, like diabetes mellitus or chronic steroid use, are more susceptible to developing prepatellar bursitis.
Prevention of Knee Bursitis
Preventing knee bursitis involves taking steps to reduce pressure and friction on the knee joint.
- Using protective gear like kneepads can help if you work on your knees or participate in contact sports. Taking regular breaks to rest and stretch your knees is especially important if your job involves kneeling for long periods.
- Maintaining a healthy weight is another key factor in preventing prepatellar bursitis and other types of knee bursitis. Excess weight puts additional stress on the knee joints, increasing the risk of developing bursitis. Engaging in regular exercise and maintaining a balanced diet can help you achieve and maintain a healthy weight.
- Proper footwear may improve lower-limb alignment and reduce stress on knee structures, although its direct effect on preventing bursitis is less established. It can still be beneficial for overall knee mechanics. Choose shoes with good arch support and cushioning to absorb shock and reduce stress on the knees. Avoid high heels and shoes with minimal support, as they can put extra strain on the knee joints.
- Gradually increasing the intensity and duration of physical activities can help prevent overuse injuries that lead to knee bursitis. Avoid sudden increases in activity levels and allow your body time to adjust to new exercises or sports.
Diagnosis & Tests
Diagnosing prepatellar bursitis involves a combination of medical history, physical examination, and sometimes additional tests to determine the underlying cause and severity of the condition.
- Symptom assessment: During the consultation, the doctor will discuss the patient's symptoms, including the severity of pain, duration of symptoms, and any activities that exacerbate the knee symptoms.
- Physical examination: The doctor will inspect the affected knee, comparing it to the healthy knee, and check for tenderness, swelling, warmth, and range of motion. They will also assess for signs of infection, such as fever or chills.
- Imaging tests: X-rays may help rule out fractures or calcifications, but bursae themselves are not well visualised on X-ray. MRI or ultrasound can help support the diagnosis of bursitis and rule out soft-tissue injuries.
- Aspiration: If the bursitis is suspected to be caused by an infection, the doctor may perform an aspiration, which involves using a needle to remove fluid from the affected bursa for laboratory analysis (Brown et al., 2021).
Treatment & Management
The main objective in managing knee bursitis is to relieve inflammation, alleviate pain, restore joint mobility, and prevent recurrence. Early intervention with conservative measures is often effective, though persistent or severe cases may require medical treatment (Brown et al., 2021). Below are the key treatment strategies used to manage knee bursitis.
1. Anti-Inflammatory Medications
NSAIDs are commonly used for symptom relief in non-infectious bursitis, but should be used cautiously in people with kidney, cardiovascular, or gastrointestinal risk factors.
- Ibuprofen: Reduces inflammation and eases joint pain during flare-ups.
- Naproxen: Helps relieve stiffness and swelling by inhibiting prostaglandin synthesis.
- Acetaminophen (Paracetamol): Offers pain relief for patients who cannot tolerate NSAIDs due to gastrointestinal or cardiovascular risks.
2. Corticosteroid Injections
In cases where symptoms persist despite initial treatment or when inflammation is more severe, corticosteroid injections may be considered.
- Hydrocortisone: It provides local anti-inflammatory action when injected into the inflamed bursa.
- Triamcinolone: It is a potent corticosteroid that delivers long-lasting anti-inflammatory effects, making it suitable for managing persistent or severe knee bursitis.
- Methylprednisolone: It is commonly used for its strong and prolonged anti-inflammatory properties, particularly in cases where knee bursitis does not respond to milder treatments.
Corticosteroid injections help to:
- Provide rapid and localised symptom relief
- Reduce persistent swelling and pain
- Shorten recovery time in chronic or recurrent bursitis
- Avoid the need for systemic medication in isolated inflammation
3. Antibiotic Therapy
When bursitis is caused by an infection—known as septic bursitis—antibiotic treatment is essential. This is typically indicated if the area is red, warm, swollen, and accompanied by fever or pus drainage. Antibiotic selection for septic bursitis depends on severity and local resistance patterns. Empiric therapy often targets Staphylococcus aureus (including MRSA), using agents such as cephalosporins, clindamycin, doxycycline, or vancomycin for severe cases. Culture results should guide definitive therapy (Darrieutort-Laffite et al., 2024).
- Cephalosporins: Broad-spectrum antibiotics effective against common skin pathogens.
- Clindamycin: Often used for resistant or anaerobic bacterial infections.
- Vancomycin: Reserved for severe infections, especially those caused by MRSA.
4. RICE Therapy (Rest, Ice, Compression, Elevation)
This supportive approach is recommended in the early stages and throughout recovery from knee bursitis.
- Rest: Reduces repetitive stress on the bursa; avoid kneeling and impact activities.
- Ice: Apply for 15–20 minutes at a time, several times per day, ensuring a cloth barrier to prevent skin injury.
- Compression: Using elastic wraps or sleeves helps control swelling and support the joint.
- Elevation: Keeping the knee elevated above heart level encourages fluid drainage and decreases swelling.
5. Physical Therapy
Once acute inflammation is under control, physical therapy plays a crucial role in rehabilitation and long-term management.
- Strengthening Exercises: Focus on quadriceps, hamstrings, and hip muscles to support knee alignment and reduce stress on the bursa.
- Stretching and Mobility Work: Improve flexibility and joint range of motion to prevent stiffness.
- Postural and Gait Training: Address any biomechanical imbalances that may contribute to recurrent bursitis.
When to See a Doctor?
If you experience persistent knee pain, swelling, or stiffness that does not improve with home remedies, it is important to consult a doctor. Seek medical attention if you notice any of the following knee bursitis symptoms:
- Severe pain that limits your ability to move your knee
- Significant swelling or redness around the knee
- Fever, chills, rapidly increasing redness, or severe tenderness may indicate septic bursitis, requiring urgent medical evaluation.
- Inability to bear weight on the affected leg
- Visible lumps or deformities around the knee
Your doctor will perform a physical examination and may order imaging tests like X-rays or MRI scans to diagnose knee bursitis accurately. They will also help determine the underlying cause of your condition and recommend the most appropriate knee bursitis treatment based on the severity of your symptoms.
Early diagnosis and treatment can help prevent complications and promote faster recovery from knee bursitis. By working closely with your doctor and following their recommended treatment plan, you can effectively manage your symptoms and reduce the risk of recurrent episodes.
FAQs
What are the most effective ways to manage knee bursitis?
What are the three primary indicators of bursitis in the knee?
How much time does it take for knee bursitis to resolve?
What is the quickest method to alleviate bursitis?
Can individuals with knee bursitis continue walking?
Is bursitis a lifelong condition?
Can bursitis lead to significant health issues?
References
- Rishor-Olney, C. R., Taqi, M., & Pozun, A. (2024). Prepatellar bursitis. In StatPearls. StatPearls Publishing. https://www.ncbi.nlm.nih.gov/books/NBK557508/
- Brown, J. N., Brown, A., & Wilson, A. (2021). Management of septic and aseptic prepatellar bursitis: A systematic review. Archives of Orthopaedic and Trauma Surgery, 139(8), 1189-1199. https://pubmed.ncbi.nlm.nih.gov/33721054/
- Darrieutort-Laffite, C., Coiffier, G., Aïm, F., Banal, F., Bart, G., Chazerain, P., Couderc, M., Coquerelle, P., Ducourau Barbary, E., Flipo, R. M., Faudemer, M., Godot, S., Hoffmann, C., Lecointe, T., Lormeau, C., Mulleman, D., Piot, J. M., Senneville, E., Seror, R., ... Salliot, C. (2024). 2023 French recommendations for diagnosing and managing prepatellar and olecranon septic bursitis. Joint Bone Spine, 91(2), 105664. https://doi.org/10.1016/j.jbspin.2023.105664
- Beyde, A., Thomas, A. L., Colbenson, K. M., Sandefur, B. J., Kisirwan, I., Mullan, A. F., O'Driscoll, S. W., & Campbell, R. L. (2022). Efficacy of empiric antibiotic management of septic olecranon bursitis without bursal aspiration in emergency department patients. Academic Emergency Medicine, 29(1), 6-14. https://doi.org/10.1111/acem.14406
Browse Other Conditions
Latest health articles
Top Health Essentials
Disclaimer
Top-Selling Medicines:
...View more
Top-OTC medicines:
...View more
Company
About UsHealth ArticleHealth StoriesHealth LibraryDiseases & Health ConditionsAyurvedaUnderstanding Generic MedicinesAll MedicinesAll BrandsNeed HelpFAQSecuritySavings CalculatorSubscribe
Registered Office Address
Grievance Officer
Download Truemeds
Contact Us
Our customer representative team is available 7 days a week from 9 am - 9 pm.
v4.25.7
2026 - Truemeds | All rights reserved. Our content is for informational purposes only. See additional information.
Our Payment Partners










































